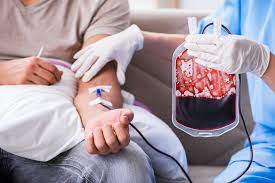
Nara, Japan – In a development that could revolutionize emergency medicine and blood transfusions worldwide, a team of Japanese scientists has created a form of artificial blood compatible with all blood types. The innovation, led by Dr. Hiromi Sakai at Nara Medical University, could address chronic shortages and logistical challenges in blood supply, especially in disaster zones and regions with limited medical resources.
How the Artificial Blood Works
The artificial blood is produced by extracting hemoglobin—the protein responsible for transporting oxygen in red blood cells—from expired donor blood. This hemoglobin is then encapsulated in a protective lipid shell, forming what are known as hemoglobin vesicles. These artificial red blood cells can deliver oxygen throughout the body just like natural blood cells.
Crucially, these vesicles lack the blood type markers that require careful matching in traditional transfusions. This means the artificial blood can be administered to anyone, regardless of their blood type, potentially reducing the demand for O-negative blood, the universal donor type.
Advantages Over Traditional Blood Donations
-
Extended Shelf Life: The artificial blood can last up to two years at room temperature and five years when refrigerated, compared to the 42-day shelf life of donated blood.
-
Universal Compatibility: No blood type matching is required, simplifying logistics in emergencies.
-
Reduced Risk: The process could decrease risks of infection, immunological reactions, and blood type mismatches.
-
Resource Efficiency: It offers a promising solution for areas with limited access to blood donations or where stockpiling is critical.
Progress and Trials
After initial promising results in animal studies, early-stage human trials began in 2022. In the latest clinical trial launched in March, 16 healthy volunteers received 100 to 400 milliliters of the artificial blood. No side effects have been reported so far, paving the way for further studies on its efficacy and safety.
Despite the promise, some experts caution that reliance on expired human blood for hemoglobin may limit large-scale production, and more research is needed before the technology becomes widely available.
Other Approaches
Meanwhile, Professor Teruyuki Komatsu at Chuo University is pursuing a different method, enclosing hemoglobin in a protein called albumin. This approach has also shown encouraging results in animal experiments, particularly in stabilizing blood pressure during hemorrhages and treating strokes.
Looking Ahead
If ongoing trials continue to yield positive results, Dr. Sakai’s team hopes their artificial blood could enter clinical use by 2030. Such a breakthrough could transform emergency medicine, surgery, and disaster response, potentially saving countless lives.
Disclaimer:
This article is based on current research and early-stage clinical trials as reported by My Modern Met and other sources. The artificial blood described is not yet approved for widespread clinical use. Further research, regulatory review, and large-scale trials are necessary before it becomes available to the public. For more details, visit the original article at My Modern Met.