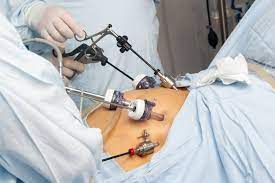
COPENHAGEN — A landmark multi-decades-long study spanning three Nordic countries has identified a significant, though rare, long-term health risk for patients undergoing gastric bypass surgery. While the procedure remains a gold standard for treating severe obesity and type 2 diabetes, researchers found that the risk of developing a specific, rare form of stomach cancer in the “bypassed” portion of the organ begins to climb more than a decade after the initial operation.
The study, published recently and drawing on comprehensive national registries from Denmark, Finland, and Sweden, tracked over 100,000 bariatric surgery patients for up to 44 years. The findings underscore a critical challenge in post-operative care: the very anatomical changes that help patients lose weight may also hide developing tumors from standard diagnostic tools.
Understanding the “Excluded” Risk
In a standard Roux-en-Y gastric bypass, surgeons create a small pouch from the upper stomach and connect it directly to the small intestine. This leaves a large portion of the stomach “excluded” or bypassed. While this bypassed section still produces digestive juices, it no longer comes into contact with food.
The Nordic research team analyzed data from 109,097 patients, comparing 82,394 gastric bypass procedures against 26,703 other types of weight-loss surgeries. Their focus was on gastric non-cardia adenocarcinoma—a cancer that occurs in the main body of the stomach.
The results revealed a “sleeper” effect:
-
Years 1–9 Post-Surgery: There was no detectable increase in cancer risk compared to the general population.
-
Years 10–44 Post-Surgery: The risk of this specific cancer jumped significantly. Patients who had undergone gastric bypass were four times more likely (Adjusted Hazard Ratio: 4.0) to develop the malignancy than those who had other bariatric procedures.
When compared to the general population, the incidence was 2.5 times higher than expected during this later period.
The “Blind Spot” Problem
The most concerning aspect of the study is not just the occurrence of the cancer, but the difficulty in diagnosing it. Because the bypassed stomach is no longer connected to the esophagus, it cannot be reached by a standard endoscope—the flexible camera tube typically used to screen for stomach issues.
“The anatomy of a gastric bypass creates a diagnostic ‘blind spot,'” says Dr. Aris Ioannides, a gastroenterologist not involved in the study. “If a patient develops symptoms like pain or internal bleeding in that excluded section, we can’t simply ‘look’ inside with routine tools. This often leads to a delayed diagnosis, which we see reflected in the study’s mortality data.”
Indeed, the study found that patients who developed cancer in the bypassed stomach had less favorable outcomes. They were less likely to undergo a gastrectomy (surgical removal of the cancer) and faced a nearly two-fold increase in all-cause mortality compared to those whose cancers were found in non-bypassed stomachs.
Putting the Numbers in Perspective
While the four-fold increase in risk sounds alarming, medical experts urge patients not to panic. The absolute risk remains remarkably low. Out of more than 109,000 patients, only 46 cases of this specific cancer were identified across the entire multi-decade follow-up period.
“We have to balance this finding against the massive, proven benefits of bariatric surgery,” says Sarah Holmgren, a clinical nutritionist specializing in metabolic health. “Gastric bypass significantly reduces the risk of heart disease, many other types of cancer, and premature death caused by obesity-related complications. We are talking about a very rare complication vs. very common life-saving benefits.”
Statistical Snapshot:
| Period Post-Surgery | Hazard Ratio (vs. Other Bariatric) | Standardized Incidence Ratio (vs. Gen. Population) |
| 1–9 Years | 1.0 (No increased risk) | 0.9 (Similar to general population) |
| 10–44 Years | 4.0 (Significant increase) | 2.5 (Significant increase) |
The Need for Lifelong Follow-Up
For the millions of people worldwide who have undergone gastric bypass, these findings serve as a reminder that “success” isn’t just about the weight lost in the first two years. It is about lifelong vigilance.
The researchers suggest that the increased risk might be due to changes in the internal environment of the bypassed stomach, such as the reflux of bile or changes in the bacterial microbiome, which could cause chronic inflammation over decades.
What should patients do?
-
Don’t skip check-ups: Even 15 or 20 years post-surgery, maintaining a relationship with a bariatric team is vital.
-
Report new symptoms: Unexplained abdominal pain, persistent nausea, or signs of anemia (fatigue, paleness) should be investigated immediately, even if a standard endoscopy comes back “clear.”
-
Advanced Imaging: If symptoms persist, doctors may need to use specialized techniques, such as “double-balloon enteroscopy” or virtual CT gastrography, to see the bypassed section.
Study Limitations and Counterarguments
The study, while massive in scale, does have limitations. Because it relies on historical registry data, researchers could not account for every individual lifestyle factor, such as smoking or H. pylori infections, which are known precursors to stomach cancer. Furthermore, the wide confidence intervals in the mortality data suggest that while the trend is concerning, more research is needed to definitively link the surgery to poorer survival rates.
Some surgeons also point out that modern surgical techniques and better management of acid reflux might lower these risks for patients undergoing the procedure today compared to those who had surgery 30 or 40 years ago.
Conclusion: A Call for Evolved Guidelines
As bariatric surgery becomes increasingly common, the medical community must adapt its long-term screening guidelines. The “set it and forget it” mentality that sometimes follows successful weight loss must be replaced with a strategy for middle-aged and older bypass alumni.
The Nordic study doesn’t suggest that gastric bypass is unsafe; rather, it shines a light on a specific long-term maintenance requirement. For patients and providers alike, the message is clear: the benefits of surgery are vast, but the price of that success is eternal—and informed—vigilance.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References and Sources
https://www.daijiworld.com/news/newsDisplay?newsID=1307279