A recent comprehensive meta-analysis combining data from over two million women reveals that hysterectomy—surgical removal of the uterus—especially when performed alongside bilateral oophorectomy (removal of both ovaries), is associated with a significantly higher risk of stroke. The findings, published in the peer-reviewed journal Menopause, highlight important long-term cardiovascular implications for women undergoing these common gynecologic procedures and call for enhanced stroke risk monitoring and preventive care in this population.
Key Findings and Statistical Context
The meta-analysis drew on the National Health and Nutrition Examination Survey (NHANES) data alongside at least 15 additional cohort studies, encompassing a sample size of approximately 2,065,490 women. It found that hysterectomy alone correlated with a 9% increased risk of stroke (Hazard Ratio [HR]: 1.09, 95% Confidence Interval [CI]: 1.04-1.15). Bilateral oophorectomy was linked to a 13% elevated stroke risk (HR: 1.13, 95% CI: 1.09-1.17). Most notably, hysterectomy combined with bilateral oophorectomy was associated with an 18% higher stroke risk compared to women who did not undergo these surgeries. In separate cohort analyses with longer follow-up, this risk increased further, with one study reporting a 51% increased stroke risk for combined surgery (HR: 1.55; 95% CI: 1.04-2.33).
The elevated stroke risk persisted across various surgical indications, ovarian conservation statuses, and demographic subgroups. Importantly, stroke risk was higher even after accounting for traditional cardiovascular risk factors such as hypertension, age, income, education, and depression severity.
Expert Commentary and Biological Mechanisms
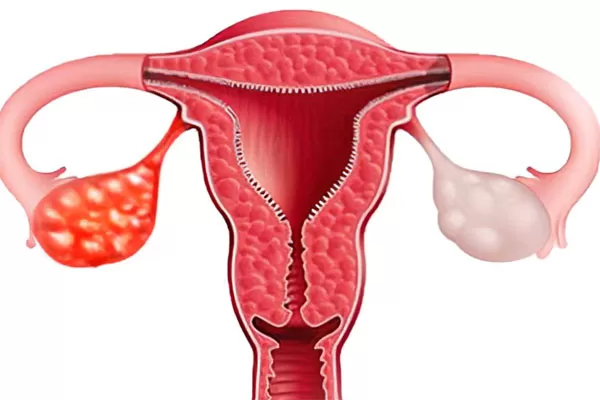
Dr. Stephanie Faubion, Medical Director of The Menopause Society and lead commentator on this research, explained that these surgeries significantly affect estrogen levels—a key hormone protective against stroke. The uterus and ovaries contribute to hormonal balance, and removal of these organs, especially the ovaries, leads to sharp declines in estrogen. This hormonal disruption can lead to earlier menopause and increase vulnerability to cardiovascular diseases including stroke.
Estrogen’s protective effects include maintaining healthy blood vessel function and lipid profiles, reducing inflammation, and influencing blood clotting. A bilateral oophorectomy can reduce serum estradiol by up to 80%, disrupting this protection, while hysterectomy alone may indirectly reduce ovarian hormone production by affecting blood supply to the ovaries. These biological effects provide plausible pathways linking these surgeries with elevated stroke risk.
Context and Background
Stroke is a leading cause of death and disability among women worldwide, and women’s unique cardiovascular risk factors are increasingly recognized. Pre-menopausal women have a lower stroke risk compared to men of similar age, in part due to estrogen’s beneficial vascular effects. However, stroke risk doubles within a decade after natural menopause, as endogenous estrogen declines naturally. Surgical menopause induced by oophorectomy and hysterectomy accelerates this process.
Hysterectomy and oophorectomy are common procedures performed to treat conditions such as uterine fibroids, endometriosis, pelvic pain, and ovarian cysts. Decisions about these surgeries require balancing symptom relief against potential long-term risks.
Public Health Implications
This growing evidence base underscores the need for healthcare providers to carefully evaluate cardiovascular risk before and after hysterectomy and oophorectomy. Women undergoing these procedures should receive counseling about potential risks, including stroke, and be offered risk reduction strategies such as lifestyle modifications, regular cardiovascular screening, blood pressure control, and potentially hormone replacement therapy where appropriate and safe.
In public health terms, awareness campaigns targeted at women and clinicians can improve stroke prevention efforts by highlighting surgery-related risks and promoting early detection. Given the high incidence of these surgeries globally, these interventions could have important impacts on women’s health outcomes.
Limitations and Counterarguments
While the meta-analysis provides robust evidence, some studies report conflicting findings, and further prospective research is needed. Limitations include reliance on observational data, self-reported surgical histories, variance in surgical techniques, and incomplete characterization of stroke types. Some evidence suggests the magnitude of risk may differ by age at surgery and hormone therapy use. Not all hysterectomies or oophorectomies carry equal risks, and unilateral oophorectomy may have different implications than bilateral removal.
Careful interpretation and individualized patient decision-making remain key.
What This Means for Women
Women facing hysterectomy and bilateral oophorectomy should discuss these findings with their healthcare providers to fully understand the benefits and risks. For many women, surgery may be necessary or the best option; however, knowledge of potential stroke risk can guide closer cardiovascular monitoring and adoption of preventive health behaviors. A heart-healthy lifestyle including regular exercise, balanced diet, smoking cessation, and blood pressure management is especially important.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://www.emedinexus.com/post/52496/Study-Links-Hysterectomy-with-Bilateral-Oophorectomy-to-Higher-Stroke-Risk-in-Women