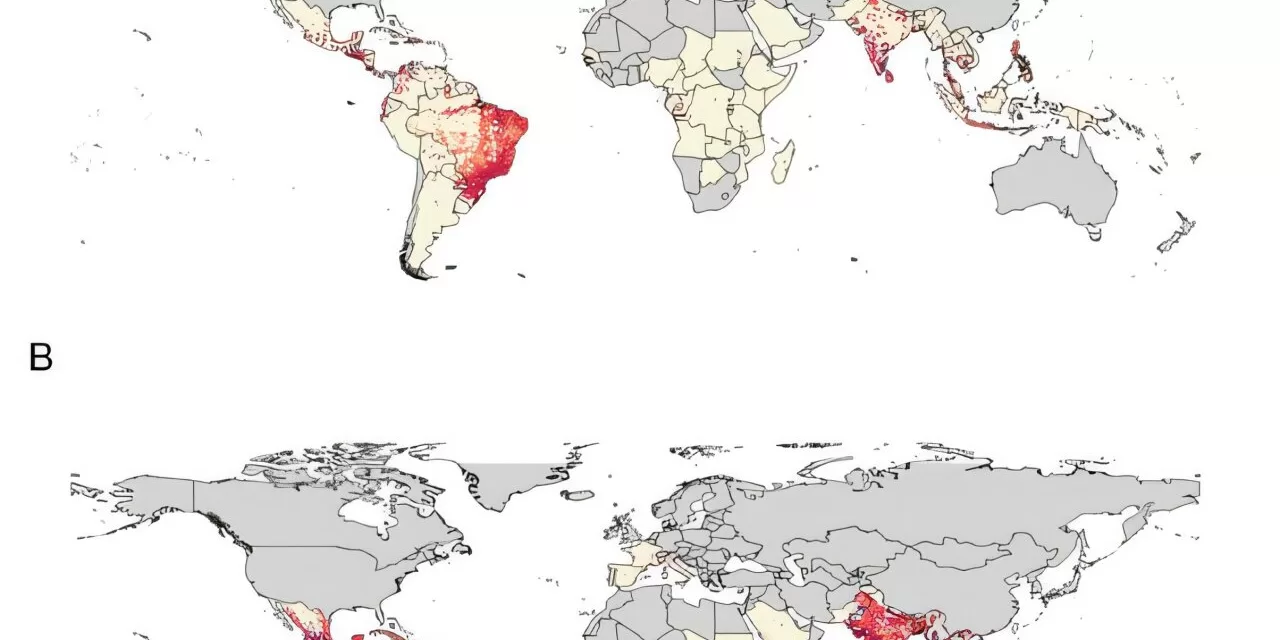
India faces the highest long-term risk from chikungunya, a debilitating mosquito-borne disease, according to groundbreaking new global risk maps published in BMJ Global Health. The research, led by teams at the London School of Hygiene & Tropical Medicine, Nagasaki University, and the International Vaccine Institute in Seoul, estimates that millions of Indians could be affected annually, with chronic disabilities emerging as the greatest concern.
India at the Epicenter of Chikungunya Risk
A comprehensive infectious disease modeling study reveals that 5.1 million people in India are currently at risk of chikungunya infections each year, a figure that could surge to 12.1 million if the virus extends to new regions within the country. Globally, between 14.4 and 34.9 million individuals may be at risk, with India, Brazil, and Indonesia topping the list. Together, India and Brazil account for 48% of the anticipated global impact on health systems and individuals.
Key Findings and Statistical Context
-
Chikungunya is transmitted mainly by Aedes aegypti and Aedes albopictus mosquitoes, common in subtropical and tropical regions. The disease causes high fever (over 39℃) and severe joint pain.
-
New modeling predicts that between 1.2% and 1.3% of people at risk are likely to be infected each year, a lower rate compared to dengue (6%), but still significant for public health.
-
Strikingly, the study highlights a chronic dimension: more than 50% of chikungunya survivors are left with long-term joint pain or disability.
According to Hyolim Kang, the lead researcher from LSHTM and Nagasaki University, “Even the healthiest of people can be infected and left with life-long disability. Prevention of the spread of this disease is important for everyone.”
Expert Commentary and Broader Context
“Chikungunya isn’t confined to tropical zones—even regions long considered safe can become hotspots due to vector expansion and climate shifts,” says Dr. Bhavna Suri, an infectious disease specialist at AIIMS, New Delhi (not involved in the study). Dr. Suri emphasizes the urgent need for surveillance upgrades and community-level interventions tailored to local needs.
Sushant Sahastrabuddhe, Associate Director General at the International Vaccine Institute and co-author of the study, notes, “The potential spread of vectors carrying viruses like chikungunya won’t wait for us to carry out years of research. Real-time sharing of these risk models is critical for public health planning.”
Implications for Public Health and Daily Life
-
India’s health system could see increased demand for supportive services, particularly for chronic pain management and rehabilitation, as no specific antiviral therapies exist for chikungunya.
-
Two vaccines (Ixchiq and Vimkunya) have been licensed for use in Brazil, showing promise for future immunization strategies in India and other high-risk areas.
-
The study supports geographic targeting for vaccine deployment, especially among adults aged 40–60, who are most affected by chronic illness, and young children or seniors, who face the highest risk of severe acute infection.
Dr. Rajesh Kumar, professor of epidemiology at PGIMER Chandigarh (not involved in the research), advises, “For individuals, prevention means minimizing mosquito bites—using nets, repellents, and eliminating stagnant water. For policymakers, it’s a call to invest in vector surveillance and consider new vaccine strategies as part of multi-layered disease control.”
Limitations and Counterpoints
The study’s estimates offer an annual long-term average and do not account for sudden changes due to extreme weather or rapid climate shifts, which may soon alter transmission patterns. While modeling improves upon past outbreaks underreporting, it relies partly on assumptions from related diseases like dengue, which may not entirely match chikungunya’s dynamics. The research also underscores that many regions, especially in Africa, may experience much higher infection rates—up to 11% in Gabon—but longitudinal data remain sparse.
Dr. Suri cautions, “Model-based projections are invaluable, but on-the-ground capacity for timely reporting and integrated vector management is equally crucial. In India’s diverse climate, vigilance must be continuous.”
Practical Guidance and Health Decisions
For the public, the findings underscore the importance of awareness and practical steps to reduce mosquito exposure:
-
Maintain clean surroundings and eliminate standing water
-
Use mosquito repellents and bed nets
-
Seek prompt medical attention for unexplained fever and joint pain
For healthcare professionals, the report suggests updating protocols for chronic pain following arboviral infection, advocating for integrated case surveillance, and promoting the judicious rollout of vaccines where available.
Prevention, early intervention, and robust community engagement remain key as India faces the prospect of bearing the greatest chikungunya burden worldwide.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Kang H, Sahastrabuddhe S, Abbas K, et al. “Global, regional, and national burden of chikungunya: force of infection mapping and spatial modelling study.” BMJ Global Health. 2025. DOI: 10.1136/bmjgh-2024-018598.
- https://medicalxpress.com/news/2025-10-india-biggest-impact-chikungunya.html