Lyme disease, the leading vector-borne illness in the United States, presents a significant public health challenge, with an estimated 476,000 people potentially contracting it each year, according to the US Centers for Disease Control and Prevention (CDC). This multisystem illness, primarily caused by the Borrelia burgdorferi spirochete and the body’s immune response, is transmitted to humans through the bites of infected Ixodes ticks. Understanding its transmission, varied symptoms, diagnostic procedures, and treatment options is crucial for prevention and effective management.
Understanding Transmission and Risk
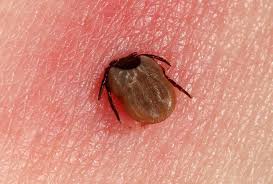
Lyme disease is transmitted when an infected tick, typically from the Ixodes genus (commonly known as deer ticks), bites a human. In the northeastern and upper midwestern United States, Ixodes scapularis is the primary vector, while Ixodes pacificus is responsible in the northwest. The tick lifecycle is a critical factor, with nymphs (about the size of a poppy seed) accounting for 90% of human disease transmissions due to their abundance, increased human outdoor activity during their peak feeding season, and their small size making them difficult to detect.
For transmission to occur, nymphs typically need to feed for 36-48 hours, and adult ticks for 48-72 hours. This lengthy attachment time underscores the importance of prompt tick removal. Despite this, only about 25-30% of US patients with early Lyme disease recall a tick bite. The risk of contracting Lyme disease is highest from May through November, particularly for individuals who spend time outdoors in wooded, brushy, or grassy habitats in endemic areas.
Symptoms Vary by Disease Stage
The clinical manifestations of Lyme disease are categorized into three stages, each with distinct symptoms:
- Stage 1: Early Localized Disease (1-30 days post-tick bite)
- Erythema migrans (EM): This is the characteristic skin rash of Lyme disease, occurring in about two-thirds of patients, typically 7 days after the bite. While often depicted as a “bull’s-eye” with central clearing, in the United States, EM is more likely to have a uniform red color. These rashes usually expand over days and can appear in less visible areas like the armpit, groin, or hairline.
- Flu-like symptoms: Patients may also experience fever, chills, malaise, muscle aches (myalgias), joint pain (arthralgia), headache, and tender local lymph nodes.
- Stage 2: Early Disseminated Disease (3-10 weeks after inoculation)
- Multiple Erythema Migrans lesions: About 20% of patients may develop additional, smaller rashes.
- Musculoskeletal symptoms: Intermittent inflammatory arthritis, often migratory, typically affecting large joints like the knee, ankle, and wrist.
- Neurologic manifestations (Lyme neuroborreliosis): Occurring in 5-20% of cases, the most common is cranial neuropathy, particularly facial nerve palsy (Bell palsy), which can be bilateral in 35% of patients. Meningitis (headache, neck stiffness, photophobia) and encephalopathy (memory/concentration issues, mood disturbances) can also occur.
- Cardiac involvement (Lyme carditis): This typically manifests as heart block, which can cause dizziness, fainting, shortness of breath, or chest pain.
- Stage 3: Late or Chronic Lyme Disease (months to years after initial infection)
- Lyme arthritis: This is the hallmark of late-stage disease, usually affecting large joints, with the knee involved in 90% of cases.
- Neurologic abnormalities: Subacute encephalopathy, chronic progressive encephalomyelitis, and late axonal neuropathies are common, with symptoms potentially resembling fibromyalgia.
- Acrodermatitis chronica atrophicans (ACA): Almost exclusively seen in European patients, this cutaneous feature involves an inflammatory phase followed by skin atrophy, leading to a “cigarette-paper skin” appearance.
Diagnosis: A Two-Step Process
In endemic areas, patients presenting with probable erythema migrans and recent tick exposure should begin treatment without blood tests. For other suspected cases, the CDC recommends a two-tier serologic testing procedure:
- Step 1: Enzyme Immunoassay (EIA) or Immunofluorescence Assay (IFA) to screen for Lyme antibodies.
- Step 2: Western blot testing if the first step is positive or equivocal. If symptoms have been present for 30 days or less, both IgM and IgG Western blots are performed; if longer than 30 days, only IgG Western blot is needed.
The US Food & Drug Administration (FDA) has also approved a modified two-tier test using concurrent or sequential EIA testing as equally accurate. Other diagnostic tests like joint aspiration, cerebrospinal fluid (CSF) analysis, and electrocardiograms (ECGs) may be used depending on the patient’s symptoms. Polymerase Chain Reaction (PCR) testing can detect B. burgdorferi DNA but is largely a research technique with low sensitivity in many clinical settings, except for synovial fluid.
Treatment: Antibiotics Are Key
With appropriate antibiotic treatment, most patients with early-stage Lyme disease recover rapidly and completely. The choice, route, and duration of antibiotics are guided by the patient’s clinical manifestations and disease stage.
- Early Localized or Early Disseminated Lyme Disease (with EM): Oral doxycycline, amoxicillin, or cefuroxime axetil for 10-14 days. Doxycycline is generally contraindicated in children under 8 years and pregnant/nursing women, for whom amoxicillin or cefuroxime axetil are preferred.
- Neurologic Lyme Disease: Intravenous (IV) penicillin, ceftriaxone, or cefotaxime are typically used for 14-21 days. Oral doxycycline may be effective for Lyme-associated meningitis, facial nerve palsy, or radiculitis.
- Lyme Arthritis: Oral antibiotics for 28 days are the standard. Refractory cases may require IV antibiotics or, if PCR is negative, symptomatic treatment with NSAIDs and potentially hydroxychloroquine.
- Lyme Carditis: Oral or parenteral antibiotic therapy for 14-21 days is recommended. Patients with severe cardiac complications, such as second- or third-degree AV block, require hospitalization, continuous monitoring, and possibly temporary cardiac pacing.
Prevention Strategies
Prevention is paramount due to the increasing incidence of Lyme disease. Personal strategies include:
- Tick Avoidance: Staying on marked trails in wooded areas, wearing long-sleeved shirts and tucking pants into socks, and wearing light-colored clothing to spot ticks easily.
- Repellents: Using products containing DEET, picaridin, IR3535, or oil of lemon eucalyptus on skin or clothing. Permethrin can be applied to clothing.
- Daily Tick Inspection and Prompt Removal: Crucial after outdoor activities. Use fine-tipped forceps to grasp the tick as close to the skin as possible and pull upward with steady, even traction. Avoid twisting, jerking, squeezing, crushing, or using heat/substances like petroleum jelly, as these can increase infection risk.
- Antibiotic Prophylaxis: A single dose of oral doxycycline (200 mg for adults, 4.4 mg/kg for children up to 200 mg) may be considered within 72 hours of removing an Ixodes tick in a highly endemic area, provided the tick was attached for at least 36 hours and doxycycline is not contraindicated. Routine prophylaxis is not recommended