NEW DELHI — In a decisive move toward transforming women’s healthcare, the Indian government has announced an ambitious national strategy to eliminate cervical cancer, centering on a dual-force approach: nationwide Human Papillomavirus (HPV) vaccination and the transition to advanced DNA-based screening.
The announcement came during India’s first national summit on cervical cancer elimination, organized by the All India Institute of Medical Sciences (AIIMS) on January 17, 2026. Health officials and NITI Aayog members gathered to issue a “National Call to Action,” signaling a shift from traditional, often less accurate testing methods to high-performance diagnostics and primary prevention.
The Scale of the Challenge
Cervical cancer remains the second most common cancer among women in India, accounting for nearly one-quarter of the world’s cervical cancer deaths. According to the World Health Organization (WHO), India sees approximately 123,000 new cases and 77,000 deaths annually. Unlike many other cancers, however, cervical cancer is almost entirely preventable.
“Cervical cancer elimination is an achievable goal for India,” stated Aradhana Patnaik, Additional Secretary and Managing Director of the National Health Mission (NHM). “We are fully committed to accelerating action across prevention, screening, and treatment.”
The Two-Pronged Strategy: Vaccination and DNA Testing
The government’s roadmap rests on two scientific pillars: the HPV vaccine and HPV DNA testing.
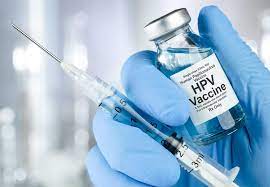
1. HPV Vaccination: The Shield
The Human Papillomavirus (HPV) is a common virus transmitted through skin-to-skin contact. While most infections clear on their own, persistent infection with high-risk strains can lead to cervical cancer.
The government intends to scale up the HPV vaccination program, primarily targeting girls aged 9 to 14. This age group is critical because the vaccine is most effective when administered before exposure to the virus. By preventing the infection at its source, the vaccine can reduce the incidence of cervical cancer by over 90%.
2. DNA-Based Screening: The Detection
For decades, India has relied on the Pap smear or Visual Inspection with Acetic Acid (VIA). While these methods have saved lives, they are often prone to human error and require frequent clinic visits.
The Ministry of Health is now prioritizing HPV DNA testing. Unlike a Pap smear, which looks for abnormal cells, a DNA test looks for the virus itself. This method is significantly more sensitive and can detect the risk of cancer years before any cellular changes occur.
“We must initiate pilot projects that demonstrate how HPV DNA-based screening and self-sampling can be implemented on scale,” said Prof. Dr. V.K. Paul, Member (Health) at NITI Aayog. He emphasized that these technologies would allow women to collect their own samples—a breakthrough for privacy and access in rural areas.
Building a “Hub-and-Spoke” Care Model
One of the primary hurdles in India’s healthcare system is the “loss to follow-up”—when a woman tests positive but does not receive the necessary treatment due to distance or cost.
To combat this, the AIIMS summit focused on a hub-and-spoke model. Under this system:
-
The Spoke: Local primary health centers provide screening and vaccination.
-
The Hub: Regional cancer centers or tertiary hospitals handle complex diagnoses and advanced treatments like surgery, radiation, and chemotherapy.
This ensures that a woman diagnosed in a remote village is seamlessly “linked” to a specialist center, closing the gap between detection and cure.
Expert Insights: Breaking the Silos
Medical professionals at the summit emphasized that technology alone is not enough; a change in the healthcare delivery culture is required.
“Cervical cancer can no longer be addressed in silos,” noted Dr. Abhishek Shankar, Assistant Professor at the Department of Radiation Oncology, AIIMS. “Convening government, clinicians, innovators, and patient advocates is key to creating the momentum and accountability needed.”
Outside experts, not involved in the government’s immediate summit, agree that the move to DNA testing is a game-changer but warn of the logistical climb. “Transitioning to DNA testing is scientifically superior, but we must ensure the lab infrastructure and cold-chain logistics are robust enough to handle millions of samples from across the country,” says Dr. Preeti Vyas, an independent oncology researcher (not affiliated with the AIIMS summit).
What This Means for You
For the average citizen, the government’s commitment suggests several immediate practical implications:
-
Vaccination: Parents of young girls should consult their pediatricians about the HPV vaccine, which is increasingly being integrated into school-based health programs.
-
Modern Screening: Women aged 30 to 65 should ask their healthcare providers about the availability of HPV DNA testing, which may only be required every 5 to 10 years, compared to more frequent Pap smears.
-
Self-Sampling: In the near future, women may be able to perform their own screening at home or in a private booth at a local clinic, removing the need for a pelvic exam for initial screening.
Addressing the Limitations
Despite the optimism, challenges remain. The cost of HPV DNA tests is currently higher than traditional methods, and vaccine hesitancy—fueled by misinformation—can hinder uptake. Furthermore, while the vaccine protects against the most common high-risk strains, it does not cover all of them, meaning screened women must still undergo regular testing.
Key Statistics at a Glance
| Metric | Statistic |
| Annual New Cases (India) | ~123,907 |
| Annual Deaths (India) | ~77,348 |
| Primary Cause | Human Papillomavirus (HPV) |
| WHO Target (by 2030) | 90% vaccinated, 70% screened, 90% treated |
| Effectiveness of HPV Vaccine | >90% reduction in cervical cancer risk |
References
- https://tennews.in/hpv-vaccination-dna-based-screening-key-to-fight-cervical-cancer-in-india-govt/#:~:text=New%20Delhi%2C%20Jan%2017%20(IANS,the%20Health%20Ministry%20on%20Saturday.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.