Kashmir, along with Delhi, Chandigarh, and other northern regions, has witnessed an alarming surge in Polycystic Ovary Syndrome (PCOS) cases that exceeds the national average, constituting what experts are calling a “silent tsunami” of this increasingly common endocrine disorder in India. PCOS prevalence in Kashmir is notably high at approximately 35%, significantly surpassing the national average estimated between 10-11% using the Rotterdam diagnostic criteria. This escalating public health concern is attributed to factors like sedentary lifestyles, poor diet, hormonal imbalances, and rising psychological stress exacerbated by unique regional socio-economic and cultural dynamics.
Key Findings and Developments
Recent epidemiological studies show India’s overall PCOS prevalence among reproductive-aged women is around 11.3%, based on systematic reviews applying standardized Rotterdam criteria. However, Kashmir’s rates stand out as exceptionally elevated—with a 2020 cross-sectional study of over 3,300 women from the Kashmir valley reporting a striking 35.3% prevalence. Other northern regions such as Delhi and Chandigarh also report rates more than double the national average, reflecting broader regional disparities. These figures reflect a substantial burden of PCOS that extends well beyond typical global prevalence estimates of 8-13%.
Expert Commentary
Dr. Aadil Bashir, Associate Professor of Social Work at the University of Kashmir and lead author on regional PCOS research, emphasized the complexity of PCOS in Kashmir: “The high prevalence is compounded by lifestyle changes and chronic stress, creating a multifaceted health challenge that affects not only physical but also mental health among women.” He highlighted the frequent co-occurrence of anxiety, depression, and metabolic disorders in women diagnosed with PCOS in the region.
Context and Background
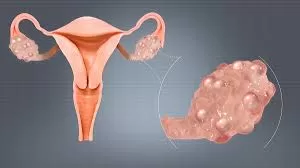
PCOS is a hormonal disorder characterized by irregular menstrual cycles, polycystic ovaries visible on ultrasound, and elevated androgen levels leading to symptoms such as acne, weight gain, and excessive hair growth. Globally, PCOS remains a leading cause of infertility and is associated with increased risks of diabetes, cardiovascular disease, and psychological conditions. India’s unique demographic and lifestyle transitions, including urbanization, sedentary behaviors, and dietary shifts towards obesogenic patterns, have contributed to an increased disease burden, particularly in urban and northern regions.
Implications for Public Health
The high PCOS prevalence in Kashmir and northern India carries widespread implications for reproductive and overall health. Infertility concerns, metabolic complications, and mental health challenges necessitate early diagnosis, public education, and effective management protocols. Despite this, awareness remains low; a Chandigarh study found that 45% of patients diagnosed had minimal understanding of PCOS, and many had to consult multiple doctors or rely on the internet for information. The need for structured healthcare pathways and counseling is urgent.
Practical Implications for Readers
Women experiencing symptoms such as irregular periods, unexplained weight gain, or acne should seek medical evaluation for PCOS. Lifestyle interventions including balanced nutrition, regular physical activity, and stress management are critical parts of managing PCOS symptoms and reducing associated health risks. Early diagnosis and tailored treatment by healthcare professionals can improve quality of life and long-term health outcomes.
Limitations and Counterarguments
The variation in PCOS prevalence across India may partly stem from diagnostic criteria differences—Rotterdam criteria tend to produce higher prevalence estimates by including milder cases. Furthermore, some regional studies rely on convenience sampling, which may skew data. Comprehensive, nationally representative studies are still needed to better quantify PCOS’s full impact and to guide resource allocation.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References