In a pioneering advance for bone health, a research team from Osaka Metropolitan University in Japan has successfully used stem cells extracted from fat tissue to regenerate bone in animal models with spinal fractures—a finding that could signal new hope for patients suffering from osteoporosis-related injuries.
Key Findings and Developments
The Japanese team, led by Yuta Sawada and Dr. Shinji Takahashi from the university’s Graduate School of Medicine, treated rats with vertebral fractures (analogous to common osteoporotic fractures in humans) using adipose-derived stem cells (ADSCs) developed into three-dimensional bone-forming spheroids. These spheroids were combined with beta-tricalcium phosphate (β-TCP), a synthetic material widely used for bone reconstruction, providing a scaffold to support new bone growth.
After transplantation, rats exhibited both significant bone regeneration and increased bone strength. Genetic analyses revealed activation of bone formation pathways. According to Dr. Takahashi, “Since the cells are obtained from fat, there is little burden on the body, ensuring patient safety. This simple and effective method can treat even difficult fractures and may accelerate healing.”
Context and Background
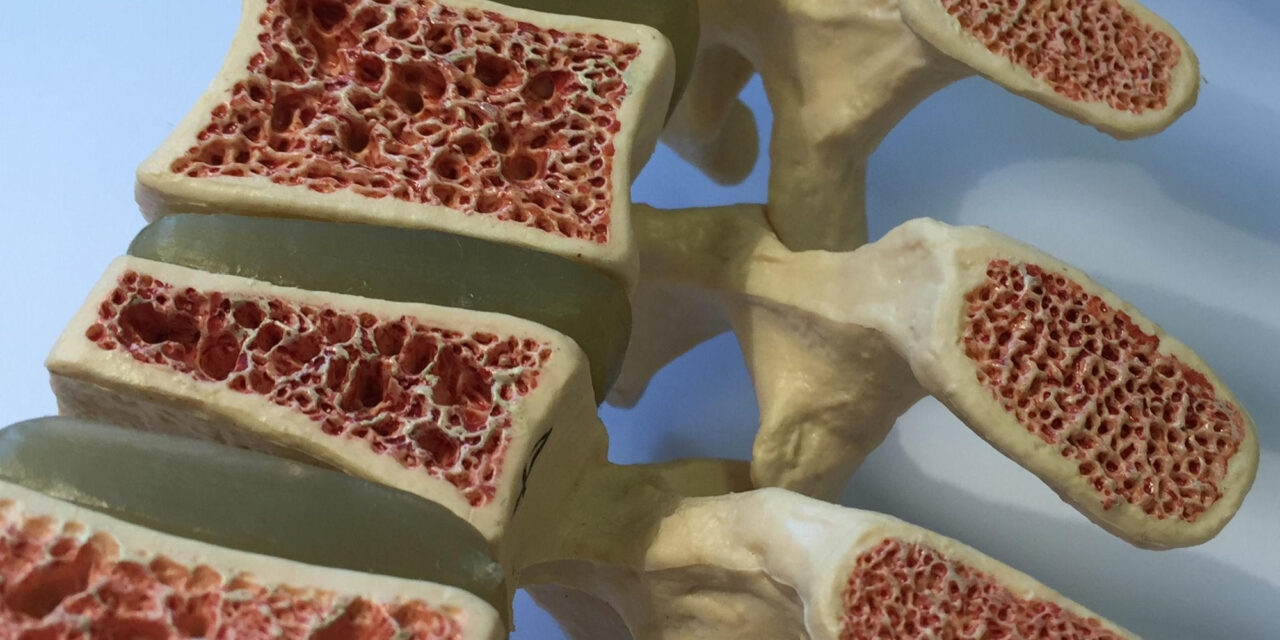
Osteoporosis, characterized by brittle and fragile bones, is a leading cause of spinal compression fractures—termed osteoporotic vertebral fractures (OVFs)—in older adults. These injuries are associated with persistent pain, loss of mobility, and a marked decline in quality of life, sometimes requiring long-term care. Current treatments range from pain management and bracing to vertebroplasty, surgical augmentation, and, in some cases, bone-stimulating medications such as teriparatide.
Stem cells are valued in regenerative medicine for their multipotency—the capacity to develop into various tissue types. ADSCs, specifically, are considered easier to harvest than bone marrow stem cells, especially in elderly patients, with research showing their capability to differentiate into bone-forming cells and improve tissue regeneration when used with biomaterial scaffolds.
Beta-tricalcium phosphate, meanwhile, is an established synthetic graft material that supports bone healing, degrades safely over time, and promotes the growth of new, healthy bone tissue. Its clinical use is often associated with fewer complications than traditional autografts, where bone is harvested from the patient’s own body.
Expert Perspectives
Commenting on the Japanese study, Dr. Maria Barba, a stem cell therapy expert not involved in the research, notes, “Adipose-derived stem cell therapies offer a feasible clinical translation pathway due to accessibility and lower morbidity compared to bone marrow stem cells. Early animal data are promising, but robust clinical trials are needed to prove safety and efficacy in humans.”
Dr. Prashant Hernigou, an orthopedics professor, adds, “Beta-tricalcium phosphate is well-established for bone reconstruction and its combination with viable stem cells could facilitate better and safer bone regeneration, potentially changing the standard of care for complex fractures.”
Implications for Public Health
Should these findings translate to human applications, regenerative stem cell therapies could reduce long-term disability and healthcare costs associated with osteoporosis. The minimally invasive nature of ADSC harvesting is particularly significant for elderly populations, who often face surgical risks.
For patients, this research suggests a future where difficult spinal fractures could be treated more efficiently, restoring mobility and independence. It also aligns with global public health goals to extend healthy lifespan and reduce the burden of chronic bone diseases.
Limitations and Counterarguments
While results in animal models are compelling, major challenges remain before such stem cell therapies can be adopted in routine clinical care:
-
Human trials: Rigorous, peer-reviewed clinical studies are needed to determine safety, dosing, and long-term outcomes in humans.
-
Regulatory hurdles: Stem cell therapies face strict regulatory scrutiny due to variability in cell quality, potential for unintended cell growth, and immune reactions.
-
Scalability: The process must be simplified for efficient, consistent production at a clinical scale.
-
Cost and accessibility: The financial and technical demands may limit widespread adoption initially, especially in lower-resource settings.
Additionally, some experts highlight immune compatibility and potential variation in cell potency depending on donor factors or underlying health conditions. Conservative treatments may still be best for many patients until these approaches are validated and approved for broader use.
Practical Takeaways
For readers, it’s important to recognize the excitement and limitations of this research:
-
This development does not change current standard-of-care practices for osteoporosis or spinal fractures at this time.
-
Healthy bone and muscle maintenance still depend on nutrition, regular exercise, fall prevention, and timely management of bone health as guided by established medical recommendations.
-
Stem cell therapies for bone regeneration remain investigational and are not widely available; patients should consult only qualified healthcare professionals before considering any advanced regenerative treatment.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.