ADDIS ABABA, Sept. 19, 2025 — Africa has crossed a sobering threshold in its fight against mpox: more than 190,000 reported cases and nearly 2,000 deaths since January 2024. The update, announced Thursday evening by the Africa Centers for Disease Control and Prevention (Africa CDC), underscores both the scale of the outbreak and the continent’s improving ability to contain it.
At an online media briefing, Dr. Yap Boum II, deputy incident manager for mpox at the Africa CDC, said 29 countries have reported 191,559 cases, including 53,013 laboratory-confirmed infections and 1,999 deaths.
“We are starting to see encouraging progress. Weekly confirmed cases have dropped by 70 percent since May, which demonstrates that current interventions are working,” Boum said.
Mpox in Africa: Turning the Tide?
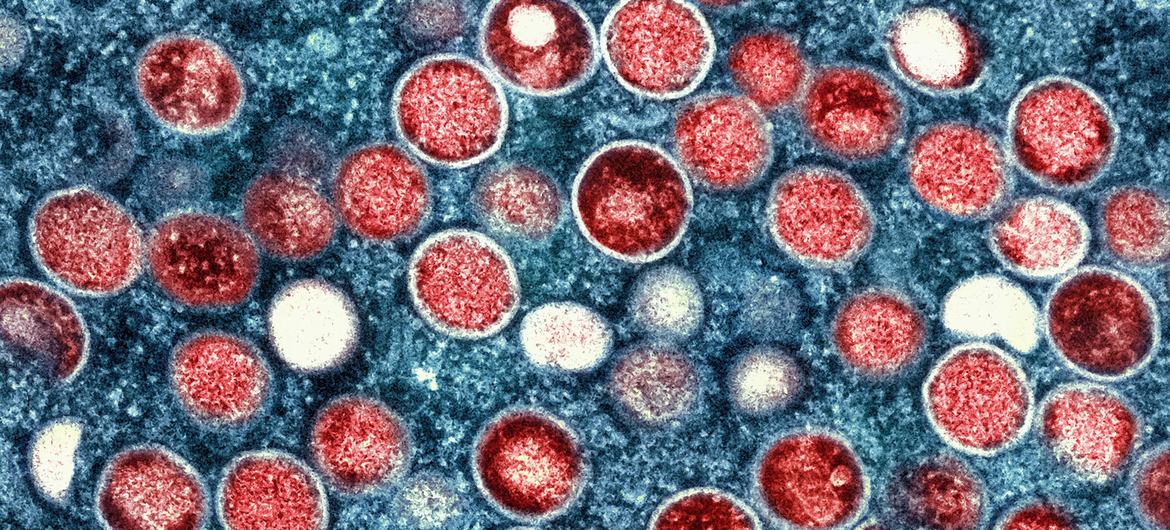
Mpox, formerly known as monkeypox, is a viral illness caused by the mpox virus, belonging to the same family as smallpox but clinically less severe. Symptoms include fever, headache, swollen lymph nodes, and a characteristic rash that progresses through several stages before crusting over and healing.
The outbreak in Africa surged in early 2024, peaking in May when weekly confirmed cases reached 1,620. Since then, numbers have steadily declined to 491 last week, according to Africa CDC figures.
Public health experts say improved testing coverage, case detection, and treatment protocols have helped slow transmission. Routine contact tracing and community education campaigns on safe caregiving practices are also believed to be contributing to this decline.
Geographic Spread and Vulnerable Communities
While mpox cases have been documented across 29 countries, the heaviest burden remains in Central and West Africa, where the virus has been endemic for decades. Countries such as the Democratic Republic of the Congo (DRC) and Nigeria continue to report the highest numbers.
Children and individuals with compromised immune systems remain at heightened risk of severe illness and death. According to WHO data, case fatality rates in Central Africa can range from 3–6 percent, depending on access to healthcare.
Dr. Chikwe Ihekweazu, Assistant Director-General for the WHO Health Emergency Programme, who was not involved in Africa CDC’s data collection, stressed the need to prioritize vulnerable populations:
“Declining case numbers are hopeful, but the virus has not disappeared. Protecting children, immunocompromised patients, and rural communities with limited health access is critical to ending this outbreak,” he said.
Ebola Outbreak Adds to Regional Challenges
In a parallel development, the World Health Organization (WHO) reported a new Ebola outbreak in the Democratic Republic of the Congo’s Kasai province, with 48 identified cases and 31 deaths as of Thursday.
According to Dr. Patrick Otim from WHO’s Regional Office for Africa, 38 patients have been laboratory-confirmed, 15 remain under treatment at an Ebola center in Bulape, and two patients have successfully recovered.
Ebola, a viral hemorrhagic fever with case fatality rates averaging 50 percent in past outbreaks, presents a severe challenge to overstretched health systems. Symptoms such as fever, weakness, vomiting, diarrhea, and internal or external bleeding make rapid detection vital.
Dr. Boum underscored the importance of timely response:
“We must identify all suspected Ebola cases early, isolate patients, and provide appropriate care. Each recovered patient is a reminder that with proper treatment and community cooperation, survival is possible.”
Public Health Implications
Africa’s double burden of infectious diseases—managing a widespread mpox outbreak while confronting new Ebola clusters—highlights vulnerabilities in public health infrastructure.
-
Testing and Surveillance: Expanded testing programs for mpox have improved diagnostic accuracy but remain uneven across rural areas. Ebola, with its capacity for rapid spread, calls for more robust surveillance systems.
-
Community Engagement: Both diseases rely heavily on public understanding. Misinformation, stigma, and caregiving practices in close-knit communities can increase transmission risk.
-
Vaccination and Treatment: While smallpox vaccines have shown cross-protection against mpox, vaccine access in African countries has been limited. For Ebola, experimental vaccines and monoclonal antibody treatments exist but are still not widely accessible in Kasai’s outbreak zone.
Counterpoints and Limitations
Although trends suggest that mpox infections are slowing, epidemiologists caution against complacency. Some key limitations remain:
-
Under-Reporting: Due to weak healthcare access in remote communities, actual mpox and Ebola cases may be higher than recorded.
-
Vaccine Inequity: Global vaccine distribution has favored wealthier nations, leaving Africa with limited resources for prevention.
-
Mutation Risks: Both viruses, particularly mpox, have shown potential for genetic variation. Although current strains have not demonstrated alarming new behaviors, continuous monitoring is essential.
Dr. Afsatou Ndoye, an infectious disease specialist at Dakar’s Fann Hospital, emphasized vigilance:
“Disease curves can be deceptive. Declines are encouraging, but until health systems can quickly detect and respond to new clusters, we remain vulnerable to resurgence.”
What This Means for the Public
For residents in Africa and beyond, the key message is continued vigilance. While declining mpox trends suggest outbreak control measures are working, individuals should remain attentive to prevention strategies:
-
Seek medical attention promptly if symptoms such as fever, rash, or swollen lymph nodes develop.
-
Follow official public health guidance on isolation and caregiving for sick family members.
-
Stay informed about vaccination campaigns where available.
-
Support community health workers by reporting suspected cases quickly.
For Ebola in Kasai, the WHO emphasizes avoiding direct contact with bodily fluids of sick individuals and encouraging immediate referral to treatment centers for suspected cases.
As both outbreaks evolve, experts remain cautiously optimistic. The decline in mpox cases provides hope, while early detection of Ebola may help prevent a larger crisis. Africa CDC and WHO stress that collaboration between governments, local communities, and global partners will determine whether these gains can be sustained.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Africa CDC. Media briefing on mpox response. September 19, 2025.