YANGON, Myanmar — Health authorities in Myanmar have launched an aggressive screening and surveillance campaign at the country’s major international gateways following reports of a Nipah virus (NiV) outbreak in neighboring India. Effective Monday, February 2, 2026, travelers arriving at Yangon and Mandalay International Airports are undergoing enhanced health checks, with a specific focus on those arriving from West Bengal, India, where two cases were confirmed late last month.
The Ministry of Health (MOH) confirmed that while no suspected cases have been detected within Myanmar to date, the measures are a proactive effort to prevent the entry of a pathogen the World Health Organization (WHO) classifies as a “priority” due to its high fatality rate and epidemic potential.
Targeted Screening and Public Awareness
The current surveillance efforts are primarily focused on identifying travelers presenting with fever and respiratory distress—key early indicators of Nipah infection. According to The Global New Light of Myanmar, the Ministry of Health is operating under established international guidelines for infectious disease emergencies.
At Yangon International Airport, health teams are:
-
Monitoring temperatures: Using thermal scanners and handheld thermometers to identify febrile passengers.
-
Targeting high-risk routes: Providing intensive screening for travelers on direct flights from Kolkata, West Bengal.
-
Educational Outreach: Distributing informational leaflets and displaying posters in both Myanmar and English to educate the public on symptoms and prevention.
“These measures are being implemented in close coordination with airport departments to ensure that any potential threat is identified at the port of entry,” the Ministry stated.
The West Bengal Outbreak: What Triggered the Alert?
The heightened vigilance follows a notification from India’s National IHR Focal Point to the WHO on January 26, 2026. Two laboratory-confirmed cases of Nipah virus were identified in Barasat, North 24 Parganas district of West Bengal.
The patients, both 25-year-old nurses working at the same private hospital, developed severe neurological and respiratory symptoms in late December 2025. While one patient has shown signs of clinical improvement, the other remains on mechanical ventilation. In response, Indian authorities tested over 190 close contacts, all of whom have fortunately tested negative, suggesting that the current cluster remains contained.
A History of the Virus
Nipah virus is not new to the region. It was first identified in 1998 among pig farmers in Malaysia. Since 2001, it has become a recurring seasonal threat in Bangladesh and India, often linked to the consumption of raw date palm sap contaminated by fruit bats.
Understanding Nipah: Transmission and Symptoms
Nipah virus is a zoonotic disease, meaning it jumps from animals to humans. The natural reservoir for the virus is the Pteropus bat, commonly known as the fruit bat or “flying fox.”
How it Spreads:
-
Animal to Human: Through direct contact with infected bats or pigs, or their bodily fluids (saliva, urine).
-
Contaminated Food: Consuming fruit or date palm sap that has been bitten or soiled by infected bats.
-
Human to Human: Close contact with an infected person’s secretions. This is particularly a risk in healthcare settings and among family caregivers.
Symptoms to Watch For:
Infection usually presents after an incubation period of 4 to 14 days, though it can extend up to 45 days.
-
Early Phase: Fever, headache, muscle pain, vomiting, and sore throat.
-
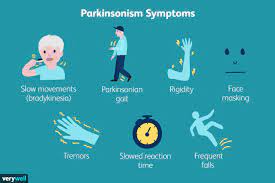
Late Phase: Dizziness, drowsiness, and altered consciousness.
-
Critical Phase: Acute encephalitis (brain swelling) and seizures, which can progress to a coma within 24 to 48 hours.
“The challenge with Nipah is that its initial symptoms are non-specific and can easily be mistaken for the flu or even COVID-19,” says Dr. Aris Thomas, an independent infectious disease consultant. “However, the rapid progression to neurological distress is a hallmark that requires immediate hospital intervention.”
The Medical Challenge: No Vaccine, High Fatality
One of the primary reasons for the international concern is the virus’s severity. The Case Fatality Rate (CFR) is estimated to be between 40% and 75%, depending on the quality of supportive care available.
Currently, there are no licensed vaccines or specific antiviral treatments for Nipah virus. Treatment is limited to “supportive care”—managing symptoms, maintaining hydration, and treating secondary infections.
However, medical science is making strides. As of early 2026, several vaccine candidates are in Phase II clinical trials in Bangladesh. Organizations like the Coalition for Epidemic Preparedness Innovations (CEPI) are funding research into monoclonal antibodies and vaccines, such as the ChAdOx1 NipahB candidate developed by the University of Oxford.
Public Health Implications and Practical Advice
For the general public in Myanmar and surrounding regions, the risk of infection remains low. Health authorities emphasize that the screening at airports is a safety net rather than a cause for panic.
How to Protect Yourself:
-
Wash Fruit Thoroughly: Peel and wash all fruits before consumption. Avoid fruit that appears to have bat bite marks.
-
Avoid Raw Sap: Do not consume raw date palm juice or sap, as bats often drink from collection containers at night.
-
Hand Hygiene: Regular handwashing with soap and water remains a primary defense against viral transmission.
-
Avoid Contact: Stay away from areas where bats are known to roost and avoid contact with sick livestock, especially pigs.
While the WHO assesses the global risk as low, the regional risk in South Asia is considered moderate due to the shared ecological corridor of fruit bats. The proactive steps taken by the Myanmar Ministry of Health serve as a critical barrier in maintaining national safety.
References
- https://tennews.in/myanmars-yangon-airport-tightens-screening-to-prevent-nipah-virus-entry/
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.