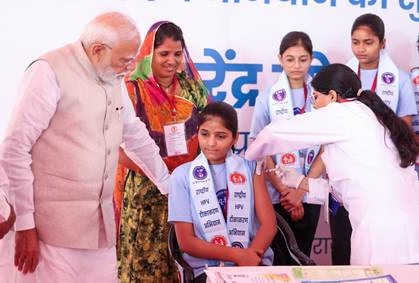
AJMER, RAJASTHAN – In a transformative move for women’s public health, Prime Minister Shri Narendra Modi officially launched India’s nationwide Human Papillomavirus (HPV) vaccination campaign today. Initiated from the historic city of Ajmer, the drive aims to provide free, voluntary, single-dose vaccines to approximately 1.2 crore girls aged 14 across the country.
The campaign represents a sophisticated shift in India’s healthcare strategy, moving from reactive treatment to proactive prevention. By targeting the primary cause of cervical cancer—the second most common cancer among Indian women—the government seeks to eliminate a disease that currently claims nearly 80,000 lives in the country every year.
A Mission for ‘Nari Shakti’
Addressing a diverse gathering of healthcare workers, families, and officials, Prime Minister Modi framed the initiative as a cornerstone of “Nari Shakti” (Women’s Power).
“We all know that when a mother falls ill in the family, the house feels scattered,” the Prime Minister stated. “If the mother is healthy, the family remains capable of facing every crisis. With this sentiment, the government has run many schemes to provide support to women.”
The Prime Minister linked the vaccination drive to a broader ecosystem of women’s health interventions, including the Pradhan Mantri Ujjwala Yojana for clean cooking fuel and the construction of millions of toilets to improve sanitation. He noted that these efforts collectively represent a shift from a “culture of neglect” to one of “care, dignity, and sensitivity.”
The Science: Why Age 14 and Why One Dose?
The decision to focus on 14-year-old girls (those who have completed 14 years but not yet 15) is rooted in clinical efficacy. Medical experts note that the HPV vaccine is most effective when administered before potential exposure to the virus.
The Power of One
While HPV vaccines were traditionally administered in two or three doses, India is adopting a single-dose schedule using the Gardasil-4 (Quadrivalent) vaccine. This alignment follows updated recommendations from the World Health Organization (WHO) and India’s National Technical Advisory Group on Immunization (NTAGI).
Evidence suggests that a single dose provides robust, long-lasting protection, with efficacy rates between 93% and 100% against the HPV types responsible for the majority of cervical cancer cases (specifically types 16 and 18).
“The transition to a single-dose regimen is a game-changer for public health logistics,” says Dr. M. Srinivas, Director of AIIMS New Delhi. “It simplifies the delivery process and ensures higher completion rates while maintaining the high level of immunity required to prevent cellular changes that lead to cancer.”
Understanding the Burden: Cervical Cancer in India
Cervical cancer remains a formidable challenge in India. According to the WHO GLOBOCAN 2022 report, India sees over 120,000 new cases annually. Persistent infection with high-risk HPV strains is the established primary cause.
By introducing the vaccine into the National Immunization Programme, India joins 160 other countries. Notably, 90 of these nations have already successfully transitioned to the single-dose schedule.
Statistical Snapshot:
-
Annual New Cases: ~1,20,000
-
Annual Deaths: ~80,000
-
Target Cohort: 1.2 Crore girls annually
-
Efficacy: 93–100% against vaccine-covered HPV types
Operational Roadmap: How to Get Vaccinated
The campaign will run in a focused “campaign mode” for the first 90 days, after which the vaccine will be integrated into routine immunization schedules.
Key Logistics for Parents:
-
Where: Exclusively at Government Health Facilities (PHCs, District Hospitals, and Medical Colleges).
-
Cost: Free of charge.
-
Consent: Vaccination is strictly voluntary. Digital or physical parental/guardian consent is mandatory.
-
Digital Integration: The U-WIN platform will handle registrations and digital certificates, similar to the Co-WIN system used during the COVID-19 pandemic.
Medical Contraindications
The Union Ministry of Health has issued clear guidelines on when to defer vaccination. It should be avoided or delayed for:
-
Girls with moderate to severe acute illness.
-
Those with a history of severe allergic reactions to previous vaccines.
-
Individuals with known allergies to yeast.
-
Girls outside the specific 14-year-old age bracket.
Expert Perspectives and Public Health Implications
While the launch is being celebrated as a milestone, public health experts emphasize that vaccination is one half of the battle.
“The HPV vaccine is incredibly effective, but it does not replace the need for cervical screenings later in life,” explains a senior oncologist from Lady Hardinge Medical College. “We must continue to promote a dual approach: vaccinate the young and screen the adult population.”
Some independent health advocates have raised questions regarding “herd effect” and the exclusion of boys from the current drive—a strategy used in some Western nations to further limit viral circulation. However, the Indian government’s current focus on 14-year-old girls is a targeted, evidence-based approach designed to protect the group at the highest risk of developing cervical malignancies.
A Healthier Future
The Union Health Ministry is urging parents to utilize this 90-day window. As Union Health Minister Shri Jagat Prakash Nadda noted during his virtual address from Kartavya Bhawan, this is not just a medical intervention, but a “transformative step in India’s preventive healthcare strategy.”
For a nation where cervical cancer has long been a leading cause of premature death among women, this vaccination drive offers a clear path toward a cancer-free future for the next generation.
References
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.