January 27, 2026
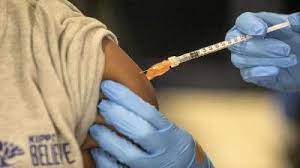
ITASCA, IL — In an unprecedented move that signals a widening rift between the medical community and federal health officials, the American Academy of Pediatrics (AAP) released its 2026 immunization schedule yesterday, pointedly rejecting recent changes made by the Centers for Disease Control and Prevention (CDC). For the first time in decades, the nation’s largest pediatric society has issued guidelines that deviate sharply from federal advice, recommending that children and adolescents remain universally vaccinated against 18 diseases—including COVID-19, RSV, and rotavirus—despite the CDC’s new stance of limiting these vaccines to high-risk groups.
The updated AAP schedule, published in the AAP Red Book Online, has garnered immediate and broad support from 12 major medical organizations, including the American Medical Association (AMA) and the American Pharmacists Association. The decision underscores a growing concern among clinicians that federal vaccine policy has become decoupled from established scientific data.
A Fracture in Consensus
Historically, the AAP and the CDC’s Advisory Committee on Immunization Practices (ACIP) have worked in lockstep to produce a “harmonized schedule,” providing a unified front for parents and physicians. That era of cooperation ended abruptly earlier this month when the ACIP pivoted, recommending vaccines for COVID-19, RSV, rotavirus, and several others only for children deemed “high-risk.”
The AAP, representing 67,000 pediatricians, is now standing its ground. Its 2026 schedule maintains that universal immunization is the only evidence-based path to protecting public health.
“For generations, the federal government’s vaccine schedule was a trusted national source of science and data-driven advice,” said Bobby Mukkamala, MD, president of the AMA. “But now we’ve seen these long-standing recommendations change without a robust, evidence-based process and no new scientific data to support it.”
The 18-Vaccine Standard
The AAP’s recommendations include universal vaccination for:
-
COVID-19: Beginning at 6 months of age.
-
Respiratory Syncytial Virus (RSV): Specifically the use of clesrovimab (Enflonsia) for all infants under 8 months during their first RSV season.
-
Rotavirus, Hepatitis A & B.
-
Meningococcal Serogroups (A, C, W, Y, and B).
Sean O’Leary, MD, MPH, chair of the AAP Committee on Infectious Diseases, was blunt about the motivation behind the separate schedule. “We recognize what is happening in ACIP and more broadly across HHS [Department of Health and Human Services] is not in the interest of the American public,” O’Leary stated.
Legal Action Against Federal Agencies
The disagreement has moved beyond the clinic and into the courtroom. The AAP, joined by the American College of Physicians, the American Public Health Association, and the Infectious Diseases Society of America, has filed a federal lawsuit to disband the current ACIP and invalidate its recent pivots.
The lawsuit alleges that the federal panel has transitioned from a scientific body into a “megaphone for spreading misinformation.” This legal escalation highlights a fundamental dispute over who defines the “standard of care” in American medicine.
What This Means for Parents and Patients
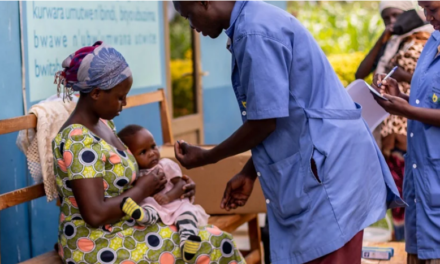
For parents sitting in exam rooms, the immediate question is: Will these vaccines still be covered?
According to Dr. O’Leary, the answer is likely yes. Under the Affordable Care Act (ACA), most private insurance plans are required to cover vaccines recommended by the AAP without a copay. However, the conflicting headlines have created a fog of confusion.
“Medical consensus has not shifted even if federal policy has,” said Peter Chin-Hong, MD, an infectious disease specialist at the University of California San Francisco (UCSF) who was not involved in drafting the new guidelines. “The science hasn’t changed, and what the AAP is doing with this statement is making that emphatic.”
Dr. Chin-Hong warns that the real danger of the CDC’s shift isn’t just a policy change, but a “tax” on clinical time. “What is going to change is the confusion and the time it takes for clinicians to explain the changes to parents, which will probably lead to less uptake of vaccines regardless of whether insurance covers them,” he said.
Advice for the Exam Room
Despite the controversy, the AAP is advising pediatricians to maintain their approach to vaccine conversations. Data continues to show that the vast majority of parents—upwards of 80% to 90% depending on the region—continue to follow the recommended schedule for their children.
Dr. O’Leary suggests that clinicians should not assume parents are skeptical. “You know they are the standard of care, so recommend them as you have,” O’Leary advised. “If parents have questions, understand that they aren’t trying to argue with you; they are concerned about the well-being of their kids.”
Limitations and Counterarguments
Critics of the AAP’s universal approach often point to “vaccine fatigue” and the burden of the growing schedule on families. Some argue that a more targeted approach, as suggested by the CDC, could focus resources on the most vulnerable. However, public health experts argue that “risk-based” vaccination strategies have historically failed because many people who experience severe disease do not fall into a recognized high-risk category.
As the legal and scientific battles continue, the AAP has launched a parent-friendly version of its 18-vaccine schedule on HealthyChildren.org to help families navigate the conflicting information.
References
- https://www.medscape.com/viewarticle/aap-recs-buck-cdc-stick-18-childhood-vaccines-2026a10002f1
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.