NEW DELHI – In a significant escalation of India’s public health mission, the Union Ministry of Health and Family Welfare has announced a comprehensive intensification of the National Leprosy Eradication Programme (NLEP). This multi-pronged strategy, centered on aggressive case detection and the reduction of social stigma, aims to interrupt the transmission of leprosy in India by 2027—three years ahead of the global Sustainable Development Goal (SDG) target.
The update was provided by Smt. Anupriya Patel, Union Minister of State for Health and Family Welfare, in a written reply to the Rajya Sabha on March 10, 2026. The government’s renewed focus comes as India continues to account for a significant portion of the global leprosy burden, reporting over 100,000 new cases annually.
The Strategy: From Surveillance to Prophylaxis
The government’s plan shifts from passive reporting to active community-based intervention. Central to this effort are the Leprosy Case Detection Campaign (LCDC) and the Focused Leprosy Campaign (FLC).
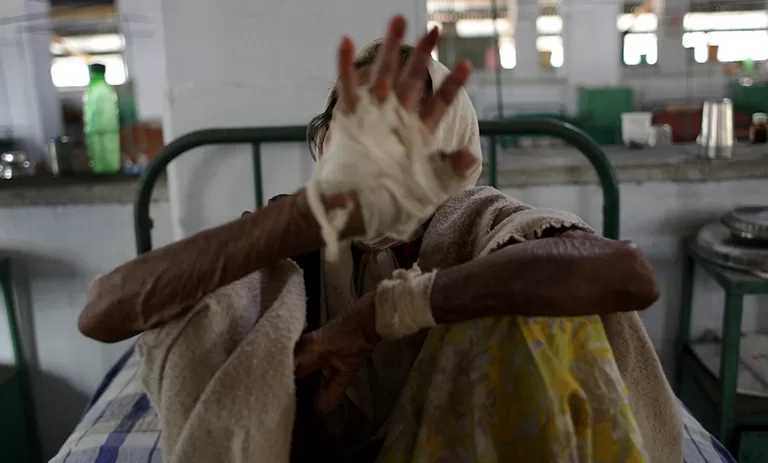
While the LCDC involves house-to-house surveys in high-burden districts, the FLC takes a more surgical approach. When a new case involving Grade 2 Disability (G2D)—visible deformity or severe sensory loss—is detected, health workers immediately screen 300 surrounding households in urban areas or the entire village in rural settings.
“Early detection is the only way to prevent the permanent nerve damage that leads to disability,” explains Dr. Kavita Singh, a public health expert not involved in the government report. “By the time a patient develops a visible deformity (Grade 2), they have often been carrying the bacteria for years. The FLC is critical because it treats the community as the patient, not just the individual.”
Key Pillars of the Enhanced NLEP:
-
ASHA-Based Surveillance: Integration of leprosy screening into the routine activities of Accredited Social Health Activists (ASHAs) in non-LCDC districts.
-
Post-Exposure Prophylaxis (PEP): Administering a single dose of Rifampicin to eligible contacts of newly diagnosed patients. Research indicates this can reduce the risk of contacts developing the disease by up to 57-60%.
-
Digital Integration: Utilizing the Nikusth 2.0 platform for real-time tracking of cases and drug supplies across the country.
Breaking the Silence: The Fight Against Stigma
Perhaps the greatest hurdle in eliminating leprosy is not medical, but social. The Sparsh Leprosy Awareness Campaign (SLAC), launched annually on January 30th (Anti-Leprosy Day), seeks to dismantle the centuries-old stigma that often leads patients to hide their symptoms.
Stigma remains a primary driver of delayed diagnosis. “Many people still fear that leprosy is a curse or is highly contagious through casual contact,” says Rajesh Tiwari, a community health educator. “In reality, it is a mildly infectious bacterial disease that is 100% curable with Multi-Drug Therapy (MDT).”
Under the NLEP, treatment and diagnostic services are provided free of cost through the Ayushman Arogya Mandirs and the broader primary healthcare system. To further support those affected, the government provides a welfare allowance of ₹12,000 for patients undergoing Reconstructive Surgery (RCS).
Statistical Context: Progress and Challenges
Data from the Directorate General of Health Services (DGHS) highlights the scale of the challenge and the progress made:
| Metric | 2014-15 | 2024-25 |
| National Prevalence Rate (per 10,000) | 0.69 | 0.57 |
| New Case Detection Rate (per 100,000) | 9.73 | 7.0 |
| Child Cases (% of new cases) | 9.04% | 4.68% |
| Grade 2 Disability (per million) | 4.68 | 1.88 |
| PEP-SDR Coverage (among contacts) | 71% (2019) | 92% |
While the national prevalence remains below the WHO “elimination” threshold of 1 case per 10,000 people, hyper-endemic pockets persist. Specifically, marginalized communities, including Scheduled Tribes (ST), continue to show a disproportionately high burden, sometimes representing over 18% of new cases despite being 8.6% of the population.
Limitations and the Road Ahead
Despite the aggressive roadmap, experts warn of “stagnant” trends in some regions. The long incubation period of Mycobacterium leprae—which can range from 5 to 20 years—means that cases detected today are often the result of infections that occurred a decade ago.
Critics also point out that while a single dose of Rifampicin (PEP) is effective, its protection may wane over time, necessitating continuous surveillance. Furthermore, the reliance on frontline workers like ASHAs requires constant training to ensure that subtle symptoms, such as pale skin patches with loss of sensation, are not overlooked.
What This Means for the Public
For the average citizen, the message from the Ministry is clear: Leprosy is curable, and the treatment is free. * Check for Symptoms: Look for light-colored or reddish skin patches with a loss of sensation, or numbness in hands and feet.
-
Seek Early Care: Early intervention prevents disability and stops the spread to family members.
-
Support, Don’t Shun: Stigma kills more than the disease itself. Including persons affected by leprosy in community life is essential for national elimination.
The government’s “National Strategic Plan and Roadmap (2023-2027)” represents the final push toward a leprosy-free India. Whether the 2027 goal is met will depend largely on the success of these community-level campaigns and the public’s willingness to step forward without fear.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Government Report: Press Information Bureau (PIB) Delhi. “Update on NLEP.” Posted 10 March 2026. (Release ID: 2237746).