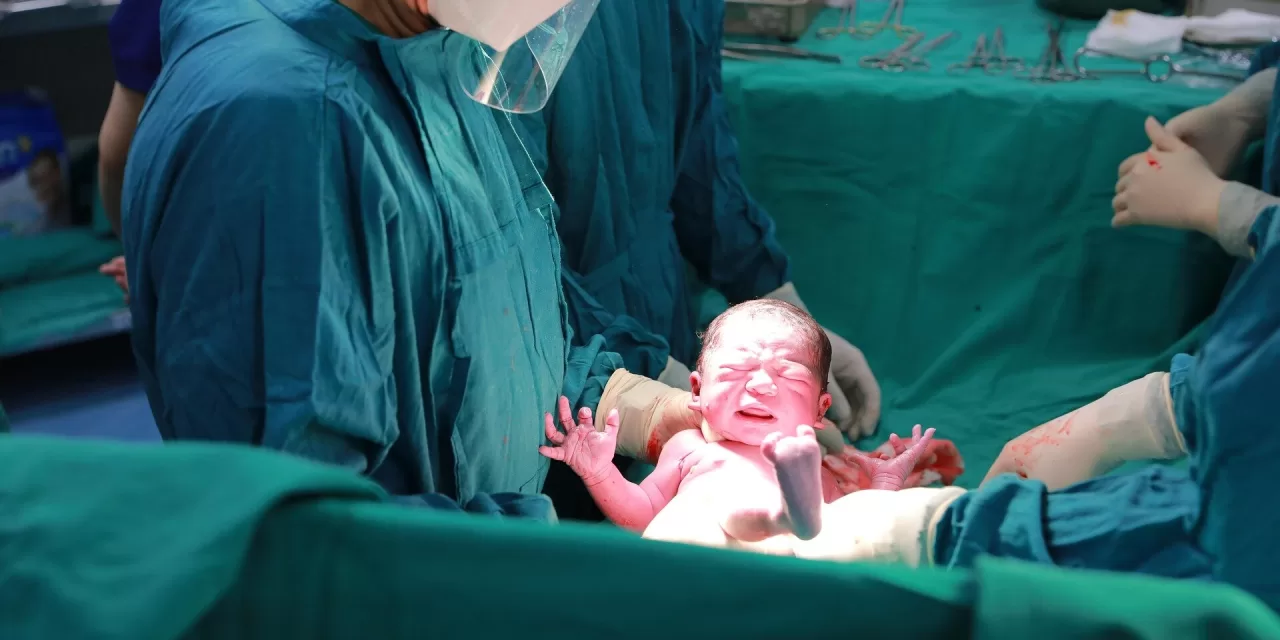
BELAGAVI, KARNATAKA — In a revealing session at the Karnataka Legislative Council this week, Health Minister Dinesh Gundu Rao addressed a growing public health crisis that has sparked debate across the medical community: the skyrocketing rate of Cesarean section (C-section) deliveries in the state.
While acknowledging the alarming statistics—where nearly half of all births in the state are now surgical—Minister Rao drew a sharp line regarding government intervention. The state, he clarified, cannot infringe upon a mother’s “personal choice” to opt for a C-section but will crack down heavily on private hospitals performing the procedure “intentionally” for financial gain.
The statement comes at a critical juncture for maternal health in India. According to data presented in the council, the C-section rate in Karnataka has surged to an average of 46%, a figure that towers over the World Health Organization’s (WHO) recommended ideal rate of 10-15%.
The Public-Private Divide
The data paints a stark picture of disparity between public and private healthcare sectors. While government hospitals in Karnataka report a C-section rate of 36%, private facilities have seen rates climb to an average of 61%. In some districts, reports suggest private sector rates have exceeded 90%.
“The department can’t intervene unless it’s found that Cesarean deliveries are being done intentionally,” Minister Rao told the council, responding to concerns about doctors allegedly misguiding patients.5 “We need to create medical and social awareness among pregnant women and their families.”
Health officials and policy experts argue that this disparity suggests non-medical factors are driving surgical deliveries in the private sector.
The Economics of Birth
“Private hospitals are increasingly performing Cesarean deliveries because they generate more income… and can be performed easily,” Rao admitted candidly during the session.
For hospitals, the incentives are clear. A C-section can be scheduled, allowing doctors to manage their time more efficiently compared to the unpredictable duration of a vaginal birth, which can last 12 to 24 hours. Furthermore, surgical deliveries often command higher fees and longer hospital stays, increasing revenue.
However, the “convenience” factor is not limited to providers. “Educated, middle-class women in urban areas are more likely to opt for Cesarean deliveries due to fear, social beliefs, and the inability to bear labor pain,” Rao noted.
This phenomenon, often termed “paternalistic demand,” complicates regulation. If a fully informed patient requests a C-section to avoid labor pain or to time the birth with an auspicious date (muhurta), ethical guidelines largely support their autonomy, provided they understand the risks.
Medical Risks: A “Major Surgery,” Not a Shortcut
Despite the normalization of the procedure, medical experts emphasize that a C-section is major abdominal surgery with significant risks compared to vaginal delivery.
Dr. Shaibya Saldanha, a consultant obstetrician-gynaecologist based in Bengaluru, explained in recent reports that while C-sections are life-saving in emergencies—such as fetal distress, cord prolapse, or placenta previa—they should not be the default.
“A C-section delivery is better than a difficult normal delivery, but a safe normal delivery is better than a C-section,” Dr. Saldanha noted.
Key Medical Risks of Unnecessary C-Sections:
-
-
For the Mother: Increased risk of infection, hemorrhage, blood clots, and a longer recovery time (6-8 weeks vs. days for vaginal birth). It also poses serious risks for future pregnancies, including uterine rupture and placenta accreta.13
-
For the Baby: Higher likelihood of respiratory distress syndrome (RDS) and a potential lack of exposure to beneficial gut bacteria found in the birth canal, which aids immune system development.
-
Government Response: Audits and Midwifery
To curb the trend without violating patient rights, the Karnataka government is launching a multi-pronged strategy.
-
Mandatory Audits: The Health Department is initiating audits of C-section deliveries at district and taluk hospitals. Hospitals with suspiciously high rates will be required to justify the medical necessity of their surgical interventions.
-
Midwifery-Led Care: In a move to promote natural birth, the government is training nurses under an 18-month midwifery project. By July 2025, specialized Midwifery-Led Care Units (MLCUs) will be operational in districts like Hassan, Mandya, and Mysuru. These units focus on respectful, physiological birth practices that reduce the need for intervention.
-
Awareness Campaigns: A new program launching next month will focus on “mentally preparing” pregnant women for natural delivery, addressing the fear of pain that drives many elective surgeries.
The Bigger Picture: A National Trend
Karnataka is not an outlier. The National Family Health Survey (NFHS-5) data indicates that C-section rates have risen across India, particularly in southern states like Telangana and Tamil Nadu.
The “epidemic” of C-sections in India reflects a complex interplay of defensive medicine—where doctors operate to avoid litigation in case of a bad outcome—commercialization of healthcare, and changing patient preferences.
Public health experts argue that while the Minister’s respect for “personal choice” is legally sound, the government has a duty to ensure that “choice” is not manufactured by fear or misinformation. If patients are told that their baby is “too big” or the cord is “around the neck” (often a normal occurrence) to induce panic and consent for surgery, the line between choice and coercion blurs.
Conclusion
As Karnataka moves to audit hospitals and promote midwifery, the success of these initiatives will depend on transparency. Reducing the C-section rate requires a cultural shift—both in the boardroom of private hospitals, where profit margins often dictate protocols, and in the minds of expectant parents, who may need reassurance that natural birth, while painful, is often the safest path for mother and child.
For now, the government’s message is a warning shot: The operating room should be a place of medical necessity, not convenience.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Primary Source: Statement by Karnataka Health Minister Dinesh Gundu Rao, Legislative Council Session, Belagavi (Dec 2024).20 Reported via Lokmat Times and The Times of India.