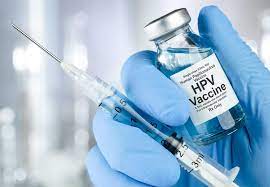
Human papillomavirus (HPV) vaccination provides strong, sustained protection against cervical pre-cancer and cancer over more than a decade after immunization, especially in girls vaccinated at ages 12 to 13, according to new research. This long-term effectiveness reinforces the critical role of HPV vaccines in preventing cervical disease and highlights the importance of continued vaccination programs and cervical screening.
Key Findings on HPV Vaccine Effectiveness
A recent study led by Public Health Scotland in collaboration with the Universities of Edinburgh and Strathclyde, published in the International Journal of Cancer, reports that the HPV vaccine remains highly effective more than 12 years after administration. Using population health data, the researchers found continued protection in women who underwent cervical screening. The vaccine was most protective when given at ages 12 to 13 but showed benefits up to age 18. Importantly, women from socioeconomically deprived areas gained substantial benefits, suggesting the vaccine’s role in reducing health disparities.
Another multinational study published recently in The Lancet tracked over 25,000 vaccinated individuals for more than 15 years. It found:
-
Over 90% effectiveness in preventing infection from high-risk HPV strains
-
A 75–85% reduction in cervical cancer precancerous lesions among vaccinated women
-
No need for booster doses as protection remained strong after a decade.
Scientific assessments confirm no evidence of viral type replacement or waning immunity within 10 years post-vaccination, underscoring the long-term public health benefits.
Expert Perspectives
Dr. Helen Harper, a leading immunologist not involved in the study, remarks, “These findings confirm what we have hoped for: robust, long-lasting immunity from HPV vaccines that will translate into fewer cervical cancer cases worldwide. This is a major public health success.” She stresses the significance of vaccinating before exposure to HPV, typically through sexual activity, thus supporting school-based immunization programs.
Prof. Andrew McDonald, epidemiologist at the University of Edinburgh, adds, “Continued high uptake, especially among adolescents, will be key to realizing the full population-level benefits including herd immunity.” He notes that even unvaccinated individuals benefit indirectly when coverage is high, an effect seen in long-term studies.
Background and Context
HPV is the most common sexually transmitted infection globally and a known cause of cervical cancer, the fourth most common cancer in women worldwide. Vaccines targeting the most oncogenic HPV types (notably 16 and 18) have been instrumental in reducing HPV infections and related cancers. Since their introduction over two decades ago, these vaccines have revolutionized cervical cancer prevention.
The current vaccines are recommended by major health authorities, including the World Health Organization (WHO) and the U.S. Centers for Disease Control and Prevention (CDC), mainly for girls and boys starting from early adolescence to maximize protection before HPV exposure.
Public Health Implications
Sustained effectiveness means fewer women will develop cervical pre-cancer and cancer, reducing the need for invasive treatments and improving health outcomes. The protective effect in deprived populations also means the vaccine could help close health inequality gaps. Additionally, as vaccinated cohorts age, cervical cancer incidence is expected to decline substantially, lessening the healthcare burden worldwide.
Despite this, screening programs remain essential. Vaccines cover the most common high-risk HPV types but do not protect against all oncogenic strains. Continued cervical screening complements vaccination, ensuring early detection and treatment of any cervical abnormalities.
Limitations and Considerations
Some limitations exist. Long-term studies rely on population screening data, which can vary by country and healthcare access. Immunization rates differ globally, and vaccine hesitancy remains a barrier in some regions. Moreover, data on effectiveness in males, though promising, require more long-term evidence. Ongoing surveillance is necessary to monitor vaccine impact, HPV type prevalence, and potential rare adverse effects.
Practical Takeaways
-
HPV vaccination is highly effective for at least 12 to 15 years post-immunization, especially when given early in adolescence.
-
Maintaining high vaccination coverage in schools is critical to maximizing public health benefits and achieving herd immunity.
-
Women and girls should continue cervical screening even if vaccinated.
-
Public health efforts should focus on reducing vaccine hesitancy to protect more individuals against HPV-related cancers.
This evidence confirms HPV vaccination as a cornerstone of cervical cancer prevention, offering long-lasting protection that can dramatically reduce the global burden of HPV-related diseases.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References:
- https://www.strath.ac.uk/whystrathclyde/news/2025/newstudyshowslong-termeffectivenessofhpvvaccine/
- https://www.ed.ac.uk/news/study-shows-long-term-effectiveness-of-hpv-vaccine