Mumbai, June 9, 2025 — Anushka’s story is one of grit and survival. Once a vibrant college student, her life was derailed by a relentless cough that led to a diagnosis of extensively drug-resistant tuberculosis (XDR-TB). For four years, she endured toxic treatments and hospital visits, only finding hope through a last-resort regimen at a Médecins Sans Frontières (MSF) clinic in Mumbai. Her eventual recovery is a rare triumph in a country still struggling to contain one of its oldest public health crises.
A Heavy Burden
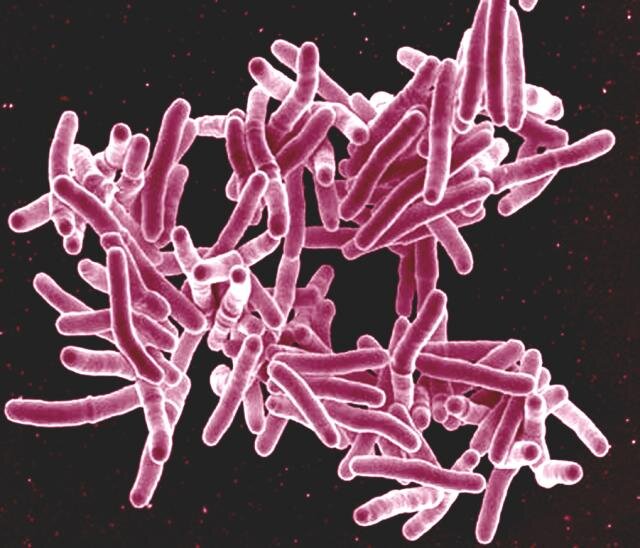
India continues to shoulder the world’s largest tuberculosis (TB) burden, accounting for 26% of global cases in 2023, according to the World Health Organization (WHO). Despite national programmes and ambitious targets, the fight is far from over. The government’s 2025 goal—an 80% reduction in TB incidence and a 90% reduction in deaths compared to 2015—remains elusive. Experts warn that underreporting and under-diagnosis, particularly in rural areas, are masking the true scale of the problem.
“India bears the highest burden of XDR-TB globally, with an estimated 110,000 new cases annually,” says Professor Anil Koul of the London School of Hygiene and Tropical Medicine. Drug-resistant TB strains, like the one Anushka battled, are particularly challenging, requiring complex and costly treatments.
Innovations and Gaps
Efforts to improve detection and treatment are underway. The government’s 100-day TB Elimination Challenge, launched in December 2024, aims to boost diagnosis and treatment at the grassroots level. Digital platforms like Ni-kshay are improving case notification and treatment monitoring.
Diagnostic innovations, such as the Truenat molecular testing platform developed by Goa-based Molbio Diagnostics, have expanded access to rapid TB testing. However, only 2.1% of the National Tuberculosis Elimination Programme budget was spent on diagnostics until 2023-24, and some globally recommended tests remain unavailable in India due to regulatory and supply hurdles.
Treatment regimens are also evolving. The introduction of the BPaLM regimen—a six-month, all-oral combination—has been a game-changer for drug-resistant TB, with a 90% success rate in clinical trials. Yet, access remains limited, with only 1,700 patients in India having received the regimen so far. Concerns about drug resistance and the need for advanced susceptibility testing further complicate widespread adoption.
The Road Ahead
While the domestic budget for the national TB programme has increased fivefold in the past decade, according to the Ministry of Health and Family Welfare, TB still receives a fraction of overall health funding. Experts highlight the need for greater investment in diagnostics, nutrition, and newer treatment options. Studies suggest that improving household nutrition alone could prevent nearly 5% of TB deaths by 2035.
Pricing and procurement challenges persist, especially for the most advanced drugs. Many patients, like Anushka, rely on humanitarian organisations for access to life-saving treatments that would otherwise be unaffordable.
Conclusion
India’s battle against TB is marked by both progress and persistent challenges. Success stories like Anushka’s are inspiring but remain the exception rather than the rule. To truly bend the curve, experts say, the country must invest more in diagnostics, ensure equitable access to new treatments, address underreporting, and tackle the socioeconomic factors that fuel the epidemic.
As Anushka herself says, “Even in that condition, I completed my graduation and kept chasing my dreams.” India’s TB response must now rise to match the resilience of its people—with urgency, equity, and compassion.
Disclaimer:
This article is based on information reported by The Economic Times HealthWorld and other publicly available sources as of June 2025. It is intended for informational purposes only and should not be considered medical advice. For diagnosis, treatment, or medical guidance, please consult a qualified healthcare professional.