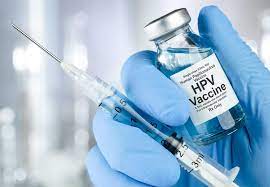
Seventeen years following the introduction of the human papillomavirus (HPV) vaccine, compelling new evidence shows a sustained reduction not only in HPV infections among vaccinated individuals but also significant herd immunity benefits among the unvaccinated population. This long-term analysis affirms the vaccine’s critical role in reducing HPV-related infections and supports continued efforts to maintain and increase vaccination coverage globally.
Key Findings and Developments
A cross-sectional study tracking over 2,300 sexually experienced adolescent girls and young women aged 13 to 26 years from 2006 to 2023 revealed a striking decrease in HPV infections targeted by the vaccine. Vaccination coverage rose from 0% to more than 80% during the study period. Among vaccinated participants, the prevalence of HPV types covered by the bivalent, quadrivalent, and nine-valent vaccines plummeted by 75% to 98%. For example, HPV type positivity for the bivalent vaccine types dropped from 27.7% at the start of the program to just 0.4% after nearly two decades.
Crucially, the study also demonstrated meaningful infection reductions among unvaccinated individuals, indicating strong herd protection. Infections by vaccine-related HPV types declined across the broader community, even among those who had not personally received the vaccine. This herd immunity was particularly noted in populations at higher risk, reinforcing the vaccine’s public health impact beyond direct recipients.
Expert Perspectives
Dr. Alyssa DeSieghardt, lead author of the recent JAMA Pediatrics publication on this topic, explains, “Our findings confirm that HPV vaccination programs yield durable protection for vaccinated individuals while also substantially decreasing infections in the broader community through herd immunity. This dual effect is vital for reducing HPV-related diseases on a population level.” Independent experts corroborate these findings: Dr. Nikhil Patel, infectious disease specialist, highlights that “High vaccination coverage is key to leveraging herd effects, protecting even those who might miss getting vaccinated, and enhancing community health outcomes”.
Additional evidence from countries like Australia and Denmark, which implemented early HPV vaccination programs with high female coverage, supports these outcomes. In Australia, genital wart cases among unvaccinated young men dropped significantly within five years of female-only vaccination campaigns, demonstrating the vaccine’s indirect protective effects.
Context and Background
The HPV vaccine, introduced nearly two decades ago, targets high-risk HPV types responsible for nearly all cervical cancers and a substantial share of other anogenital and oropharyngeal cancers. There are currently three major vaccines available: bivalent, quadrivalent, and nine-valent, each covering progressively more HPV types. The vaccines have undergone rigorous clinical trials and have been incorporated into national immunization programs worldwide.
Mathematical models predicted that herd immunity would develop at vaccination coverages exceeding 50%, with programs targeting both girls and boys potentially eliminating vaccine-type HPV infections at reach of coverage levels around 80%.
Public Health Implications
This evidence underscores the importance of maintaining high HPV vaccination rates to sustain broad community protection. Herd immunity helps reduce transmission in unvaccinated individuals, curtailing HPV spread and lowering the incidence of HPV-attributable cancers and conditions, such as genital warts. Public health messaging can leverage these findings to combat vaccine hesitancy by emphasizing community-wide benefits.
Clinicians should advocate for HPV vaccination among adolescents and young adults, noting that even partial vaccination coverage in a population contributes to overall protection. The findings are reassuring for those vaccinated late or who did not complete the full schedule, as community-level protection reduces their risk indirectly.
Limitations and Counterarguments
While the benefits of HPV vaccination and herd effects are evident, some limitations warrant consideration. Vaccine uptake and herd immunity effects vary by region and population, especially in areas with lower healthcare access or vaccine availability. Additionally, most studies focus on female vaccination programs, with ongoing research assessing the broader impact of gender-neutral vaccination efforts.
Moreover, the duration of immunity, particularly with single-dose versus multi-dose schedules, is still under investigation. Current long-term data suggest protection lasts at least 14-17 years, but continued surveillance is essential.
Practical Takeaways for Readers
Individuals, especially parents of adolescents, should view HPV vaccination as a critical preventive health measure that not only protects the vaccinated person but also contributes to the well-being of the entire community. Routine vaccination before exposure to HPV via sexual activity ensures the greatest benefit. Even for those who may have missed early vaccination, discussing catch-up options with healthcare providers is advisable.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://www.emjreviews.com/general-healthcare/news/hpv-vaccine-shows-strong-herd-effect-17-years-on/