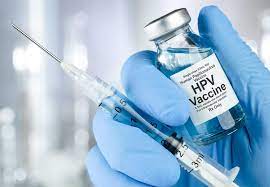
In a landmark victory for preventive medicine, new clinical data and real-world assessments have reaffirmed that the Human Papillomavirus (HPV) vaccine is not just a tool for future prevention, but a current powerhouse in reducing existing rates of precancerous lesions among girls and young women.
The findings, which bolster decades of research, confirm that widespread vaccination programs are successfully intercepting cervical cancer at its most treatable stage: before it even begins. For public health officials and families alike, the message is clear: the vaccine is fulfilling its promise as a primary shield against one of the most common cancers affecting women worldwide.
The Shield Against “Stage Zero”
Cervical cancer is almost uniquely preventable because it is preceded by identifiable “precancerous” changes in the cells of the cervix, often referred to as cervical intraepithelial neoplasia (CIN). These lesions are graded by severity (CIN1, CIN2, or CIN3), with the higher numbers indicating a greater risk of progressing to invasive cancer.
Recent epidemiological reviews indicate that in countries with high vaccine uptake, the incidence of these high-grade lesions has plummeted. For instance, data indicates that the vaccine can reduce the risk of developing these precancerous conditions by more than 50% in women vaccinated before their first exposure to the virus.
“What we are seeing is a generational shift,” says Dr. Elena Rossi, an oncologist specializing in gynecological cancers (who was not involved in the latest study). “We are moving from a reactive model of ‘find and treat’ to a proactive model of ‘prevent and eliminate.’ By stopping the virus from causing the initial cellular damage, we are effectively starving the pipeline that leads to cervical cancer.”
Understanding the HPV Link
HPV is a group of more than 200 related viruses, more than 40 of which are spread through direct sexual contact. While most HPV infections clear on their own thanks to the immune system, “high-risk” strains—specifically HPV 16 and 18—are responsible for approximately 70% of cervical cancer cases globally.
The vaccine works by introducing a protein that mimics the virus, prompting the body to produce antibodies. If the person is later exposed to the actual virus, their immune system recognizes it and prevents it from infecting the cells.
Statistical Success: A Look at the Numbers
The impact of the vaccine is most visible in populations that were early adopters of the immunization schedule. According to the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO):
-
Infection Reduction: Among teen girls, infections with HPV types that cause most HPV cancers and genital warts have dropped by 88%.
-
Precancerous Impact: Among young adult women, infections with these types have dropped by 81%.
-
Real-World Protection: In the United Kingdom, a long-term study published in The Lancet found that the cervical cancer program reduced cervical cancer rates by almost 90% in women who were offered the vaccine between the ages of 12 and 13.
Beyond the Individual: The “Herd” Effect
One of the most significant takeaways for public health is the concept of herd immunity. When a large percentage of the population—including boys—is vaccinated, the overall circulation of the virus decreases. This provides “indirect protection” to those who may not have been vaccinated or those who are immunocompromised.
Health authorities now recommend the vaccine for all children aged 11 or 12, though it can be started as early as age 9. The logic is simple: the vaccine is most effective when administered before any potential exposure to the virus occurs.
Addressing the Limitations and Barriers
Despite the overwhelming evidence of efficacy, challenges remain. In many regions, vaccine hesitancy and misinformation regarding reproductive health continue to stall uptake. Furthermore, some critics point out that the vaccine does not protect against all types of HPV, meaning that vaccinated individuals still require regular screenings.
“The vaccine is a miracle, but it isn’t a replacement for the Pap test or HPV screening,” notes Dr. Rossi. “Because there are rarer strains of the virus not covered by current vaccines, and because some women may have been exposed prior to vaccination, regular screenings remain the ‘safety net’ of women’s health.”
Additionally, global equity remains a hurdle. While high-income nations see falling cancer rates, cervical cancer remains a leading cause of death for women in low- and middle-income countries where access to both the vaccine and regular screening is limited.
The Path Forward: A World Without Cervical Cancer?
The World Health Organization has set an ambitious “90-70-90” target for 2030: 90% of girls fully vaccinated by age 15, 70% of women screened with a high-performance test, and 90% of women with cervical disease receiving treatment.
The latest evidence suggesting the vaccine’s high efficacy against precancerous lesions provides the scientific fuel needed to reach these goals. For the general public, it transforms the conversation from one of fear about a potential cancer diagnosis to one of empowerment through prevention.
As we look toward a future where cervical cancer could be virtually eliminated, the current data serves as a powerful reminder of the impact of preventative immunology. For parents and young adults, the decision to vaccinate is no longer just about a shot—it’s about securing a future free from the shadow of a preventable disease.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References and Sources
- https://nagalandtribune.in/hpv-vaccine-can-help-prevent-precancerous-lesions-in-girls-women/