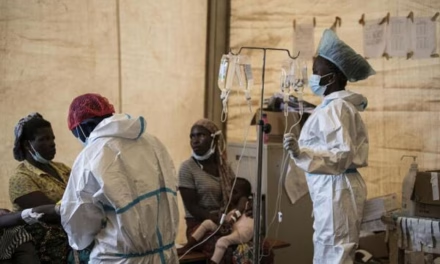
From 2021 through July 2025, clinical trials conducted across India have resulted in 1,705 participant deaths and over 7,000 serious adverse events (SAEs), averaging one death and four life-threatening complications daily. This alarming data was disclosed by the Central Drugs Standard Control Organisation (CDSCO) in response to a Right to Information (RTI) request, exposing the human cost behind the nation’s clinical research efforts.
Key Findings and Developments
The CDSCO’s RTI response reveals that between 2021 and mid-2025, a total of 1,705 participants died due to SAEs occurring during clinical trials nationwide. Alongside these fatalities, 7,189 cases of non-fatal but serious adverse events—such as severe reactions or complications—were reported, equating to roughly 4.2 individuals daily suffering life-threatening side effects. From January to July 2025 alone, 232 participants succumbed during trials. These figures encompass both patients enrolled for treatment and healthy volunteers participating in research studies.
Despite the high toll, financial compensation for victims remains scarce. Only 68 trial participants received compensation as legally mandated, highlighting the difficulty in establishing direct causation between trial participation and death or injury needed to claim recompense.
Expert Perspective and Context
Dr. Anjali Mehta, a clinical pharmacologist unaffiliated with the CDSCO or trial sponsors, comments, “While clinical trials are essential for advancing medicine, these numbers highlight the immense risks participants face. Transparency and rigorous safety monitoring must improve to protect individuals who volunteer for research.”
India is among the world’s largest hubs for clinical trials due to its diverse population and cost-effective operations. The regulatory framework, primarily overseen by the CDSCO, mandates ethical conduct, participant safety, and compensation protocols. Nonetheless, the new data indicate gaps between regulations and real-world practices, especially regarding timely compensation and detailed public reporting of adverse events.
Background on Clinical Trial Safety and Regulations
Clinical trials are critical steps in developing new drugs, vaccines, and therapies. They undergo multiple phases designed to assess safety, efficacy, dosing, and side effects. Serious Adverse Events are untoward medical occurrences that can cause death, disability, hospitalization, or other severe outcomes related to the investigational product or study procedures.
In India, the Drugs and Cosmetics Rules, along with guidelines from the Indian Council of Medical Research (ICMR), govern clinical trial conduct. Sponsors and investigators must report SAEs promptly to CDSCO and ethics committees. Compensation clauses are legally enforced for trial-related injuries or deaths. However, proving causality and securing compensation remain contentious and often delayed.
Implications for Public Health and Patients
The data underscore the necessity for enhanced vigilance in clinical research to safeguard participant welfare. Patients and volunteers should be fully informed about risks and benefits, and trial oversight agencies must enforce accountability measures visibly. Public trust in clinical trials hinges on transparent disclosure of adverse event data and fair treatment of affected participants.
Moreover, these findings should motivate policymakers to review compensation rules, expedite claim processing, and strengthen enforcement against protocol deviations or lapses in participant care. Robust ethical oversight protects participants and preserves the scientific integrity essential for medical progress.
Limitations and Counterarguments
Although the reported deaths and SAEs are concerning in absolute terms, it is important to contextualize them within the large scale of global clinical research. Trials frequently involve high-risk patients or novel therapies targeting severe diseases, which may inherently carry elevated risks unrelated solely to the investigational drug. The CDSCO has also withheld some detailed SAE data citing confidentiality laws.
Some experts argue that current safety management and regulatory frameworks, while imperfect, largely function to minimize risks and ensure trials proceed ethically. They emphasize that ongoing improvements in trial design, monitoring technology, and informed consent processes continue to enhance participant safety standards worldwide.
Practical Advice for the Public
Individuals considering joining clinical trials should:
-
Discuss potential risks and benefits thoroughly with healthcare providers and trial investigators.
-
Verify that the trial is approved and monitored by regulatory authorities and ethics committees.
-
Understand their rights regarding monitoring, reporting adverse effects, and claiming compensation.
-
Seek independent medical advice if unclear about trial procedures or safety concerns.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Medical Dialogues. “One Death a Day: 1,705 Lives Lost in India’s Clinical Trials Since 2021,” August 2025. https://medicaldialogues.in/news/industry/pharma/cdsco/one-death-a-day-1705-lives-lost-in-indias-clinical-trials-since-2021-rti-reveals-154346