The World Health Organization (WHO) recently reported an alarming surge of mpox (monkeypox) in Africa, documenting active transmission in 17 countries with 2,862 confirmed cases and 17 deaths recorded between September 14 and October 19, 2025. This resurgence underscores the continuing public health threat posed by mpox, a viral disease that has zoonotic origins and typically causes mild to moderate illness but can lead to fatalities.
Understanding the 2025 Mpox Spike in Africa
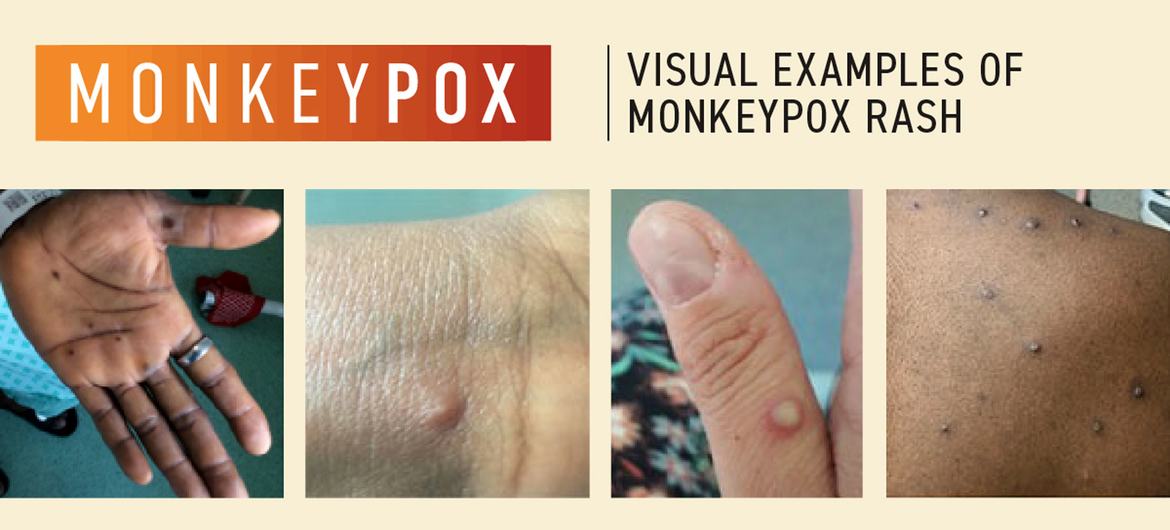
Mpox, caused by the mpox virus (MPXV), is transmitted through close physical contact, such as skin-to-skin interactions and exposure to respiratory droplets. It is characterized by symptoms that start with fever, malaise, and swollen lymph nodes, progressing to distinctive pus-filled skin lesions. Generally, the infection lasts two to four weeks, but immunocompromised individuals may experience prolonged or severe illness.
Between mid-September and mid-October 2025, the WHO’s Africa regional office documented ongoing mpox transmission in multiple African countries, including the Democratic Republic of the Congo (DRC), Liberia, Kenya, and Ghana. The DRC remains the epicenter, with some countries showing rising case numbers, such as Kenya and Liberia, while others like the DRC and Ghana report early signs of decline. The cumulative case fatality ratio during this period stands at approximately 0.6%, a reminder of the disease’s potential severity in some populations.
Adding complexity to the outbreak is the presence of multiple viral clades—genetic variants of the mpox virus. The DRC continues to report the Clade 1b variant, which experts believe may be more easily transmitted and possibly associated with greater morbidity. This variant predominantly spreads via human-to-human transmission, including sexual networks, as noted by WHO officials.
Expert Insights and Public Health Implications
Dr. Anne Mwangi, an infectious disease epidemiologist not involved with the WHO report, explains, “The sustained transmission of mpox in Africa reflects both biological factors of the virus and substantial challenges within healthcare systems, including limited surveillance, insufficient medical supplies, and community health-seeking behaviors.”
The ongoing conflict and displacement in parts of Central Africa, particularly in eastern DRC, exacerbate transmission risks and hinder effective public health responses. Displaced populations face overcrowded living conditions with limited access to healthcare, which facilitates the spread of mpox and other infectious diseases.
The Africa Centres for Disease Control and Prevention (Africa CDC) declared the mpox outbreak a public health emergency of continental security in August 2024, a designation reflecting its severity and need for coordinated response strategies. By August 2025, Africa CDC reported over 174,000 suspected cases and 1,900 deaths since the outbreak’s escalation in 2024, further emphasizing the scope of the crisis.
Broader Context and Global Concerns
Though the African continent remains the primary locus, mpox cases have been confirmed in various non-African countries, sometimes linked to travel or importation of infected animals. The WHO continues to monitor global trends, underscoring the importance of international cooperation and comprehensive surveillance to contain outbreaks and prevent wider spread.
The WHO Director-General, Dr. Tedros Adhanom Ghebreyesus, has emphasized that despite the end of the mpox public health emergency designation in some regions, the potential for resurgent waves persists, highlighting the need for ongoing vigilance and integration of mpox prevention into broader health systems.
Practical Guidance for Readers
For the general public and health professionals alike, awareness of mpox transmission and prevention is key. Since the virus transmits primarily through close contact, avoiding direct exposure to skin lesions or materials contaminated with the virus is advised. Good hygiene practices, including hand washing and disinfecting surfaces, can reduce risk, especially in households with infected individuals.
Vaccines initially developed for smallpox have shown cross-protection against mpox, and antiviral treatments exist, though sometimes access is limited in resource-constrained settings. Early diagnosis and isolation of cases remain critical for controlling spread.
Limitations and Ongoing Challenges
Despite advances in understanding mpox, challenges remain. Underreporting due to limited diagnostics, stigma, and variable health infrastructure complicate accurate epidemiological assessments. Researchers continue to study the virus’s evolving genetics and transmission dynamics to refine public health responses. The role of animal reservoirs and environmental factors also requires further investigation.
Conclusion
The recent WHO report on mpox in Africa serves as a crucial reminder of the persistent threats posed by emerging and re-emerging infectious diseases. Effective response demands robust surveillance, community engagement, international support, and sustained investment in healthcare infrastructure to mitigate impact and save lives.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Reuters. “WHO says mpox now detected in more countries, with 17 deaths in Africa over six weeks.” October 31, 2025.