A recent analysis by researchers at the University of Cambridge sheds light on a persistent problem in clinical blood pressure readings: common cuff-based methods may be giving inaccurately low systolic results, potentially missing cases of hypertension.
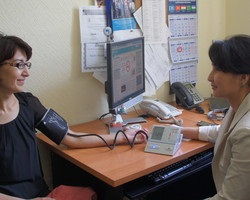
For decades, clinicians have relied on the auscultatory method, which involves placing an inflatable cuff around the upper arm, inflating it to halt blood flow, and then slowly releasing pressure while listening for characteristic tapping sounds. These taps indicate the return of blood flow and are used to determine both systolic (first taps) and diastolic (last taps) pressure.
However, the new research explains that the artery beneath the cuff remains closed for longer than previously thought as the pressure is released. This means the first taps actually appear later, causing the reading to underestimate true systolic pressure. The same process results in diastolic pressure often being overestimated.
According to the study’s co-author, Kate Bassil, “the auscultatory method is the gold standard, but it overestimates diastolic pressure, while systolic pressure is underestimated.” The research team, led by Professor Anurag Agarwal, built a physical model to reproduce what occurs underneath the cuff. Crucially, they discovered that using flat tubes (which collapse more like real human arteries) instead of round rubber tubes revealed the underlying mechanical error that leads to delayed reopening of the vessel and a lower systolic reading.
This systematic underestimation can have significant real-world implications. “We are currently not adjusting for this error…which has been estimated to lead to as many as 30 percent of cases of systolic hypertension being missed,” noted Bassil.
The researchers offer low-cost solutions such as raising the arm before measurement to create more predictable downstream pressures. Such adjustments could allow clinicians to compensate for the systematic bias without needing new devices. If new monitors are developed, they could consider patient-specific characteristics—like age or body mass index—to further improve accuracy.
Hypertension remains the leading modifiable risk for premature death worldwide. Accurate readings are vital for effective diagnosis and treatment, preventing both undertreatment of high blood pressure and overtreatment that can lead to unnecessary medication and side effects.
The Cambridge team is preparing for clinical trials to test these corrections in diverse populations and real-world settings. Partnerships with clinicians and industry, as well as updated training and protocols, will be essential for implementing these improvements.
Disclaimer
This article is for informational purposes only and is not a substitute for professional medical advice. Always consult with qualified health professionals for diagnosis and treatment of health conditions.
Reference: “Why your blood pressure reading might be wrong” — Earth.com