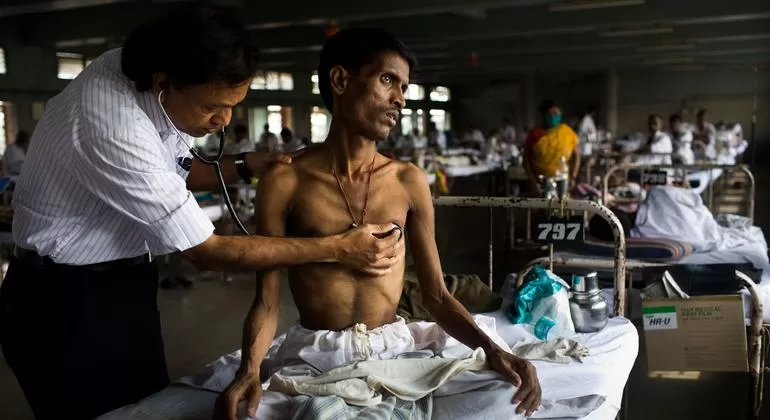
In the congested lanes of Govandi, Mumbai, a deadly health crisis persists. Tuberculosis (TB) continues to ravage families living in cramped, makeshift homes, with doctors estimating nearly every second household affected by the disease. This situation starkly highlights the broader national challenge as India, home to 27% of global TB cases, races against time to eliminate TB by 2025 — a goal now looking increasingly unattainable due to systemic healthcare gaps and socioeconomic barriers.
Key Findings and Developments
India’s battle against TB is formidable. According to the World Health Organization (WHO), India accounts for over a quarter of the world’s TB cases, with two deaths every three minutes caused by the disease. Despite the government’s ambitious pledge to eliminate TB five years ahead of the global schedule under the National Tuberculosis Elimination Programme (NTEP), progress faces many hurdles. Since 2015, India has reduced TB incidence by 17.7%, a significant achievement, yet the disease remains deeply entrenched, particularly in densely populated urban slums like Govandi, where living conditions facilitate transmission.
Patient voices underline the human toll. Mehboob Sheikh, diagnosed six months ago, lost his livelihood due to severe fatigue and weight loss, symptoms typical of untreated TB. Despite ongoing treatment, his condition remains fragile, compounded by economic hardship and delayed social support. Such stories highlight the intersection of health with poverty and social stigma — a barrier that keeps many from seeking timely diagnosis and treatment.
Expert Commentary
Dr. Lancelot Pinto, a noted respiratory specialist, cautions against overoptimism: “We do not necessarily have all the resources in place to scale up and eliminate TB by 2025.” He emphasizes that reliance on outdated diagnostic methods like sputum microscopy leaves many cases undetected, allowing drug-resistant forms to spread unchecked.
Health worker Pramila Pramod adds a social perspective, noting the stigma attached to TB: “Families hide diagnoses, particularly fearing marriage prospects for young women.” This stigma undermines public health efforts and facilitates continued transmission in communities.
Context and Background
India’s NTEP, renamed in 2020 from the Revised National TB Control Programme, aims to accelerate detection, treatment, prevention, and capacity building with a patient-centered approach. The program follows a National Strategic Plan targeting an 80% reduction in TB incidence by 2025 and incorporates innovative tools, partnerships, and financial support for affected individuals. Despite these efforts, challenges persist, including staff shortages, poor mapping of high-risk areas, and disruptions wrought by the COVID-19 pandemic.
Socioeconomic factors exacerbate India’s TB burden. Overcrowding, malnutrition, and poverty create fertile ground for TB spread. In slums like Govandi, housing made from tarpaulin and salvaged wood with limited ventilation perpetuates airborne transmission. Moreover, a recently published international study revealed toxic pollution from a nearby biomedical waste plant further aggravates respiratory illnesses, compounding the TB crisis.
Innovative Solutions
New technologies are offering hope. AI-powered portable handheld X-ray machines have revolutionized TB screening in underserved areas. These devices are lightweight—less than 3.5 kilograms—and battery-operated, making them easy to transport in backpacks for outreach in slums and remote regions. Nearly 5 million X-rays have been conducted using such technology, helping detect cases earlier and more efficiently than previous methods.
Dr. Shibu Vijayan of Qure.ai highlights the impact: “These machines have drastically reduced the gap between symptom onset and diagnosis, enabling health workers to reach vulnerable populations directly.” The handheld X-rays have a diagnostic accuracy of approximately 90%, significantly aiding in TB identification and prompt treatment initiation.
Public Health Implications
Despite innovative strides, India’s TB elimination goals hinge on addressing systemic issues. Reliable healthcare delivery with well-trained staff, robust mapping and surveillance of high-risk areas, and overcoming social stigma remain critical. Financial support like the government’s monthly cash assistance to patients is crucial but inconsistently delivered, as patients like Mehboob Sheikh continue to struggle with basic survival needs alongside treatment.
The National TB Elimination Programme’s integrated approach—spanning improved diagnosis, patient support, and multi-sector partnerships—must be sustained and scaled. Failure to do so risks perpetuating TB’s spread in vulnerable communities and undermining national and global health targets.
Limitations and Counterarguments
India’s progress is notable but unevenly distributed. Critics argue government spending on TB elimination remains insufficient relative to needs, and essential drug and diagnostic supplies have experienced shortages, hampering treatment continuity. Additionally, some experts warn that ambitious timelines may overlook complex local challenges, suggesting a more flexible goal could allow for stronger groundwork and sustainable elimination efforts by 2030—the WHO’s global target.
Practical Takeaways for Readers
For health-conscious individuals and healthcare professionals alike, the persistent TB crisis in India underscores the importance of early diagnosis, adherence to treatment, and combatting stigma through education. Vigilance in crowded, high-risk settings and nutrition support also play vital roles in prevention. Technological advances like handheld AI X-rays provide tools for frontline health workers but addressing underlying social and systemic factors will determine long-term success.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Daijiworld. “Mumbai slums battle tuberculosis as India struggles to meet 2025 goal.” September 21, 2025. https://daijiworld.com/news/newsDisplay?newsID=1292933