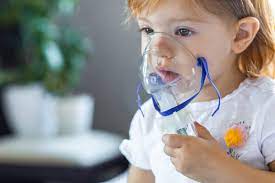
NEW DELHI — In a sobering revelation that underscores the mounting health cost of India’s toxic air, the Union Health Ministry has informed Parliament that Delhi’s central government hospitals alone recorded over 200,000 cases of acute respiratory illness (ARI) between 2022 and 2024. The disclosure comes amidst a deepening public health crisis, with medical experts warning that the surge in hospitalizations is merely the “tip of the iceberg” of a generation suffering from irreversible lung damage.
The Official Disclosure
Responding to a query in the Rajya Sabha on Tuesday, Minister of State for Health Prataprao Jadhav presented data that paints a grim picture of the capital’s health. Six central government hospitals in Delhi—including premier institutions like AIIMS, Safdarjung, and Ram Manohar Lohia Hospital—reported a staggering cumulative load of ARI cases: 67,054 in 2022, rising to 69,293 in 2023, and 68,411 in 2024.
While the raw number of emergency visits has plateaued at a high level, the severity of these cases appears to be worsening. The data indicates that hospital admissions—patients sick enough to require overnight monitoring or intensive care—rose steadily from 9,878 in 2022 to 10,819 in 2024.
“Polluted air is a triggering factor for respiratory ailments and associated diseases,” Minister Jadhav stated, marking a significant, albeit cautious, acknowledgment from the government. However, he stopped short of declaring pollution a direct cause of death, noting that “health effects of air pollution are a synergistic manifestation of factors, which include food habits, occupational habits, socio-economic status, medical history, and immunity.”
Beyond Delhi: A National Crisis
While Delhi remains the epicenter, the data reveals that the crisis is metastasizing to other metros previously considered safer due to their coastal geography.
-
Mumbai: The financial capital witnessed a shocking five-fold increase in ARI hospital admissions at reporting sites, jumping from just 31 in 2023 to 474 in 2024.
-
Chennai: Southern India’s major hub is also seeing a persistent caseload, with over 1,500 emergency respiratory cases reported annually at its sentinel surveillance sites.
The Science: Validating the Link
Strengthening the case for a direct link between the smog and the sick wards, the Indian Council of Medical Research (ICMR) has completed a landmark multi-site study. Analyzing data from 33,213 patients attending emergency rooms across five hospitals, the study found a “strong and consistent” correlation: as pollution levels spiked, so did the number of patients gasping for air in emergency departments.
This data challenges the long-standing bureaucratic defense that the health impacts of pollution are anecdotal or difficult to quantify. “The association is strong and consistent with global findings,” the Ministry noted regarding the ICMR study, though it maintained that the study “cannot formally prove causation.”
Expert Perspectives: “A Visible Burden”
While policymakers navigate the complexities of causation, clinicians on the ground describe a clear and present emergency.
“The health burden of air pollution is no longer abstract; it is visible every day in our emergency rooms,” says Dr. Suranjit Chatterjee, a senior consultant in internal medicine at Indraprastha Apollo Hospitals. He notes that prolonged exposure to PM2.5 (fine particulate matter) is weakening respiratory systems across all age groups, making them susceptible to severe infections that take longer to heal.
Dr. Gopi Chand Khilnani, Chairman of the PSRI Institute of Pulmonary, Critical Care and Sleep Medicine, offers a starker perspective on the changing nature of lung disease in India. “Thirty years ago, 90% of Chronic Obstructive Pulmonary Disease (COPD) cases were smokers. Today, nearly 50% of our COPD patients are non-smokers. Their only fault is breathing,” Dr. Khilnani explains. His advice to patients with chronic conditions is drastic but increasingly common: “If you can afford it, leave Delhi for 6-8 weeks.”
The Pediatric Toll: Sacrificing a Generation
Perhaps the most alarming aspect of the crisis is its impact on children. Dr. Saurabh Khanna, a leading neonatologist, warns that the damage extends beyond temporary coughs. “Children inhale more air relative to their body weight than adults. When they breathe this toxic air, we are seeing cases of reduced lung growth,” he says. “We are essentially capping the potential of an entire generation’s lungs before they even reach adulthood.”
The physiological impact is multifaceted:
-
Inflammation: PM2.5 particles bypass natural defenses, lodging deep in the alveoli and causing persistent inflammation.
-
Neurotoxicity: Emerging evidence suggests these particles can cross the blood-brain barrier, potentially affecting cognitive development in children.
-
Systemic Risk: The pollutants enter the bloodstream, elevating risks for heart attacks and strokes even in younger populations.
Public Health Implications and Recommendations
The government has responded by expanding its surveillance network. The National Centre for Disease Control (NCDC) now operates over 230 sentinel surveillance sites across 30 states and Union Territories to track these illnesses in real-time. However, surveillance is diagnosis, not a cure.
For the general public, the implications are immediate. Health experts recommend a shift in daily routine during high-AQI periods:
-
Timing Matters: Avoid outdoor activities early in the morning or late evening when pollutants are trapped closer to the ground.
-
Protection: Use N95 masks rather than cloth masks, which offer little protection against PM2.5.
-
Indoor Air: Creating a “clean air room” at home with an air purifier, especially for vulnerable family members, is becoming a medical necessity rather than a luxury.
Conclusion
The admission of 2 lakh cases by the government serves as a grim validation of what citizens have felt in their throats and lungs for years. While the official stance remains cautious regarding “direct causation,” the convergence of hospital data, ICMR research, and clinical testimony paints an undeniable picture: India’s air is not just dirty; it is a public health emergency of unprecedented scale. As winter intensifies and AQI levels hover in the ‘severe’ category, the cost of inaction is being paid in hospital admissions and shortened lives.
Medical Disclaimer:
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References:
-
Parliamentary Data: Statement by Minister of State for Health Prataprao Jadhav in Rajya Sabha, responding to Question No. 274 (December 2024). Source: Sansad TV / Ministry of Health & Family Welfare.