NEW DELHI – In a significant move toward modernizing the nation’s pharmaceutical regulatory landscape, the Union Ministry of Health and Family Welfare (MoHFW) has issued a draft notification to amend the Drugs Rules, 1945. The proposal, announced via Gazette Notification GSR 164(E) on March 9, 2026, seeks to streamline the testing protocols for plasma-derived medicinal products (PDMPs) by removing redundant testing layers that experts say do not add to patient safety but do increase the complexity of production.
The amendment specifically targets Para G of Part XII C in Schedule F, proposing to eliminate the requirement for “double testing”—the practice of testing for viral markers in both the initial plasma pool and the final finished product. By shifting the focus to the “pooled plasma” stage, India aims to harmonize its manufacturing laws with the world’s most stringent pharmacopoeial standards, including those of the United States, Europe, and the United Kingdom.
Understanding the “Double Testing” Dilemma
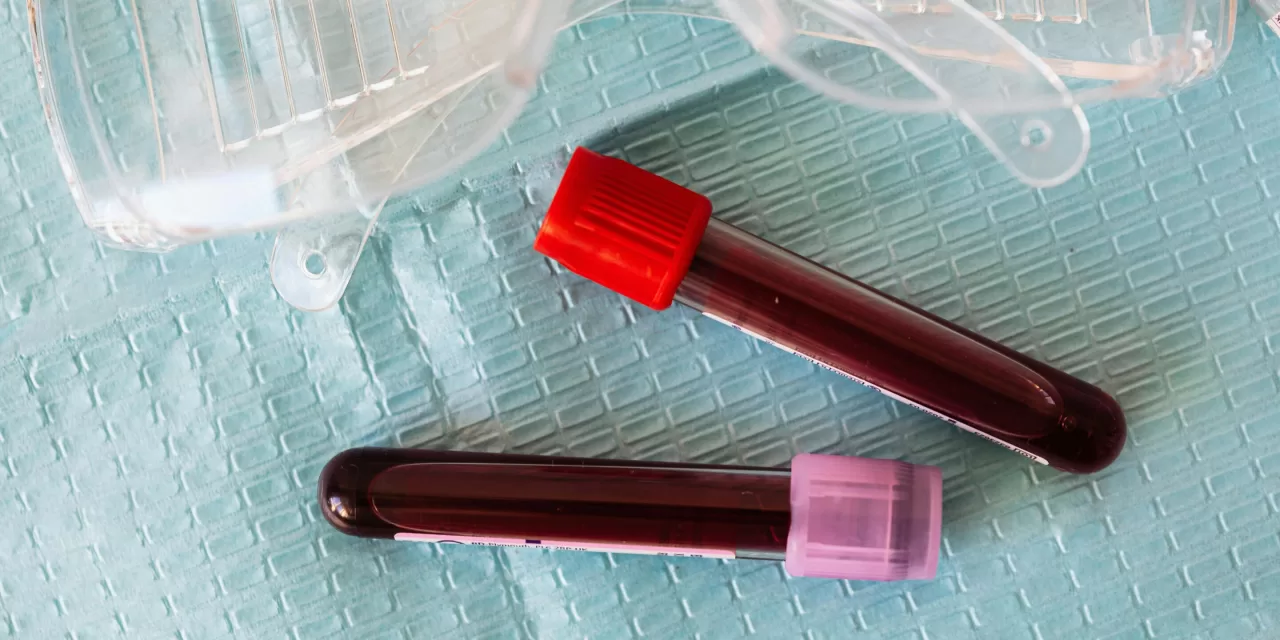
To understand the significance of this change, one must look at how life-saving blood products—such as albumin, immunoglobulins, and clotting factors—are made. These products are derived from human plasma collected from thousands of donors.
Currently, Indian regulations require manufacturers to test for viral markers (specifically Hepatitis B, Hepatitis C, and HIV) at two distinct stages:
-
The Homogeneous Pool: The large collection of plasma before it undergoes “fractionation” (the process of separating plasma into individual proteins).
-
The Finished Product: The final vial of medicine ready for clinical use.
The Ministry’s draft suggests that testing the finished product is scientifically redundant if the starting “pool” has already been certified negative for these viruses using high-sensitivity molecular and serological tools.
“The science of plasma fractionation has evolved to a point where the safety is ‘built-in’ through rigorous screening of the source material and validated viral inactivation steps during manufacturing,” says Dr. Aruna Sharma, a senior consultant in Transfusion Medicine (not involved in the drafting). “Testing the finished product for these specific viral antibodies or antigens often yields no additional safety data because the manufacturing process itself is designed to neutralize these very components.”
The Global Benchmark: Harmonization with the “Big Four”
The MoHFW’s proposal is not an isolated experiment but an effort to align India with the “Big Four” Pharmacopoeias:
-
Indian Pharmacopoeia (IP)
-
British Pharmacopoeia (BP)
-
United States Pharmacopeia (USP)
-
European Pharmacopoeia (EP)
Under these international standards, the “first homogeneous pool” of plasma is the critical control point. It must test negative for the Hepatitis B surface antigen (HBsAg), Hepatitis C virus RNA, and antibodies to HIV. Once a pool is cleared, it moves into a manufacturing environment that includes heat treatment, solvent-detergent cleansing, and nanofiltration—processes that are internationally recognized as more effective at ensuring safety than end-product testing.
Implications for Public Health and Access
For the general public and healthcare providers, this regulatory shift carries several potential benefits:
1. Improved Affordability and Availability
Redundant testing adds significant costs to the manufacturing process. By removing unnecessary steps, the “compliance burden” on domestic manufacturers is reduced. In the long term, this could lead to more competitive pricing for essential treatments like Intravenous Immunoglobulin (IVIg), which is used to treat primary immunodeficiency and various autoimmune disorders.
2. Faster Release of Life-Saving Meds
Finished product testing can take days or weeks to process and validate. Streamlining this could reduce the time it takes for a batch of medicine to move from the factory to the hospital bedside, a crucial factor during shortages of blood-derived products.
3. Strengthening Domestic Manufacturing
By adopting global standards, Indian-made blood products become more “export-ready.” Alignment with the USP and EP allows Indian manufacturers to compete more effectively in international markets, potentially bolstering India’s position as a global pharmacy hub.
Addressing Safety Concerns: Is Anything Lost?
Whenever a testing layer is removed, the immediate question from patient advocacy groups is: Does this make the product less safe?
According to the Ministry and independent virologists, the answer is grounded in the “Multi-Barrier” approach. Modern plasma manufacturing does not rely on a single test. Instead, it relies on:
-
Donor Screening: Rigorous physical and history checks of donors.
-
Individual Unit Testing: Testing every single bag of donated blood.
-
Pool Testing: Testing the combined thousands of units.
-
Viral Inactivation: Chemical and thermal processes that destroy any remaining viral particles.
“The finished product stage is often the least effective place to look for viruses,” explains Dr. Rajesh Kumar, a regulatory specialist. “In some cases, the very process of making the medicine—like concentrating antibodies—can interfere with the accuracy of the viral tests on the final vial, leading to ‘false positives’ that waste perfectly good life-saving medicine.”
The Road Ahead: Public Consultation
The government has emphasized that this is a progressive step toward scientific rationalization. However, the amendment is currently in a “draft” stage. The Ministry has invited stakeholders—including pharmaceutical companies, medical associations, patient rights groups, and the general public—to submit comments and suggestions.
This period of public discourse ensures that all perspectives, including those of smaller laboratories and specialized clinics, are considered before the law is finalized.
Summary of Proposed Changes
| Feature | Current Requirement | Proposed Amendment |
| Testing Stage | Pooled Plasma AND Finished Product | Pooled Plasma ONLY |
| Viral Markers | HBsAg, HCV, HIV | HBsAg, HCV RNA, HIV Antibodies |
| Regulatory Goal | Local Compliance | Global Pharmacopoeial Alignment |
| Expected Outcome | Redundant costs/Delayed release | Reduced burden/Faster access |
References
-
Press Information Bureau (PIB): “Ministry Invites Public Comments on Draft Amendment to the Drugs Rules, 1945,” published March 11, 2026.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.