Published: March 10, 2026
NEW DELHI — In a move set to redefine the landscape of emergency medicine in India, the Union Government has unveiled a sweeping plan to expand emergency and trauma care capacities across district hospitals by 50%. Announced during a high-level post-budget webinar titled “Sabka Saath Sabka Vikas – Fulfilling Aspirations of People,” the initiative targets the critical “golden hour”—the first 60 minutes following a traumatic injury or medical emergency when prompt treatment is most likely to prevent death. By integrating digital tracking, a specialized medical workforce, and a unified 112 emergency response system, the government aims to shield vulnerable families from the catastrophic out-of-pocket expenses often triggered by sudden medical crises.
A Strategic Shift to the District Level
For decades, high-quality trauma care in India has been largely concentrated in tertiary centers and private metropolitan hospitals. The Union Budget 2026-27, specifically under Para 88, seeks to decentralize this expertise. The government’s proposal to establish dedicated Emergency & Trauma Care Centres in District Hospitals acknowledges a stark reality: emergency cases account for a massive portion of hospital admissions, yet emergency-specific beds currently represent only a fraction of total capacity.
“Strengthening emergency and trauma care at the district level requires a systematic and outcome-oriented approach that goes beyond infrastructure to focus on performance and service delivery,” stated Dr. V.K. Paul, Member (Health), NITI Aayog, who moderated the session. He emphasized that the success of this expansion hinges on monitoring real-time indicators to improve treatment for time-sensitive conditions like road traffic injuries, heart attacks, and strokes.
The Four Pillars of the New Emergency Framework
The webinar, attended by policymakers, clinicians, and state administrators, outlined a multi-dimensional strategy to ensure that the 50% capacity increase translates into saved lives.
1. Unified Response Systems (112 Integration)
A central theme of the discussion was the seamless integration of the 112 Emergency Response Support System (ERSS) with ambulance services and hospital triage. Currently, fragmented communication between police, fire, and medical dispatch can lead to life-threatening delays. The new roadmap calls for an interoperable mechanism where a single call triggers a coordinated chain of survival.
2. Infrastructure Transformation
The plan moves away from the traditional “casualty ward” model toward fully functional Emergency Care Departments. These centers will be equipped with:
-
Triage Areas: To prioritize patients based on the severity of their condition.
-
Resuscitation Bays: For immediate life-saving interventions.
-
Dedicated Diagnostics & OTs: Ensuring that imaging and emergency surgeries occur within the department rather than across the hospital campus.
3. Workforce Development: The Emergency Specialist
The shortage of trained emergency personnel remains a significant hurdle. To address this, the government discussed expanding MD and DNB courses in Emergency Medicine. A key recommendation included the creation of a dedicated Emergency Medical Officer (EMO) cadre, ensuring that doctors in these units are specialists in acute care rather than generalists on rotation.
4. Digital Integration and Trauma Registries
To improve long-term outcomes, the webinar highlighted the development of State Trauma Registries integrated with a National Trauma Registry. By tracking patient outcomes digitally, health authorities can use data-driven planning to optimize ambulance deployment and identify geographic “hotspots” for accidents or specific medical emergencies.
Statistical Context: The Cost of Delay
The urgency of these reforms is backed by sobering data. According to the Ministry of Road Transport and Highways (MoRTH), India reports over 1.5 lakh fatalities annually due to road accidents, many of which are preventable with timely trauma care. Furthermore, a study published in The Lancet suggests that nearly 30% of India’s disease burden could be addressed through improved emergency and secondary care.
For the average citizen, an emergency is not just a health crisis but a financial one. “Emergencies often expose families, particularly the poor and vulnerable, to unexpected health expenditure,” the Budget announcement noted. By providing these services at the district level through government-funded centers, the initiative aims to reduce the reliance on expensive private transport and private facility admissions.
Perspectives from the States
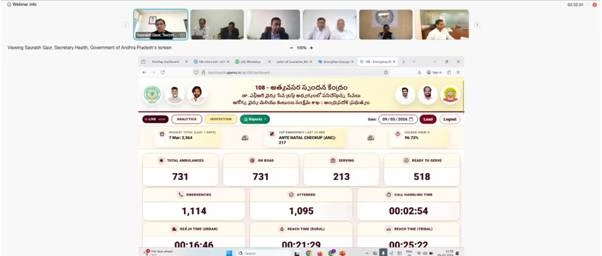
State representatives shared local innovations that could serve as blueprints for the national rollout. Dr. Rajan Khobragade, Additional Chief Secretary of Kerala, and officials from Andhra Pradesh and Tamil Nadu discussed “hub-and-spoke” models for ambulance deployment. These systems use real-time GPS data to ensure the nearest equipped vehicle reaches the patient, reducing response times significantly in rural corridors.
Limitations and Challenges
While the 50% capacity increase is ambitious, experts cautioned that “bricks and mortar” are only half the battle. Dr. Sanjeev Bhoi, Professor of Emergency Medicine at AIIMS New Delhi, noted that maintaining clinical governance and standardized protocols across diverse districts will be essential.
Critics of rapid expansion often point to the “maintenance gap”—where high-tech equipment is procured but remains non-functional due to a lack of specialized technicians or consistent power supply. The webinar addressed this by emphasizing “facility readiness” and the need for a sustainable supply chain for emergency medicine.
What This Means for You
For the health-conscious consumer, these developments signal a shift in how one should approach a medical crisis:
-
Know the Number: Familiarize yourself with 112 as the primary gateway for medical emergencies.
-
Trust Local Districts: As these centers roll out, the local District Hospital may soon offer specialized stabilization that previously required a trip to a distant state capital.
-
The Power of Triage: Patients and families should understand that “Triage” means the most critical cases are seen first, which is a hallmark of an efficient, life-saving system.
The implementation roadmap following this webinar will likely define Indian emergency medicine for the next decade, turning the “Golden Hour” from a concept into a widespread clinical reality.
References
-
Press Information Bureau (PIB): “Post-Budget Webinar: Strengthening of Emergency & Trauma Care Centres,” March 9, 2026.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.