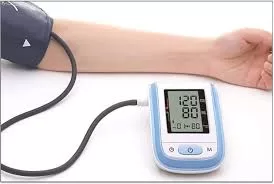
High blood pressure, or hypertension, affects over 1.3 billion people worldwide and causes around ten million deaths each year. A groundbreaking online tool, unveiled in a recent study published in The Lancet, aims to change how this silent killer is managed by enabling doctors to precisely predict the blood pressure-lowering effects of different medications for their patients. This innovation comes at a crucial time, especially in India, where an estimated 315 million people had high blood pressure in 2021, according to a study by the Indian Council of Medical Research and the Madras Diabetes Research Foundation.
The tool, known as the Blood Pressure Treatment Efficacy Calculator, synthesizes data from nearly 500 randomized clinical trials involving more than 100,000 people. It allows healthcare providers to select medication regimens tailored to the specific blood pressure reduction a patient needs to reach their target levels. Unlike traditional methods that rely heavily on fluctuating blood pressure measurements, this tool uses rigorous evidence to guide treatment decisions with greater accuracy.
Key Findings and Expert Insights
Dr. Nelson Wang, a cardiologist and Research Fellow at The George Institute for Global Health, emphasized the significance of the tool’s precision: “Every 1 mmHg reduction in systolic blood pressure lowers your risk of heart attack or stroke by two percent.” However, with dozens of antihypertensive drugs available, each with multiple dosing options and many patients requiring combination therapies, the complexity can be overwhelming. This calculator brings clarity by quantifying the average treatment effects observed across hundreds of studies.
Dr. Mohammad Abdul Salam, Programme Head of Cardiovascular Research at The George Institute in Hyderabad, highlighted the challenge facing healthcare providers: “Achieving optimal control requires a clear understanding of the efficacy of antihypertensive drugs at different doses and in various combinations. Without clarity on what we want to achieve and how to achieve it, we will not meet our targets.” He underscored that while treatment guidelines set the blood pressure goals, the calculator informs which drugs and doses best achieve these goals.
Traditionally, blood pressure treatments start with a single medication that typically lowers systolic pressure by 8-9 mmHg, yet most patients require reductions between 15-30 mmHg to hit ideal targets. Dr. Wang explained that relying solely on repeated blood pressure measurements can be misleading due to natural fluctuations caused by time of day, season, or measurement inconsistencies. “These random fluctuations can be as big or larger than the changes brought about by treatment,” he said, which complicates assessing a medication’s true effectiveness.
Anthony Rodgers, Senior Professorial Fellow at The George Institute, pointed out that no comprehensive resource existed before to quantify the effectiveness of blood pressure medicines, especially when used in combinations or varied doses. “Using the calculator challenges the traditional ‘start low, go slow’ approach to treatment, which can lead to delays or inadequate control,” he explained. “With this new method, you specify your blood pressure reduction goal, choose an evidence-based treatment plan, and initiate the patient on the best path sooner.”
Public Health Context and Implications
Hypertension is often called the “silent killer” because it frequently shows no symptoms until serious complications like heart attack, stroke, or kidney disease occur. Globally, fewer than one in five people with high blood pressure have it under control. In South-East Asia, including India, over 294 million people are affected, making efficient management a vital public health goal.
The adoption of this tool in clinical practice could improve the control rate of hypertension significantly. Professor Rodgers noted that moving the global control rate to just 50% could save millions of lives. The next phase involves clinical trials testing treatment plans tailored by the calculator, which could validate its real-world effectiveness and pave the way for widespread use.
Limitations and Balanced Perspectives
While promising, the tool’s effectiveness depends on further validation in diverse healthcare settings and populations. Blood pressure management also involves lifestyle changes and patient adherence, factors not directly addressed by a medication efficacy calculator. Some experts caution that without careful integration into clinical workflows, tools like this might not reach their full potential.
Furthermore, while the tool averages treatment effects from large trials, individual patient responses can vary, underscoring the need for continued monitoring and personalized clinical judgment. Blood pressure variability and measurement inaccuracies remain challenges in hypertension care.
Practical Takeaways for Readers
For individuals managing high blood pressure, this research highlights the importance of evidence-based care tailored to individual needs rather than a one-size-fits-all approach. Patients should engage actively with healthcare providers about their treatment goals and options, understanding that medication choice and dosage can be optimized based on scientific evidence.
This advance also reinforces the need for regular blood pressure monitoring and adherence to prescribed therapies. As this tool becomes clinically validated and available, it may contribute to more precise, efficient, and effective hypertension control, potentially lowering risks of cardiovascular complications for millions.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References:
-
https://www.newindianexpress.com/nation/2025/Aug/29/new-online-tool-to-manage-treat-high-blood-pressure-study