December 13, 2025
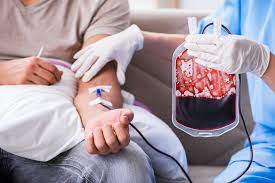
In a move widely celebrated by patient advocacy groups and public health experts, the National Blood Transfusion Bill, 2025 was introduced in the Indian Parliament yesterday, marking a potential watershed moment for India’s healthcare infrastructure.
The bill, introduced as a Private Member’s Bill by MP Parshottambhai Rupala in the Lok Sabha and Dr. Ajeet Madhavrao Gopchade in the Rajya Sabha on Friday, December 12, aims to overhaul the regulation of blood transfusion services in India. It seeks to establish a unified national framework to ensure the safety, quality, and availability of blood—a critical resource that remains a lifeline for millions.
A “Historic” Step for Patient Safety
The introduction of the bill has been met with immediate acclaim from the Thalassemia community, which relies heavily on frequent, lifelong blood transfusions. The Thalassaemia Patients Advocacy Group (TPAG) termed the move a “historic and long-awaited step” toward rectifying systemic gaps in blood safety.
“For India’s thalassemia community, which depends on safe, uninterrupted, and quality-assured blood transfusions for survival, this legislation marks a historic step forward,” a TPAG spokesperson stated. “It reflects a coherent and serious parliamentary commitment to reforming one of India’s most under-regulated yet critical public health areas.”
Key Provisions: What the Bill Proposes
Currently, blood in India is regulated as a “drug” under the Drugs and Cosmetics Act, 1940, a framework that critics argue is outdated and insufficient for the complex service-oriented nature of modern transfusion medicine. The new bill proposes to shift this paradigm by creating a dedicated National Blood Transfusion Authority (NBTA).
According to the draft, the NBTA would be vested with statutory powers to:
-
Standardize Operations: Prescribe uniform national standards for blood collection, testing, processing, and storage.
-
Enhance Haemovigilance: Strengthen the monitoring of adverse reactions to blood transfusions, a critical safety mechanism currently fragmented across states.
-
Enforce Accountability: Mandate the registration of all blood centers and impose strict penalties for non-compliance with safety protocols.
-
Promote Voluntary Donation: Institutionalize measures to phase out replacement donation in favor of 100% voluntary, non-remunerated donation.
The “Lifeline” Context: Why This Matters
The urgency of this legislation is underscored by India’s massive burden of hemoglobinopathies. India is often termed the “Thalassemia Capital of the World,” with an estimated 100,000 to 150,000 patients living with Thalassemia Major and approximately 10,000 to 15,000 new children born with the condition annually.
For these patients, blood is not merely a treatment; it is a bi-weekly necessity. However, the inconsistency in blood quality has led to tragic consequences. Suneha Paul, a 23-year-old beta-thalassemia patient from West Bengal, highlighted the human cost of regulatory gaps.
“I was diagnosed at two months old and have been receiving blood transfusions every two weeks,” Paul said. “Every day is a challenge to fight the stigma of HIV [contracted via transfusion] for no fault of ours. I strongly urge all Members of Parliament to pass this bill at the earliest.”
Paul’s story is not unique. Despite mandatory screening for Transfusion-Transmissible Infections (TTIs) like HIV, Hepatitis B, and Hepatitis C, the residual risk remains a concern due to varying testing standards (e.g., the lack of universal Nucleic Acid Testing or NAT) across the country’s fragmented network of blood banks.
Expert Perspectives
Medical experts have long argued that blood transfusion services require a specialized governance structure distinct from general pharmaceutical regulation.
Prof. N.K. Ganguly, former Director General of the Indian Council of Medical Research (ICMR), weighed in on the bill’s significance. “Strengthening the governance of blood transfusion services is essential for ensuring safety and public trust. I hope the proposed bill provides a much-needed, science-based framework to streamline standards and improve patient outcomes,” he said.
Anubha Taneja Mukherjee, Member Secretary of TPAG, emphasized that the governance structure must be inclusive. She urged the government to ensure “patient representation in any body constituted under this framework,” ensuring that the lived experiences of poly-transfused patients inform policy decisions.
Deepak Chopra, President of Thalassemics India, added, “This Bill represents a transformational shift. For decades, patients have struggled with inconsistent quality. A national framework will finally bring uniformity, accountability, and dignity to patient care.”
Challenges and Limitations
While the bill’s introduction is a positive signal, it faces the hurdles common to Private Member’s Bills, which historically have a lower success rate of becoming law compared to government-sponsored legislation. However, the dual introduction in both houses of Parliament suggests a coordinated effort to keep the issue on the legislative agenda.
Furthermore, implementation will be the true test. Establishing a central authority in a federal system where health is largely a state subject will require robust coordination between the Centre and State governments. Ensuring that smaller, rural blood centers can meet the high standards proposed by the NBTA without shutting down—potentially creating access deserts—will be a key logistical challenge.
Implications for Public Health
If passed, the National Blood Transfusion Bill 2025 could revolutionize patient safety in India. By standardizing quality assurance, the bill aims to:
-
Reduce TTI Transmission: Minimizing the risk of HIV and Hepatitis transmission through rigorous, uniform screening protocols.
-
Ensure Equity: Bridging the gap between high-tech urban blood centers and under-resourced rural facilities.
-
Boost Voluntary Donation: Moving India closer to the World Health Organization’s goal of self-sufficiency through voluntary blood donation.
For now, the eyes of the medical community and millions of patients are fixed on Parliament, hoping this “lifeline” legislation translates into law.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Primary Source: Ten News Network. (2025, December 12). “Thalassemia patient groups hail introduction of National Blood Transfusion Bill in Parliament.” Retrieved from TenNews.in