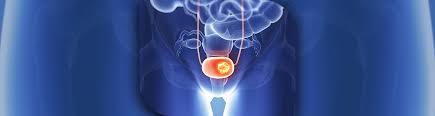
Bladder cancer treatment for high-risk non-muscle invasive bladder cancer (NMIBC) has long relied on intravesical Bacillus Calmette-Guérin (BCG) therapy, a form of immunotherapy that boosts the immune system locally to reduce tumor recurrence. In recent years, adding immune checkpoint inhibitors (ICIs) to BCG has generated excitement as a potential way to improve outcomes. However, evidence presented at the 2025 European Society for Medical Oncology (ESMO) meeting and other recent studies suggest that while some benefit is seen, the combination is not a clear-cut breakthrough and carries increased risks of toxicity.
What is New?
Two pivotal phase 3 trials, POTOMAC and ALBAN, evaluated adding an immune checkpoint inhibitor to standard BCG in patients with high-risk NMIBC. The POTOMAC trial combined durvalumab (Imfinzi) with BCG, while ALBAN tested atezolizumab (Tecentriq) plus BCG. Additionally, the recently published CREST trial paired the investigational PD-1 blocker sasanlimab with BCG.
The results showed some modest improvement in disease-free survival and recurrence reduction, especially in the POTOMAC trial with durvalumab. However, this came at the cost of significantly increased immune-related adverse events, ranging from mild flu-like symptoms to more severe immune toxicities impacting organs. As Dr. Bradley McGregor of Dana-Farber Cancer Institute, the discussant of these studies, noted, “Adding immune checkpoint blockade to BCG is not a slam dunk.” Moreover, there is currently no reliable method to identify which patients would benefit most from these combinations, limiting personalized treatment.
Background and Context
NMIBC accounts for approximately 70% of newly diagnosed bladder cancers, and BCG immunotherapy has been a mainstay for decades. However, 30-40% of patients either fail to respond or experience recurrence, creating a critical need for improved therapies.
Immune checkpoint inhibitors, such as pembrolizumab, durvalumab, atezolizumab, and sasanlimab, block proteins that tumors use to evade immune attack, thus reactivating T cells to target cancer cells. These agents have revolutionized treatment for advanced bladder cancer and are now being tested earlier in the disease course in combination with BCG.
Key Findings
-
The POTOMAC trial demonstrated a statistically significant improvement in disease-free survival with durvalumab plus BCG compared to BCG alone.
-
Both the ALBAN and CREST trials showed trends toward better outcomes but with higher toxicity profiles.
-
The increased immune-related side effects include colitis, hepatitis, pneumonitis, and others that require careful monitoring.
-
No current biomarkers reliably predict patient response to these combination regimens.
-
BCG alone remains effective for many patients with high-risk NMIBC, and its failure rate may be lower than previously assumed.
Expert Opinions
Dr. McGregor highlighted the nuanced benefits and risks, emphasizing the need for better patient selection. Other experts suggest that ongoing trials investigating novel agents, dosing strategies, and additional immunomodulatory drugs may further refine approaches. The landscape is evolving, with efforts to enhance response durability while minimizing adverse events.
Public Health Implications
This evolving treatment paradigm offers hope for bladder cancer patients who have limited bladder-preserving options besides radical surgery. If combinatorial immunotherapy regimens are optimized, they could improve quality of life and survival for many. However, broader application awaits confirmatory trials, longer follow-up, and incorporation of predictive biomarkers to tailor therapy and manage toxicity.
Limitations and Counterarguments
-
Increased toxicity limits the feasibility of combining ICIs with BCG for all patients.
-
Lack of clear predictive biomarkers means exposing many patients to additional risks without guaranteed benefit.
-
The modest clinical improvements require weighing against side effects and cost implications.
-
Some experts recommend continuing BCG monotherapy as standard until more definitive guidance emerges.
Practical Takeaways for Patients
For patients with high-risk NMIBC, current standard treatment remains BCG immunotherapy alone. Those facing BCG failure or recurrence should consult their oncologists about clinical trials involving immune checkpoint inhibitors or other novel therapies. Close monitoring for potential immune-related side effects is essential. Future treatment may become more personalized as research progresses.
Medical Disclaimer:
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.