February 14, 2026
NEW DELHI — India’s medical device sector is undergoing a seismic shift as the central government’s multi-pronged strategy—comprising the Production Linked Incentive (PLI) Scheme, specialized Medical Device Parks, and massive investment in high-tech human capital—begins to deliver tangible results. As of early 2026, the nation has moved from assembling basic consumables to manufacturing high-end diagnostic and life-support equipment, including MRI machines and linear accelerators, once almost entirely sourced from overseas. This transition marks a critical milestone in the “AtmaNirbhar Bharat” (Self-Reliant India) mission, aiming to transform the country into a global MedTech powerhouse while making life-saving technology more affordable for its 1.4 billion citizens.
The PLI Impact: Breaking the Import Ceiling
For decades, India relied on imports for nearly 80% of its medical device needs, particularly for complex, high-end electronics. The Production Linked Incentive (PLI) Scheme for Medical Devices, with a budgetary outlay of ₹3,420 crore, was designed to break this cycle.
According to the latest data from the Department of Pharmaceuticals, the scheme has already catalyzed significant industrial movement. As of September 2025, 22 greenfield projects have been commissioned, and production has commenced for 55 distinct high-end products. These are not just bandages and syringes; they include:
-
Radiology & Imaging: MRI machines, CT scanners, Mammograms, and PET detectors.
-
Cancer Care: Linear Accelerators (LINAC) and Rotational Cobalt machines.
-
Critical Care: Advanced ventilators, anesthesia workstations, and dialysis machines.
-
Implants: Heart valves, stents, and specialized orthopedic implants.
The economic footprint is equally impressive. Cumulative sales under the scheme have reached ₹12,344 crore, including nearly ₹5,870 crore in exports, proving that “Made in India” devices are meeting stringent international quality standards.
“Plug-and-Play” Innovation: The Rise of Medical Device Parks
To further lower the barriers to entry for manufacturers, the government has sanctioned dedicated Medical Device Parks in Uttar Pradesh, Madhya Pradesh, Tamil Nadu, and Himachal Pradesh. These parks offer a “plug-and-play” ecosystem, significantly reducing the initial capital expenditure (CAPEX) for companies.
“The shared infrastructure model is a game-changer,” says Rajiv Nath, Forum Coordinator for the Association of Indian Medical Device Industry (AiMeD). “By providing common facilities for sterilization, 3D printing, and biocompatibility testing, these parks eliminate the need for every small unit to invest millions in under-utilized labs. It brings down the per-unit cost of manufacturing by 25-30%.”
In Tamil Nadu and Uttar Pradesh alone, over 190 manufacturers have already been allotted land, with many units already moving into the construction phase. These hubs are designed to house everything from electromagnetic compatibility (EMC) centers to gamma radiation facilities, ensuring that a product can go from prototype to validated medical grade within a single campus.
Bridging the Talent Gap: Training 750 High-Tech Professionals
A robust manufacturing sector requires more than just machines; it needs a specialized workforce. Under the Capacity Building and Skill Development sub-scheme, the government has partnered with 12 premier institutions, including various IITs and the National Institutes of Pharmaceutical Education and Research (NIPER).
The goal is ambitious: to produce 750 high-tech professionals over a three-year window. These individuals are trained in industry-aligned curricula that cover medical device design, diagnostics, and advanced production techniques.
“We are shifting the focus from pharmacy to a multidisciplinary MedTech approach,” noted Prof. Shailendra Saraf, Director of NIPER Ahmedabad, during the institute’s recent convocation. NIPER Ahmedabad now hosts a Centre of Excellence (CoE) in Medical Devices, supported by a ₹110 crore outlay. This center serves as a bridge between academic research and industrial application, ensuring that local innovations don’t just stay in the lab but reach the hospital floor.
Public Health Implications: Affordability and Access
For the average patient, these policy shifts translate into one major benefit: affordability. Indigenously manufactured devices are currently priced 10% to 30% lower than their imported counterparts.
In a country where out-of-pocket healthcare expenses can push families into poverty, the localization of dialysis machines, oxygen concentrators, and cardiac stents is a vital public health intervention. Furthermore, the Promotion of Research in Pharma-Medtech Sector (PRIP) scheme, which recently received over 710 research project applications, is now funding the development of AI-driven diagnostics and wearable health monitors tailored for Indian physiological data.
Challenges and the Road Ahead
Despite the optimism, experts caution that the road to total self-reliance has hurdles. A recent report by Rubix Data Sciences suggests that while India is a leader in low-to-mid-tech consumables (accounting for 47% of exports), it still relies on imports for nearly 60% of electro-medical equipment.
“The PLI scheme has been a catalyst, but it isn’t a silver bullet,” warns Pavan Choudary, Chairman of the Medical Technology Association of India (MTaI). “We still face an inverted duty structure where raw materials are sometimes taxed higher than finished goods. To sustain this momentum, we need to deepen component-level manufacturing—making the sensors and microchips here, not just the outer casing.”
Additionally, while India’s regulatory body (CDSCO) has introduced online portals for risk classification, achieving global reciprocity with the US FDA or European CE marking remains essential for Indian manufacturers to capture a larger slice of the $500 billion global market.
High-end medical devices being manufactured in India under the PLI Scheme
1.Rotational Cobalt Machine
2.Linear Accelerator (LINAC)
3.Laser Ablation System
4.CT Scan
5.MRI
6.MRI Coils
7.Mammography
8.X-ray equipment
9.X- Ray including Fixed Line Frequency (LF) and High Frequency (HF) X-Ray Product
10.C-arm/ Surgical X-Ray C-Arm
11.Cath-Lab
12.PET Detector
13.Digital X-Ray Flat Pannel Detector
14.X – Ray Panels
15.Anesthesia Workstation
16.Anesthesia Unit Ventilators
17.Dialyzer
18.Dialysis Machine
19.Haemodialysis Catheter
20.Peritoneal Dialysis Kits
21.Oxygen Concentrators
22.High Flow Oxygen Devices
23.Intensive Care Ventilators
24.Emergency Ventilators
25.ECG
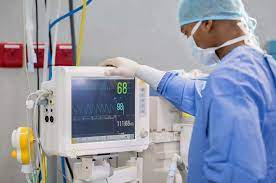
26.Patient Monitoring System / Patient Monitors
27.Multi-Parameter Monitor
28.Defibrillators / Automated External Defibrillators (AED
29.Bi-Phasic Defibrillators
30.Stress Test System
31.Hip Implants
32.Knee implants
33.Trauma Implants
34.PTCA Balloon Dilation Catheter / PTCA Balloon Catheter/Drug Eluting Balloons
35.Heart Valves
36.Stents/Drug Eluting Stents
37.Intravascular Lithotripsy Catheter System
38.Endocutter
Conclusion
As India eyes a $50 billion medical device market by 2030, the current expansion represents more than just economic growth. It is the construction of a resilient healthcare spine. For the healthcare provider, it means faster access to equipment and service; for the patient, it means a more affordable path to recovery.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Press Information Bureau (PIB): “Medical Devices Industries in the country – Year End Review 2025,” (Release ID: 2199433).