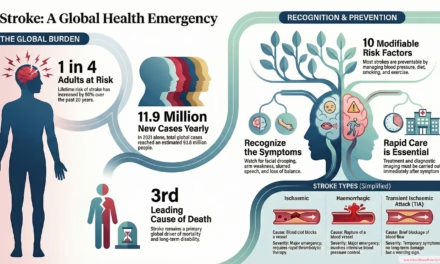
Introduction
This programme reflects India’s recognition of the demographic shift toward an ageing population and the unique health challenges it poses. By the end of this session, you should be able to:
- Understand the background and rationale for NPHCE.
- Outline its objectives and strategies.
- Explain the organizational structure and services provided at different levels of healthcare.
- Appreciate its integration with other health and social welfare programs.
- Critically analyze its challenges and future directions.
Background and Rationale
- The world is ageing rapidly. According to the UN World Population Prospects, by 2050, 1 in 6 people globally will be over 65 years.
- In India, the proportion of elderly (≥60 years) is growing steadily – from 8.6% in 2011 to nearly 10.5% in 2021, and is expected to reach 19% by 2050.
- The elderly face a triple burden:
- Chronic non-communicable diseases (NCDs) such as diabetes, hypertension, cardiovascular diseases, cancers, and COPD.
- Functional decline and disabilities – locomotor, vision, hearing loss, dementia.
- Social and psychological issues – loneliness, neglect, economic insecurity, elder abuse.
Recognizing these challenges, the Government of India launched the NPHCE in 2010–11 during the 11th Five-Year Plan, in 100 identified districts of 21 states , aiming for comprehensive, dedicated, and affordable separate healthcare services to the elderly.
Objectives of NPHCE
- To provide accessible, affordable, and high-quality healthcare services to the elderly at all levels of healthcare.
- To identify health problems early through screening and regular check-ups.
- To build capacity of health professionals in geriatric care.
- To establish dedicated infrastructure for geriatric health services.
- To promote community-based elderly care including home-based services.
- To integrate health with social support for holistic elderly care.
Strategies of Implementation
- Preventive and promotive services: Health education on lifestyle, nutrition, fall prevention, and mental health.
- Curative services: Dedicated geriatric OPD, indoor services, physiotherapy, palliative care.
- Capacity building: Training doctors, nurses, ANMs, ASHAs, and caregivers in geriatric care.
- IEC and awareness generation: Empowering families and communities to support elderly health.
- Research and monitoring: Evidence-based policy development and program evaluation.
Service Delivery under NPHCE
The programme ensures continuum of care through a hub-and-spoke model across primary, secondary, and tertiary levels.
1. Sub-centre and Village Level
- Home visits by ASHA/ANM.
- Health education on nutrition, hygiene, fall prevention.
- Identification of at-risk elderly and referral.
2. Primary Health Centre (PHC)
- Weekly geriatric clinic.
- Screening for common conditions: hypertension, diabetes, cataract, depression, mobility issues.
- Provision of essential drugs for chronic diseases.
- Counselling and family education.
3. Community Health Centre (CHC)/Sub-district Hospital/civil hospitals
- Bi-weekly geriatric clinic.
- 10-bedded geriatric ward.
- Physiotherapy unit.
- Laboratory and diagnostic support.
4. District Hospital
- Dedicated geriatric OPD daily.
- 10-bedded geriatric ward.
- Rehabilitation services.
- Linkage with palliative care and NGOs.
- Counselling and day-care services.
5. Regional Geriatric Centres (RGCs)
- Located in medical colleges. (20 institutes were upgraded.)
- Tertiary-level care with speciality departments – orthopaedics, neurology, cardiology, and psychiatry.
- 10-bedded geriatric ward.
- Advanced diagnostic and therapeutic services.
- Training hub for doctors and nurses.
- Conducting research on ageing and geriatric conditions.
6. National Centre of Ageing (2 in number)
- AIIMS New Delhi, and Madras Medical College Chennai
- Apex centre for training, research, and policy support
- Collaboration with NGOs, international agencies, and other ministries.
Integration with Other National Programmes
NPHCE does not work in isolation – it is integrated with:
- NPCDCS – for hypertension, diabetes, cancers.
- National Mental Health Programme – dementia, depression.
- National Programme for Palliative Care (NPPC) – end-of-life care.
- National Programme for Control of Blindness and Deafness – cataract, hearing aids.
- Social welfare schemes such as National Policy on Older Persons, pensions, senior citizen helplines.
Human Resource and Training
- Doctors at PHC/CHC trained in basic geriatric care.
- Nurses and multipurpose workers trained in elderly-friendly communication, mobility support, and chronic disease management.
- Development of geriatric curriculum in medical colleges.
- Caregiver training for family members and community volunteers.
Monitoring and Evaluation
- Monthly and quarterly reports from PHC, CHC, and district hospitals.
- Key indicators include:
- Number of elderly screened and treated.
- Prevalence of hypertension/diabetes among elderly.
- Bed occupancy in geriatric wards.
- Number of physiotherapy sessions delivered.
- Annual review at the state and national levels.
Achievements So Far
- More than 20 Regional Geriatric Centres established.
- Geriatric clinics functional in hundreds of districts.
- Increased availability of physiotherapy and palliative care services.
- Elderly health issues have received greater visibility in health policy.
Challenges
Despite progress, the programme faces many challenges:
- Human resource shortages – limited specialists in geriatric medicine.
- Infrastructure gaps – not all districts have functional geriatric wards.
- Low community awareness – stigma around mental health, neglect of elderly.
- Financial sustainability – high cost of chronic care and assistive devices.
- Monitoring issues – underreporting of elderly morbidity data.
- Urban-rural disparities – services more accessible in urban areas.
Future Directions
- Strengthening home-based elderly care using telemedicine and community health workers.
- Universal screening of elderly for NCDs and disabilities at PHC level.
- Expansion of Regional Geriatric Centres to all states.
- Public-private partnerships for assistive devices and rehabilitation.
- Integration with insurance schemes like Ayushman Bharat.
- Promoting healthy ageing through lifestyle modification, social engagement, and age-friendly environments.
Global Perspective
- The WHO promotes Healthy Ageing 2015–2030 strategy, focusing on functional ability, social participation, and dignity.
- India’s NPHCE is aligned with the UN Decade of Healthy Ageing (2021–2030).
Conclusion
To conclude, the National Programme for Health Care of the Elderly is a landmark initiative aimed at ensuring dignity, independence, and quality of life for India’s ageing population. While implementation challenges remain, it provides a robust framework to address the growing health needs of the elderly.
As future public health professionals, you must not only be aware of the technical details of the programme but also advocate for age-friendly policies and practices in your communities.