A new wave of research has revealed that administering antibiotics to infants—especially during pregnancy and the first weeks of life—may have significant long-term impacts on their immune system, leaving them more vulnerable to infections and potentially weakening their response to vaccines.
Reduced Immune Memory and Lung Protection
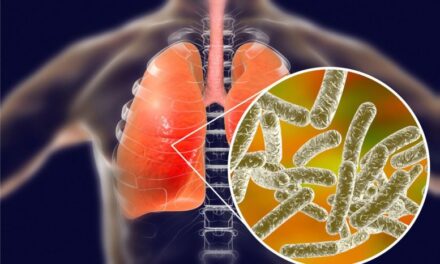
Researchers from the University of Rochester Medical Center and collaborators worldwide have found that antibiotic exposure in early life impairs the normal development of an infant’s immune system. Mouse and human studies demonstrated that infants exposed to commonly used antibiotics, such as ampicillin, gentamicin, and vancomycin, had significantly reduced levels of protective CD8+ T cells in their lungs. These specialized cells—known as tissue-resident memory T cells—are crucial for providing rapid, long-lasting defense against respiratory infections. The research showed that these deficits could persist into adulthood, potentially leaving individuals at increased risk for illnesses later in life.
Gut Microbiome Disruption: The Hidden Cause
These immune changes are closely linked to disruptions in the infant’s gut microbiome. Antibiotics, while often life-saving, do not discriminate between harmful and beneficial bacteria, leading to a loss of important bacterial populations, such as Bifidobacterium. This imbalance impairs the gut’s ability to produce inosine—a molecule essential for ‘teaching’ developing immune cells how to respond to future infections. Without this molecular guidance, an infant’s immune system may not mature properly, akin to missing chapters in a textbook needed for vital lessons on fighting disease.
Weakened Vaccine Response
Another critical consequence of early antibiotic use is a dampened response to vaccines. Multiple studies have now shown that infants who received antibiotics shortly after birth had significantly lower levels of antibodies following vaccination. For instance, research conducted in Australia found that babies given antibiotics during the first weeks of life had reduced immunity to several vaccines at seven and fifteen months of age. The more antibiotic courses a child received, the weaker their immunity, with antibody levels sometimes dropping below protective thresholds for key vaccines such as DTaP (diphtheria, tetanus, pertussis), Hib, and others.
Potential Solutions and Ongoing Research
On a hopeful note, some experiments suggest that supplementing key bacterial metabolites, like inosine, may help reverse some immune deficits caused by antibiotics. These findings open the door to possible interventions for infants who require antibiotic therapy, strengthening their immune “education” despite necessary disruptions to their microbiome.
Disclaimer:
This article summarizes scientific studies on the effects of antibiotics on infant immune development. The findings are intended for informational purposes only and should not be interpreted as medical advice. Always consult a qualified healthcare provider before making decisions about your or your child’s medical care. Research in this area is ongoing, and recommendations may evolve as new evidence emerges.