May 14, 2025
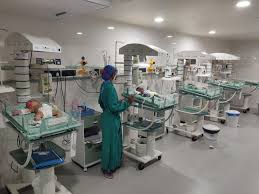
In the high-stakes environment of the Intensive Care Unit (ICU), the focus has traditionally been on stabilizing critically ill patients using evidence-based practices. However, a growing body of research and new guidelines from the Society of Critical Care Medicine are shifting this perspective, emphasizing the vital role that families and primary caregivers play in patient care and recovery.
The Changing Face of ICU Care
Historically, ICU teams have viewed family members as potential obstacles-sources of conflict, stress, and even disruption. A 2009 study found that up to 70% of ICU staff had experienced conflicts with family caregivers, often ranking these disputes among their top workplace stressors.
But recent guidelines, reaffirmed in the Society of Critical Care Medicine’s 2024 Guidelines on Family-Centered Care for Adult ICUs, advocate for a new approach. They recommend that family presence should be the default, not the exception, and encourage family attendance on rounds and participation in bedside care.
Dr. Giora Netzer, vice president and chief experience officer at the University of Maryland Medical System and co–vice chair of the guidelines task force, explains, “Supporting families isn’t just the right thing to do-it leads to better clinical outcomes. When families are involved, patients who survive often have better functional outcomes, and for those who don’t, care can be better matched to their needs, reducing suffering.”
From Roadblock to Ally
Despite the evidence, integrating families into ICU care remains a challenge. Many clinicians are untrained in the “soft skills” of family engagement and have faced emotionally charged conflicts with caregivers. This has led to an ingrained wariness, with some clinicians reflexively viewing families as sources of trouble.
Yet, experts like Kimberly Best, RN, a dispute resolution specialist with decades of ICU experience, argue that reframing families as allies rather than adversaries can transform care. “These are the people who know the patient best-their preferences, their history, their typical responses,” Best says. “When we involve them appropriately, it not only personalizes care but also reduces anxiety for everyone involved.”
Best recalls a case where a family member, initially seen as “difficult,” became an invaluable resource after being invited to participate in daily rounds and contribute observations. The result? Improved communication, greater satisfaction, and better patient outcomes.
Steps Toward Collaboration
Hospitals like the University of Maryland Medical System are institutionalizing policies that elevate caregivers’ roles. Family members are now considered central to the care team, not mere visitors. They’re allowed to stay overnight, participate in care discussions, and even assist with comfort measures or communication logs.
Key strategies for fostering collaboration include:
-
Acknowledging the Family’s Role: Recognizing that families are part of the patient’s personhood, not outsiders.
-
Uncovering Goals of Care Together: Using open-ended questions to align care with the patient’s values and priorities.
-
Assigning Constructive Roles: Giving caregivers specific tasks-like maintaining a communication log or helping with comfort measures-to provide focus and a sense of purpose.
-
Improving Communication: Proactive education and structured family meetings can reduce conflict and enhance collaboration, as shown in research by Dr. Élie Azoulay.
Zac Shepherd, an ICU travel nurse, notes, “ICUs can be dehumanizing, but inviting caregivers to participate reminds everyone that we’re in this together.”
The Payoff
While involving families may require an upfront investment of time and effort, the dividends are significant: more personalized patient care, reduced caregiver anxiety, higher satisfaction, fewer lawsuits, and even improved job satisfaction for healthcare providers.
As hospitals nationwide begin to adopt these family-centered practices, the ICU is evolving from a place of conflict to one of collaboration-where families are not a hindrance, but a help.
Disclaimer:
This article is based on information from Medscape’s “From Hindrance to Help: The Test of ‘My Person’ in the ICU” and summarizes expert opinions and guideline recommendations. It is intended for informational purposes only and should not be taken as medical advice. For specific medical concerns, consult a qualified healthcare professional.
Citations: