Autoimmune diseases, which currently affect millions worldwide, are chronic conditions where the immune system mistakenly attacks the body’s own tissues. Traditional lifelong treatments largely rely on immunosuppressive drugs intended to reduce inflammation and control symptoms. However, accumulating evidence reveals that these lifelong medications often fall short of providing sustained remission and can pose significant side effects. This landscape is now evolving with exciting new therapies aiming to reset the immune system and offer long-term, if not permanent, relief without continuous drug use.
Key Findings and Developments
Conventional treatments for autoimmune diseases, such as lupus, rheumatoid arthritis, and multiple sclerosis, primarily involve immunosuppressive drugs that control disease activity but do not address the root immunological dysfunction. According to leading experts, these drugs may fail to eradicate disease-causing immune cells, particularly hidden B cells residing deep within the body, limiting their long-term effectiveness. As a result, many patients face lifelong treatment regimens with frequent dosing and risks of adverse effects such as increased infection susceptibility.
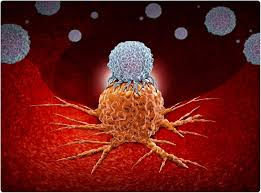
A major breakthrough in recent years has been the development of chimeric antigen receptor (CAR) T-cell therapy, which involves genetically modifying a patient’s immune cells to specifically target and eliminate problematic B cells fueling autoimmune disease. Early clinical studies have demonstrated remarkable outcomes, with patients achieving durable drug-free remission lasting several years after a single CAR-T treatment infusion. One study found remission could last at least four years, with hopes that this could become lifelong. These findings were highlighted in recent presentations at the American College of Rheumatology Convergence 2025, where dual-targeted CAR-T therapies showed promising safety and efficacy in systemic lupus erythematosus (SLE) and other refractory autoimmune diseases.
Expert Perspectives
Dr. Bauer Ventura of the University of Chicago Medicine, who oversees clinical trials of CAR-T for autoimmune diseases, remarked, “Most of their patients have achieved no disease activity or very little disease activity off immunosuppression, which is unheard of in severe systemic autoimmune diseases. These early results could be revolutionary for autoimmune treatment”.
Dr. Nick Jones from Swansea University emphasizes that targeting immune cell metabolism represents another promising approach. His team identified the ABHD11 protein as a potential drug target to reduce inflammation and prevent autoimmune flare-ups without the broad immunosuppression seen in current therapies. “This research opens up exciting possibilities for safer and more effective treatments,” Jones said.
Background and Context
Autoimmune diseases are complex and heterogeneous, making universal cures elusive. Their management has conventionally relied on broadly immunosuppressive agents such as methotrexate, corticosteroids, and biologics that dampen immune activity but come with risks of serious side effects and often incomplete control over disease progression. The challenge has been to develop treatments that specifically address the immune system’s dysregulation without broadly compromising immune defenses.
Innovative immunotherapy techniques, including CAR-T cell therapy, bispecific antibodies, innovative cytokine targeting, and microbiome-based interventions, have emerged from new mechanistic understanding of immune tolerance and regulation. These therapies aim to precisely recalibrate the immune response, promoting long-lasting disease remission and improved quality of life.
Implications for Public Health and Patients
For patients living with autoimmune disorders, these emerging therapies represent a potential paradigm shift—from managing symptoms lifelong to possibly achieving drug-free remission or “resetting” the immune system. This could reduce treatment burden, improve safety, and lower healthcare costs associated with chronic medication usage and disease complications.
However, access, cost, and safety issues remain hurdles. CAR-T therapy involves complex manufacturing processes, is expensive, and carries risks like cytokine release syndrome and neurotoxicity. Patient-specific immune features may also influence outcomes, necessitating personalized treatment approaches and further research.
Limitations and Counterarguments
While promising, CAR-T and other novel therapies are still in experimental or early clinical stages for most autoimmune diseases. Long-term safety, durability across diverse autoimmune conditions, and potential adverse effects need rigorous evaluation through large randomized trials. Moreover, such treatments may not be suitable for all patients, particularly those with compromised overall health or co-morbidities. It is also important to note that conventional immunosuppressive drugs still play a critical role in managing disease flares and maintaining control for many individuals.
Practical Advice for Readers
Autoimmune disease patients should consult qualified healthcare providers to discuss all available treatment options, including emerging therapies being evaluated in clinical trials. While the prospect of drug-free remission is exciting, current standard treatments remain essential for disease management. Patients should avoid abruptly stopping immunosuppressive medications without medical guidance. Staying informed about new developments and clinical research can empower patients to engage actively in their care decisions.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References