Australia is witnessing a significant surge in measles cases in 2025, raising alarms about declining vaccination rates and potential threats to herd immunity. As of early October, there have been 133 confirmed measles cases reported this year, compared to 57 in 2024 and just 26 in 2023. This rise comes more than a decade after the World Health Organization (WHO) declared Australia free of endemic measles, spotlighting the challenges posed by waning immunization coverage and global viral spread.
Key Developments and Statistics
Measles, caused by the Morbillivirus, is one of the most contagious human pathogens, with an infected individual capable of spreading the virus to 12 to 18 others in an unvaccinated population. The WHO recommends at least 95% two-dose vaccination coverage to maintain herd immunity and prevent outbreaks. However, vaccination rates in Australia have declined since the COVID-19 pandemic. Pre-pandemic measles vaccine coverage at two years of age was about 94%, but this dropped to approximately 92.5% in 2023, with some regions experiencing rates as low as 70%-75%. Moreover, delays in timely vaccination mean that one in three children received their first dose late in 2024, increasing their susceptibility to infection.
The recent spike in cases is partly attributed to imported infections linked to international travel, affecting not only adults but also children too young to be vaccinated. Regions with notably low vaccination coverage, including parts of New South Wales, Queensland’s Gold Coast, Northern Territory Indigenous communities, and pockets in major cities like Melbourne and Sydney, are particularly vulnerable to outbreaks. Western Australia has also reported 47 cases this year, including a concerning cluster in the Pilbara region with cases linked to mining workforce travel.
Expert Insights
Josh Davis, MD, PhD, infectious disease specialist at the University of Newcastle, emphasized the virus’s infectiousness, describing measles as spreading “like wildfire” in under-vaccinated populations. He noted, “Although the current number of cases might seem small, it forms part of a worrying trend that threatens to erode herd immunity”.
Frank Beard, MBChB, associate professor at the University of Sydney and associate director at Australia’s National Centre for Immunisation Research and Surveillance, highlighted the consequences of decreased immunization. He pointed to barriers such as appointment difficulties, costs, and vaccine hesitancy fueled by misinformation and trust issues leading some parents to delay or forgo vaccination for their children.
Professor Margie Danchin at Murdoch Children’s Research Institute described the decline in childhood vaccination coverage since the pandemic as a “huge concern,” warning that although Australia’s endemic measles-free status is not yet at immediate risk, the potential for wider spread is increasing. She stressed that pockets of low coverage serve as tinder for outbreaks given the virus’s extraordinary contagiousness.
Public Health Context and Implications
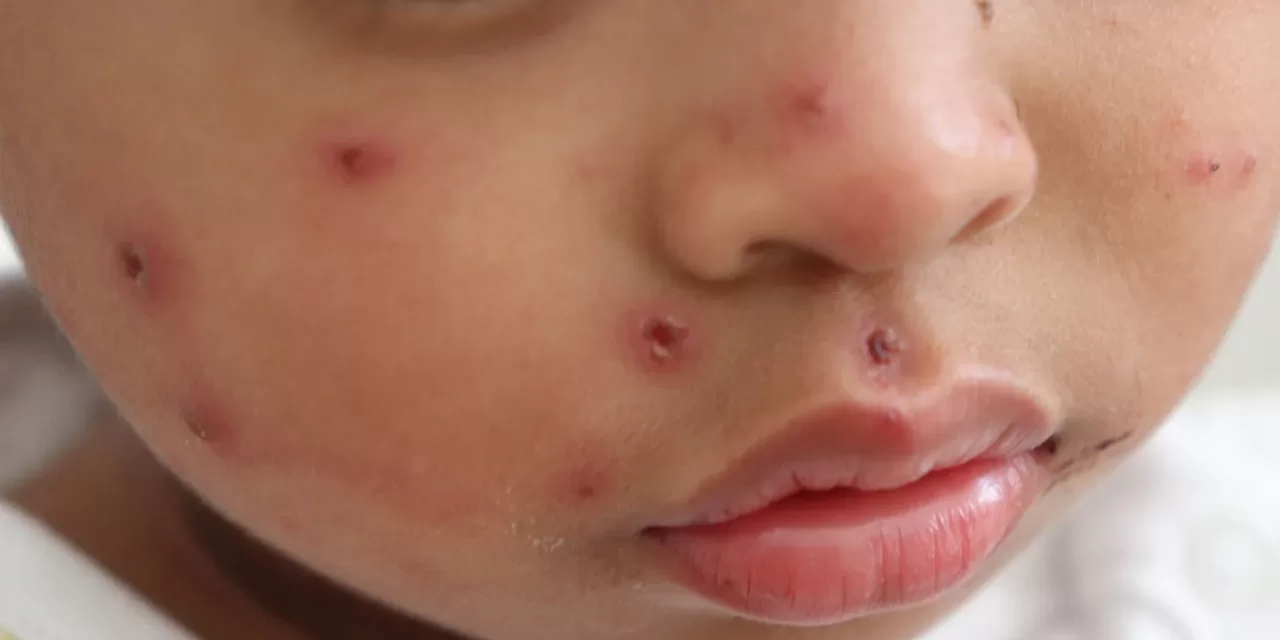
Measles symptoms include fever, cough, runny nose, conjunctivitis, and a characteristic rash. While often mild, measles can lead to severe complications including pneumonia, encephalitis, and death, particularly in young children and immunocompromised individuals. It also has long-term effects such as immunosuppression that can increase vulnerability to other infections.
The resurgence of measles underscores the critical role of consistent, high vaccination coverage in preventing outbreaks. Herd immunity protects even those who cannot be vaccinated, such as infants under 12 months. The WHO’s threshold of 95% coverage is based on measles’ high transmissibility, and falling short risks outbreaks that strain healthcare resources and endanger vulnerable populations.
The spread of measles also has broader implications for other vaccine-preventable diseases, such as rubella, which may circulate simultaneously and complicate clinical diagnosis. Health experts urge adherence to recommended vaccination schedules and recommend that travelers verify immunity before international trips to mitigate the risk of importing infections.
Limitations and Counterpoints
While the rise in cases is concerning, experts caution that not all areas are equally affected, and many outbreaks have been contained thus far. Some argue that catch-up vaccination campaigns and heightened surveillance can prevent a full return to endemic measles. Also, some adults may have natural immunity from past infection, and vaccination programs remain robust in most parts of Australia.
However, ongoing vaccine hesitancy and structural barriers to access remain challenges. Continuous public health efforts to address misinformation, facilitate access, and encourage timely vaccination are essential to reversing current trends.
Practical Takeaways for Readers
For the public, ensuring that children receive the two recommended doses of the MMR vaccine on schedule (12 and 18 months) remains critical. Adults who are unsure about their immunity should seek medical advice, especially before travel. Recognizing early symptoms and avoiding contact with vulnerable individuals can help limit spread. Staying informed through reliable health authorities and participating in community vaccination efforts supports collective protection.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References