AUCKLAND – Health authorities in New Zealand are moving swiftly to contain a potential resurgence of measles after two new cases were confirmed in a single household in Auckland. The announcement, made Tuesday by Health New Zealand (Te Whatu Ora), comes just three weeks after the nation celebrated the end of its previous outbreak, highlighting the persistent threat posed by global travel and gaps in local immunity.
The cases have been linked to overseas travel, with officials identifying several high-risk “locations of interest,” including a long-haul international flight and a busy metropolitan emergency department. Public health teams are currently engaged in an intensive contact-tracing operation to identify individuals who may have been exposed.
Tracking the Exposure: Flight SQ281 and Beyond
The two individuals arrived in Auckland on February 17 aboard Singapore Airlines flight SQ281. Following their arrival, the virus may have been transmitted at Auckland International Airport and subsequently within the waiting room of the Waitakere Hospital emergency department.
“Because measles is one of the most contagious viruses on the planet, we treat every single case as a significant public health event,” says Dr. Arlo Kendrick, an infectious disease specialist not involved in the current investigation. “The fact that this occurred in a hospital waiting room is particularly concerning, as that environment often contains vulnerable individuals with underlying health conditions.”
Health officials are specifically reaching out to passengers seated in the immediate vicinity of the cases on the Singapore Airlines flight. However, they urge anyone who was at the airport or Waitakere Hospital during the specified windows to remain vigilant for symptoms.
The “1-to-18” Factor: Why Measles is Different
Measles is not a typical respiratory virus. While a person with the flu might infect one or two others, a single person with measles can infect up to 18 secondary cases in an unvaccinated population.
The virus is transmitted through respiratory droplets or by breathing air that an infected person has occupied. Crucially, the virus can remain suspended in the air and active on surfaces for up to two hours after the infected person has left the room.
Recognizing the Symptoms
Symptoms typically appear 10 to 14 days after exposure. According to Health New Zealand, the progression usually follows this timeline:
-
Early Phase (Days 1–7): High fever, cough, runny nose, and red, watery eyes (conjunctivitis). Small white spots, known as Koplik spots, may appear inside the cheeks.
-
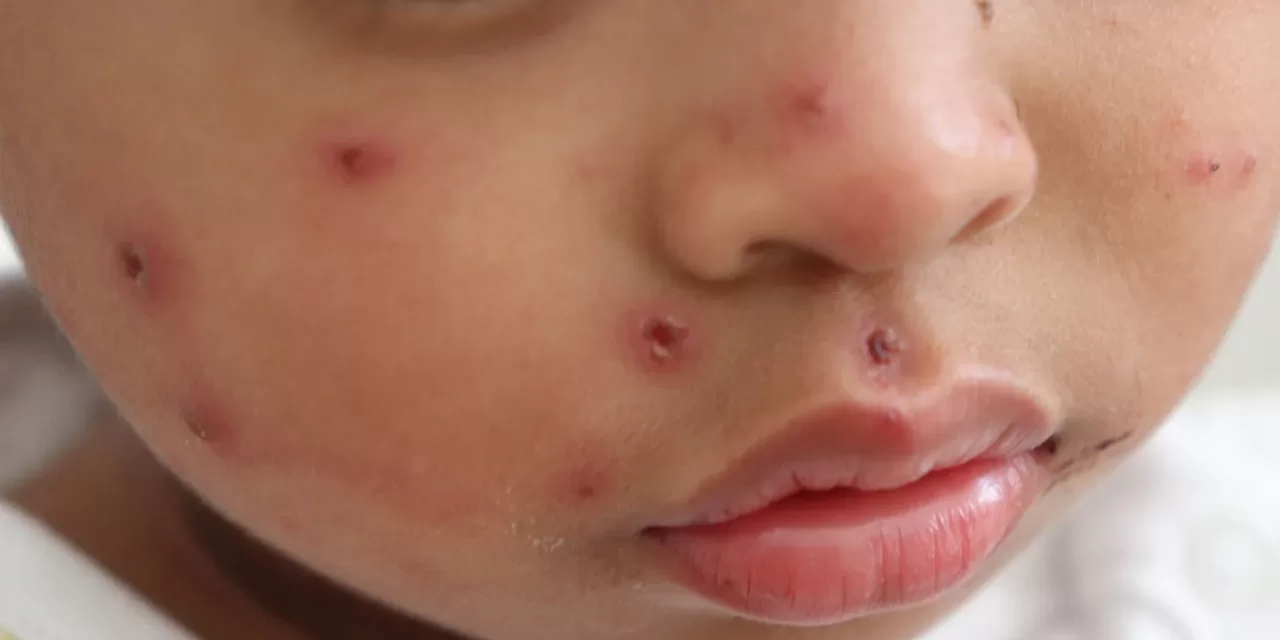
Rash Phase (Days 7–18 post-exposure): A blotchy, reddish-brown rash typically begins on the face and upper neck, spreading downward to the hands and feet over three days.
A Fragile Milestone Overturned
New Zealand’s previous measles outbreak, which began in September 2025, was only declared officially over earlier this month. The rapid re-emergence of the virus underscores a “new normal” for a world with increasing mobility and fluctuating vaccination rates.
“We are in a constant state of ‘importation risk,'” says Sarah Thompson, a public health researcher. “New Zealand remains at risk because our ‘herd immunity’—the percentage of the population that is vaccinated—has dipped below the 95% threshold required to prevent community spread.”
In 2023, global measles deaths rose to an estimated 107,500, the majority of whom were children under five. This occurred despite the existence of the MMR (Measles, Mumps, and Rubella) vaccine, which has been proven safe and highly effective since its introduction in the 1960s. Before widespread vaccination, measles caused an estimated 2.6 million deaths annually.
Expert Commentary: The “Immunity Gap”
While the two cases are currently contained within one household, experts warn against complacency.
“The tragedy of measles is that it is entirely preventable,” notes Dr. Kendrick. “When we see cases popping up like this, it’s a signal that there are ‘pockets’ of the population—often young adults or children whose routine immunizations were delayed—who are essentially sitting ducks for a virus looking for a host.”
Public health officials are urging New Zealanders to check their immunization records. In New Zealand, the MMR vaccine is free for anyone born after January 1, 1969, who has not already had two doses.
What Should You Do?
Health New Zealand has issued a clear protocol for anyone who suspects they have been exposed or are showing symptoms:
-
Isolate Immediately: Do not go to work, school, or public places.
-
Call Ahead: Do not walk into a doctor’s office or emergency room unannounced. Call your healthcare provider or a health information line first. This allows the clinic to take precautions to prevent you from infecting others in the waiting room.
-
Verify Status: Check your digital health records or contact your GP to ensure you have received both doses of the MMR vaccine.
Potential Limitations in Containment
While contact tracing is effective, it is not foolproof. Asymptomatic transmission does not occur with measles, but people are infectious for about four days before the rash appears. This “silent window” is when most transmission occurs during travel, making the flight SQ281 exposure particularly critical.
Public Health Outlook
The global landscape for measles is shifting. With international travel back to pre-pandemic levels and “vaccine fatigue” affecting some regions, the World Health Organization (WHO) has warned of an increase in large-scale outbreaks. For New Zealand, these two cases serve as a stark reminder that “elimination” of a disease is a status that must be defended every single day.
For now, the focus remains on the Auckland household and the hundreds of travelers who may have crossed paths with them. The next 14 days will be a critical window to see if these two cases remain isolated or if they represent the spark of a new outbreak.
Reference Section
-
Health New Zealand (Te Whatu Ora): Official Statement on Auckland Measles Cases (Feb 24, 2026).
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.