New Delhi – In a significant shift from viewing bariatric procedures solely as weight-loss interventions, leading medical experts are now championing metabolic surgery as a critical defense against organ failure for patients with uncontrolled Type 2 diabetes. According to Dr. Manjunath Maruti Pol, Additional Professor in the Department of Surgery at the All India Institute of Medical Sciences (AIIMS), New Delhi, this surgical intervention effectively halts the progression of life-threatening complications, offering a lifeline where medication alone fails.
The Silent Crisis of Uncontrolled Diabetes
India, frequently dubbed the “diabetes capital of the world,” faces a staggering public health challenge. Estimates suggest over 70 million Indians live with diabetes, with recent studies, such as those by the Indian Council of Medical Research (ICMR), indicating the true burden could be even higher.
The most alarming statistic, however, is not the prevalence but the control. Dr. Pol highlights that nearly 50% of these patients suffer from “uncontrolled diabetes,” defined as maintaining an HbA1c level (a three-month average of blood sugar) above 7.5% despite adhering to a regimen of three or more medications and lifestyle modifications for at least two years.
“HbA1c is inversely related to the occurrence of complications,” Dr. Pol explained in a recent statement. “If HbA1c increases, organs will begin to fail in a short duration, leading to death.”
Unchecked high blood glucose acts as a slow poison to the body’s vascular system, leading to:
-
Nephropathy: Kidney damage often requiring dialysis or transplant.
-
Retinopathy: Vision loss and blindness.
-
Neuropathy: Nerve damage leading to amputation.
-
Cardiovascular Disease: Significantly higher risk of heart attacks and strokes.
Beyond Weight Loss: The Science of Metabolic Surgery
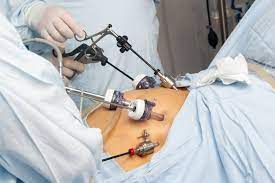
While traditionally known as “weight-loss surgery,” the procedure’s impact on diabetes goes far beyond the weighing scale. Dr. Pol notes that metabolic surgery—specifically procedures like the Roux-en-Y gastric bypass or sleeve gastrectomy—alters the patient’s gastrointestinal anatomy in a way that fundamentally changes their metabolism.
The surgery typically involves reducing the stomach size and rerouting the small intestine to bypass the duodenum (the first section of the small intestine). This anatomical change triggers a powerful hormonal response.
“When food goes directly to the intestine, bypassing the duodenum, there is a release of certain hormones like GLP-1 (Glucagon-like peptide-1) in a physiological dose and rhythm,” Dr. Pol stated.
These “incretin” hormones stimulate the pancreas to produce insulin more effectively and decrease insulin resistance. Crucially, these metabolic benefits often appear within days of the surgery—long before significant weight loss occurs—proving the effects are “weight-independent.”
Clinical Evidence and Global Consensus
The medical community’s stance on this intervention has evolved rapidly. In 2016, the International Diabetes Federation (IDF) and massive consensus bodies like the Diabetes Surgery Summit (DSS-II) formally recognized metabolic surgery as a standard treatment option for appropriate candidates.
Guidelines now recommend surgery for:
-
Patients with a BMI ≥ 40 (Class III obesity), regardless of glycemic control.
-
Patients with a BMI of 35.0–39.9 with inadequately controlled hyperglycemia.
-
Consideration for patients with a BMI of 30.0–34.9 with uncontrolled Type 2 diabetes.
Data from AIIMS reinforces these global findings. In a retrospective analysis of over 100 surgeries performed by Dr. Pol’s team, 35% were on patients with uncontrolled Type 2 diabetes. The result? “All of them are currently off diabetes medications,” Dr. Pol confirmed, citing near-normal blood sugar levels often observed as early as the first post-operative day.
A Comparative Perspective: Surgery vs. Medication
While modern pharmacology has produced potent drugs like Ozempic and Mounjaro (GLP-1 receptor agonists) that mimic the very hormones stimulated by surgery, long-term data suggests surgery may still hold the upper hand for organ protection.
A landmark study published in JAMA and recent findings from the Cleveland Clinic (2025) suggest that while medications are effective, metabolic surgery is associated with a lower cumulative incidence of macrovascular and microvascular complications over a 10-year period compared to medical therapy alone.
Dr. Ali Aminian, a global expert in metabolic surgery (not involved in the AIIMS report), has noted in similar research contexts that surgery essentially “resets” the metabolic thermostat, providing a durability that daily medication compliance struggles to match.
Barriers, Risks, and the Path Forward
Despite the clear benefits, metabolic surgery is not a magic bullet, nor is it without risk. It is a major surgical procedure costing between ₹3 to ₹6 lakhs in private settings (though subsidized in government institutions like AIIMS).
Potential limitations and risks include:
-
Nutritional Deficiencies: Patients must take multivitamins, calcium, and iron supplements for life to prevent malnutrition.
-
Surgical Risks: As with any surgery, there are risks of infection, bleeding, or leaks, though laparoscopic and robotic techniques have minimized these.
-
Not a Guaranteed Cure: While “remission” is common, diabetes can relapse if lifestyle changes are not maintained.
Furthermore, access remains a hurdle. With millions of potential candidates and limited specialized centers, scaling this solution is a challenge for India’s healthcare infrastructure.
Conclusion
For patients trapped in the cycle of escalating insulin doses and deteriorating health, Dr. Pol’s message is one of hope and urgency. Metabolic surgery is no longer just about fitting into smaller clothes; it is about saving kidneys, hearts, and lives. As the burden of diabetes grows, integrating this surgical “organ shield” into standard diabetic care could define the next decade of public health in India.
Medical Disclaimer:
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References:
-
Primary Source: Ten News Network. (2025, December 10). Metabolic surgery can help prevent organ damage, failure due to uncontrolled diabetes: AIIMS doctor. Retrieved from https://tennews.in