A new study published in Scientific Reports by researchers from Trinity College Dublin suggests that targeted use of the corticosteroid dexamethasone may enhance the body’s immune response against tuberculosis (TB), offering a potential complementary strategy alongside traditional antimicrobial therapy.
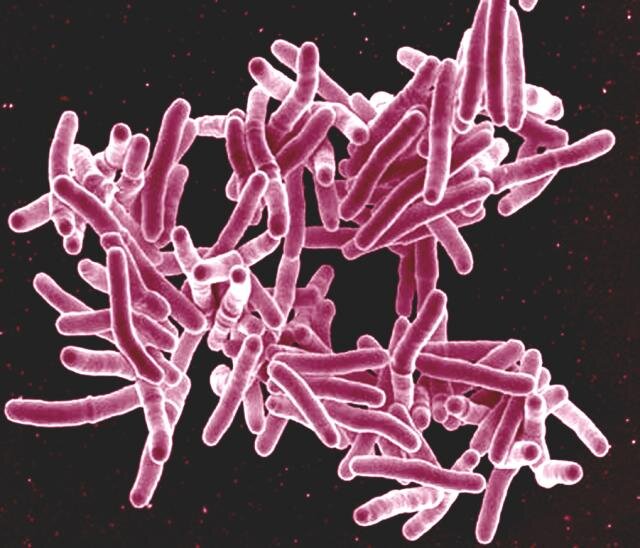
The research, conducted at St. James’s Hospital in Dublin, explored how dexamethasone influences macrophages—the immune cells responsible for engulfing and destroying Mycobacterium tuberculosis, the bacterium that causes TB. Results indicate that precisely targeted steroid treatments can bolster macrophage function while simultaneously reducing harmful inflammation, long a challenge in TB management.
Why Tuberculosis Still Matters
Tuberculosis remains one of the deadliest infectious diseases globally, affecting over 10 million people and killing approximately 1.25 million annually according to the World Health Organization. Despite decades of antibiotic therapy, TB control continues to face hurdles due to drug resistance, lengthy treatment regimens, and inflammatory lung damage caused by overactive immune responses.
Clinicians have traditionally used corticosteroids like dexamethasone in limited TB cases—such as TB meningitis—to reduce inflammation. However, concerns about potential reactivation of latent infection have limited their broader use. The new findings may shift this perspective.
Inside the Study: Modulating the Immune Response
The Dublin research team isolated macrophages from healthy volunteers and lung fluid samples of patients undergoing bronchoscopy to study the interactions between dexamethasone and M. tuberculosis. When these macrophages were treated with the steroid, researchers observed several key effects:
-
Reduced glycolysis: Dexamethasone decreased the metabolic rate in macrophages, cutting the energy available for excessive inflammation while maintaining bacterial control.
-
Decreased cytokine production: It dampened both pro- and anti-inflammatory cytokines, achieving a balance between immune defense and tissue protection.
-
Improved bacterial clearance: Treated macrophages showed a lower bacterial load, likely due to enhanced autophagy and phagosomal acidification—mechanisms through which immune cells digest pathogens.
The study also found that macrophages treated with dexamethasone survived longer after infection, suggesting protection from immune-mediated cell death, a finding consistent with earlier mechanistic research on corticosteroids’ anti-necrotic effects in M. tuberculosis-infected cells.
Expert Perspective: A Step Toward Host-Directed Therapies
Professor Joseph Keane, senior author and Professor of Medicine at Trinity College Dublin, called the findings “reassuring,” noting that they redefine the role of steroids in TB therapy.
“In clinical practice, steroids are the most underused adjunctive therapy for TB,” Keane explained. “What’s encouraging is that dexamethasone not only tempers inflammation but also supports macrophages in controlling infection. This study provides new evidence to help us target inflammation without compromising microbial defense”.
Independent experts welcomed the development but urged cautious optimism. Dr. Rajiv Khanna, a pulmonologist at the All India Institute of Medical Sciences (AIIMS), who was not involved in the study, commented that the research “moves the needle toward host-directed therapies, a promising frontier that targets the body’s immune response rather than the pathogen itself.”
However, he added, “Clinical trials in diverse populations are needed to confirm whether these laboratory effects translate into real-world patient outcomes.”
Clinical Implications and Limitations
If confirmed in human trials, targeted steroid therapy could become a universal adjunct in TB care—helping patients recover faster and potentially reducing lung damage that contributes to long-term breathing difficulties.
Earlier meta-analyses of corticosteroid adjunct therapy found mortality benefits across various TB forms, including extrapulmonary and HIV-associated cases. However, those benefits came with cautionary notes. High-dose or prolonged corticosteroid use has been linked to adverse effects such as hyperglycemia, hypertension, and increased infection risk.
Dr. Khanna emphasized, “The therapeutic balance is extremely delicate. Overuse of steroids can suppress immune defenses, potentially worsening outcomes in patients with untreated or drug-resistant strains.”
The authors of the Dublin study echoed this caution, framing their work as groundwork for precision immunomodulation—honing doses and delivery routes that stimulate beneficial pathways without increasing risk.
The Broader Context: Toward Integrated TB Treatment Strategies
This study reinforces growing scientific interest in “host-directed therapies” (HDTs), which complement antibiotics by modifying the body’s immune environment. By enhancing macrophage resilience and mitigating tissue-destructive inflammation, HDTs like dexamethasone could shorten recovery time and curb transmission, particularly in countries such as India, home to the world’s highest TB burden.
According to India’s National TB Elimination Programme, approximately 2.8 million new TB cases were reported in 2024. Integration of adjunct therapies into standard TB regimens—currently spanning six to nine months—could also help counteract antibiotic resistance, a mounting global health crisis.
The Road Ahead
The Trinity College research team plans further investigation into molecular pathways linking steroid use with cellular immunity and bacterial control. Randomized controlled clinical trials are needed to determine optimal dosage, timing, and patient selection for adjunct steroid therapy in TB.
Meanwhile, WHO guidelines continue to emphasize adherence to antimicrobial therapy as the treatment cornerstone. Caution is advised in unsupervised or unregulated steroid use, particularly given their broad immunosuppressive effects.
What It Means for Patients
For patients, the new findings underscore a broader message: anti-TB therapy is evolving toward more personalized, immune-aware care. If future studies confirm these benefits, targeted, low-dose corticosteroids could become a safer, widely applicable tool against TB.
Until then, experts recommend following prescribed anti-TB medication schedules and consulting healthcare providers before making any treatment changes.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://www.tcd.ie/news_events/articles/2025/could-targeted-steroid-use-offer-a-universal-complimentary-treatment-to-fight-tb/
- https://english.mathrubhumi.com/lifestyle/health/new-study-gives-fresh-hopes-in-tb-treatment-heres-how-steroids-can-improve-immune-response-xidjsr9j