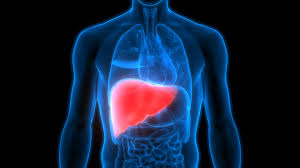
Heavy and prolonged alcohol consumption is a leading cause of liver disease worldwide, inflicting damage that sometimes cannot be fully undone even after quitting. Recent scientific findings shed light on why the liver—the only organ capable of regenerating itself—may lose this vital ability in cases of long-term heavy drinking. Understanding these mechanisms is crucial for public health and may usher in new treatments beyond liver transplantation.
The Liver’s Remarkable Regenerative Power
The liver stands apart in human biology for its capacity to regenerate. After injury or partial removal, healthy liver cells (hepatocytes) typically multiply, restoring tissue mass and function. In mild to moderate alcohol-induced liver injury, this regenerative ability often aids recovery within weeks or months of alcohol cessation. Liver enzyme levels such as AST and ALT, markers of inflammation and damage, tend to normalize within days to weeks after stopping alcohol, signaling healing is underway. Clinical studies show that fatty liver conditions can improve significantly as early as two to three weeks after quitting alcohol, with reductions in liver fat, inflammation, and scarring over ensuing months.
Why Healing Sometimes Fails
However, in cases of alcohol-related hepatitis and advanced cirrhosis, the story changes. Long-term heavy drinking induces extensive scarring (fibrosis) and liver cell damage, severely impairing regeneration. Recent work by researchers at the University of Illinois Urbana-Champaign, Duke University, and Chan Zuckerberg Biohub Chicago reveals a critical biological reason: liver cells become trapped in a dysfunctional “repair limbo.” They partially activate regenerative pathways but fail to mature into fully functioning hepatocytes required for effective tissue regeneration
Professor Auinash Kalsotra explained, “The liver cells attempt to switch into repair mode but get stuck in a half-functioning state—they are neither mature liver cells nor stem-like cells capable of regrowth,” highlighting how inflammation disrupts normal RNA splicing critical to protein synthesis and cell maturation.
Molecular Underpinnings and Implications
Heavy alcohol use triggers inflammation and oxidative stress, which exacerbate liver damage by producing harmful reactive oxygen species. This oxidative stress overwhelms the liver’s antioxidant defenses, worsening cellular injury and promoting formation of toxic protein and lipid adducts that can further impair liver function and stimulate immune responses.
Laboratory studies also show that quitting alcohol restores many metabolic pathways that support liver regeneration. Abstinence reverses fatty liver changes by improving lipid metabolism enzyme regulation, reducing inflammation via downregulating key signaling pathways like Toll-like receptor 4 and MAP kinases, and enhancing antioxidant enzyme activity.
Though partial recovery is common with sustained sobriety, once cells are locked in this dysfunctional repair state, normal regeneration halts, and permanent damage may ensue. This explains why some patients continue to suffer liver failure despite abstinence.
Expert Views
Dr. Meghan Wood, Chief Clinical Officer at Refine Recovery, cautions that while many see normalization of enzyme levels within weeks, “In patients with more severe damage, the timeline is much longer and sometimes the liver can’t fully heal.” She emphasizes that early interventions and continued abstinence are pivotal for better outcomes.
Hepatologist Dr. Anna Mae Diehl, co-lead on the regenerative biology study, stresses, “Understanding why regeneration fails opens new treatment avenues, aiming to ‘unstick’ liver cells from this limbo state and promote healing without transplantation.”
What This Means for Public Health
Alcohol-related liver disease (ARLD) remains a leading cause of liver-related deaths worldwide, accounting for about 3 million deaths annually. The new findings underscore the importance of early detection and prevention, highlighting that while quitting alcohol always benefits liver health, it might not reverse late-stage damage. Public health strategies should emphasize prevention of heavy drinking and early intervention to preserve the liver’s regenerative capacity.
For readers, the take-home message is clear: avoiding excessive alcohol and quitting early can allow the liver to heal substantially. Supporting liver health through a balanced diet, hydration, exercise, and medical follow-up is essential. Those with heavy drinking histories should seek medical advice regularly.
Limitations and Ongoing Research
Most current knowledge comes from animal models and cell studies, with ongoing research needed to translate findings into human therapies fully. Variability in individual genetics, drinking patterns, and coexisting conditions influence outcomes. Moreover, the molecular mechanisms behind “repair limbo” need further exploration to develop targeted drugs that can reactivate liver regeneration.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.