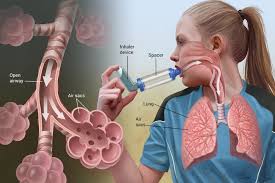
SAN DIEGO — Obesity not only increases the risk of asthma but also worsens symptoms and responses to standard controller medications. Despite this, most physicians fail to address weight management when treating asthma patients with obesity, according to research presented on March 2 at the American Academy of Allergy, Asthma, & Immunology (AAAAI) 2025 Annual Meeting in San Diego.
More than 40% of adults and nearly 20% of children in the United States are obese. The Global Initiative for Asthma (GINA) guidelines recommend incorporating weight reduction in asthma treatment plans for individuals with obesity, highlighting that even a 5%-10% weight loss can significantly improve asthma control. Additionally, recent approvals from the US Food and Drug Administration (FDA) have sparked public interest in weight loss medications.
To evaluate how well these guidelines are implemented in clinical practice, researchers at Brigham & Women’s Hospital in Boston examined electronic health records of adult patients with asthma and obesity. Using OpenAI’s GPT-4o, the team analyzed free-text notes from primary care, allergy/immunology, and pulmonary specialists who treated these patients between January 2020 and September 2023.
The researchers’ AI-assisted analysis sought to answer key questions: Was asthma discussed in the patient encounter? If so, was obesity management addressed? If weight management was discussed, what strategies were suggested? And finally, was weight loss mentioned in the context of asthma?
Out of 17,660 outpatient asthma-related encounters, only 25.8% included discussions on obesity management. Among this subset, fewer than half linked weight loss to asthma care. Ultimately, just 12.6% (2,219 of 17,660) of patients with obesity and asthma had a documented conversation with their healthcare provider about weight loss as a strategy to improve asthma symptoms, reported lead author Oluwatobi Olayiwola, MD, an allergy/immunology fellow at Brigham & Women’s Hospital.
The study also found that weight management discussions were only slightly more common during in-person visits compared to telemedicine appointments. Pulmonary specialists were the most likely to address obesity management, whereas allergy/immunology providers were the least likely to do so. However, when allergy specialists did discuss weight loss, they were more likely to connect it to asthma treatment.
Olayiwola acknowledged a potential limitation of the study: the reliance on written documentation. “Just because things aren’t written down doesn’t mean they’re not being discussed,” she noted. “We’re all busy. We don’t always type every single word.”
The findings struck a chord with meeting attendees. Ama Alexis, MD, clinical assistant professor of pediatrics at Weill Cornell Medical College and allergist/immunologist at Hudson Allergy in New York, called the data “important.” She emphasized the need to normalize discussions about obesity management as part of comprehensive asthma care, particularly as more patients adopt GLP-1 receptor agonists for weight loss.
Looking ahead, Olayiwola and her colleagues plan to explore whether proactively discussing obesity management leads to tangible patient outcomes, such as improved asthma control, weight loss, or reduced reliance on biologic therapies and inhaled corticosteroids.
Olayiwola and Alexis disclosed no relevant financial relationships.
Disclaimer: This article is based on preliminary research presented at a scientific conference. The findings have not yet been published in a peer-reviewed journal and should not be interpreted as definitive medical advice. Patients should consult their healthcare providers before making any changes to their treatment plans.