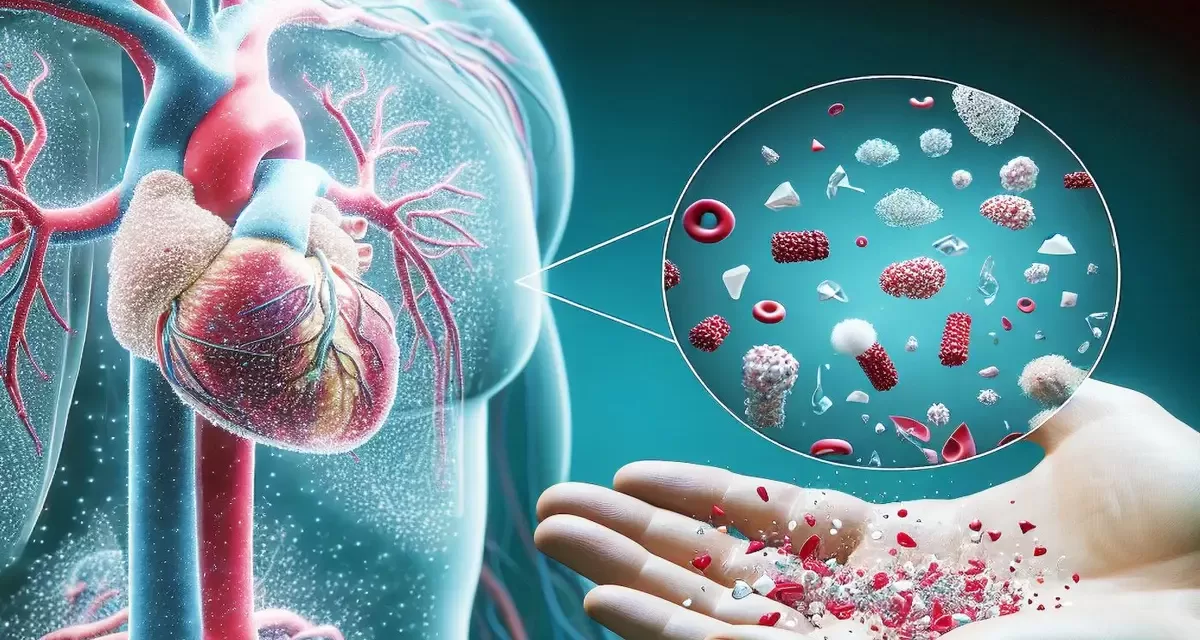
Researchers from the Chinese Academy of Sciences warn that viruses thriving on plastic debris in the environment—known as the plastisphere—may accelerate the global crisis of antibiotic resistance through gene transfer mechanisms. Published in the journal Biocontaminant on December 31, 2025, their perspective piece calls for urgent studies to quantify this overlooked risk, as plastics colonize oceans, rivers, and soils worldwide.
Key Findings from the Study
The plastisphere refers to the microbial biofilms that rapidly coat plastic waste, creating hotspots for antibiotic resistance genes (ARGs). Lead author Dong Zhu and colleagues, including Xue-Peng Chen and Di Wu, propose that viruses within these biofilms act as “hidden drivers” of ARG dissemination. They mediate horizontal gene transfer (HGT)—a process where genetic material jumps between bacteria without reproduction—facilitating the spread of resistance across species, including pathogens.
Viruses package ARGs during infection and deliver them to new bacterial hosts via transduction, a form of HGT that occurs more readily in the dense, packed biofilms of plastispheres. Additionally, some viruses encode auxiliary metabolic genes (AMGs) that enhance bacterial survival against antibiotics and pollutants, indirectly favoring resistant strains. Prior research detected 57 ARG subtypes in water plastisphere viromes, conferring resistance to 13 antibiotic classes.
Environmental context matters: In aquatic settings, lysogenic viruses (which integrate into host DNA) dominate, boosting HGT risks, while soil plastispheres favor lytic viruses that kill hosts, potentially curbing resistance.
Broader Context of Plastisphere Risks
Plastics have invaded ecosystems globally, with over 14 million tons entering oceans annually and microplastics detected in remote soils and air. These fragments provide stable surfaces that select for unique microbial communities, distinct from surrounding environments, with higher beta-diversity and deterministic assembly processes. Studies confirm plastispheres enrich ARGs—up to 12.4 times more potential pathogens than bulk soils—and mobile genetic elements that enable HGT.
Bacteria in plastispheres, like Pseudomonas and Bacillus, often carry multidrug resistance, exacerbated by plastic-adsorbed pollutants such as heavy metals and antibiotics. Viruses expand this threat by interacting with diverse prokaryotes, including Enterobacteriaceae and Vibrionaceae families linked to human infections. One study found closer virus-pathogen links in plastispheres than natural habitats, heightening “superbug” emergence risks.
This builds on earlier work showing biofilms as HGT hotspots, where ARG transfer rates exceed planktonic cultures. The plastisphere’s stressors—nutrient scarcity and toxins—prompt viruses to switch life cycles, adapting to promote host fitness and resistance.
Expert Perspectives
Dong Zhu, from the State Key Laboratory of Regional and Urban Ecology at the Chinese Academy of Sciences, emphasized, “Most research has focused on bacteria in the plastisphere, but viruses are everywhere in these communities and interact closely with their hosts. Our work suggests that plastisphere viruses may act as hidden drivers of antibiotic resistance dissemination.”
Dr. Elena Martinez, a microbiologist at the University of Barcelona not involved in the study, noted via email, “This perspective rightly shifts attention to viruses, which we’ve underestimated in plastic pollution dynamics. Their broad host ranges in biofilms could indeed amplify ARG mobility, but we need phage transplantation experiments to confirm transduction rates.”
Similarly, findings echo global concerns from the World Health Organization, which reports 1.27 million annual deaths from antibiotic-resistant infections, urging surveillance of environmental reservoirs like plastispheres.
Public Health Implications
This viral role in plastispheres could undermine antibiotic efficacy, as resistant pathogens hitchhike on drifting plastics to beaches, water supplies, and food chains. For consumers, it means everyday plastic use—from bottles to bags—contributes indirectly to resistance, potentially complicating treatments for common infections like UTIs or pneumonia.
Healthcare professionals face heightened challenges treating “superbugs” like multidrug-resistant Pseudomonas, prevalent in plastispheres. Practical steps include reducing single-use plastics, supporting phage therapy (viruses targeting resistant bacteria), and monitoring virus-host ratios in wastewater. For individuals, minimizing microplastic exposure via filtered water and natural fibers aids broader efforts, though direct health links remain under study.
Governments should integrate viral ecology into waste policies, prioritizing biodegradable alternatives less prone to ARG hotspots.
Limitations and Future Directions
The perspective acknowledges gaps: No direct measurements of ARG flux between plastisphere viruses and bacteria exist, and methodological biases—like bacterial DNA contamination in viromes—may inflate ARG estimates. Computational predictions of virus-host links need experimental validation, such as lab-based transduction assays.
Conflicting roles persist—lytic viruses might suppress ARGs by killing hosts—highlighting habitat-specific effects. Authors urge refined detection methods and field studies to assess real-world dissemination.