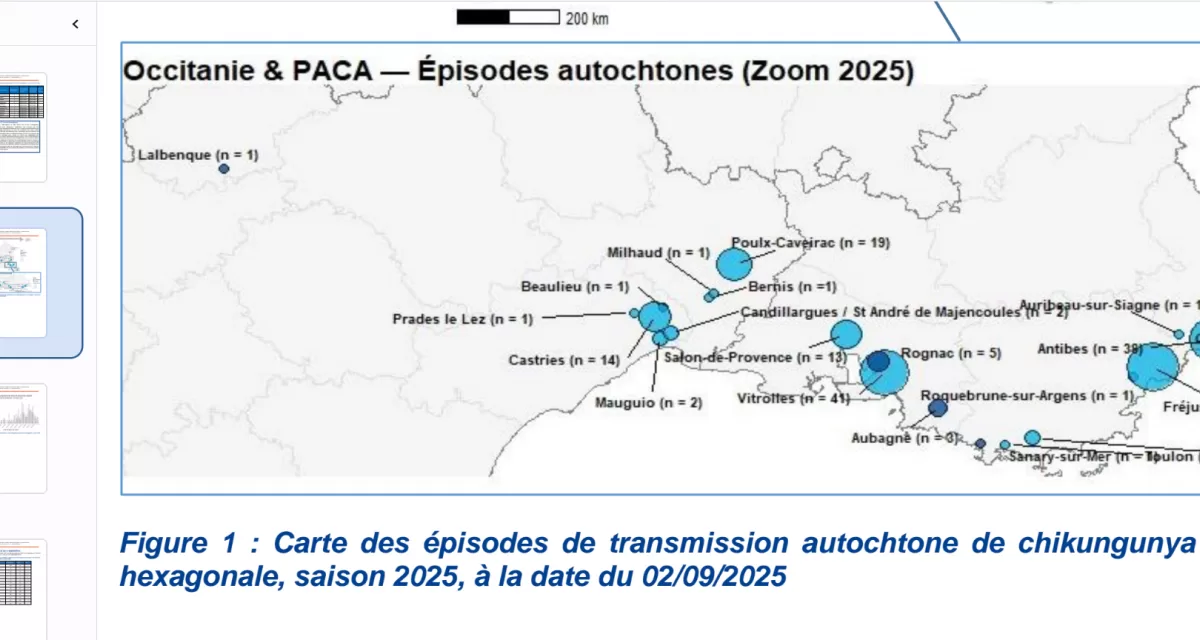
As of early September 2025, France’s Mediterranean coast has confirmed over 300 locally acquired cases of chikungunya, a mosquito-borne viral disease typically endemic to tropical regions. This outbreak, unprecedented in scale and geographic spread for mainland France, highlights growing public health challenges linked to climate change, insect vector expansion, and emerging infectious diseases in Europe. Health authorities continue intensified surveillance and control efforts to mitigate further spread, emphasizing prevention and traveler awareness.
Key Findings and Recent Developments
In 2025, France has experienced its largest recorded outbreak of chikungunya virus disease on the Mediterranean coast, with official reports confirming more than 300 locally transmitted cases by early September. Outbreak clusters have been identified across several southern regions including Provence-Alpes-Côte d’Azur, Corsica, Occitanie, Auvergne-Rhône-Alpes, Grand Est, and Nouvelle-Aquitaine. This marks a steep rise compared to previous years when local transmissions were sporadic and geographically limited. Multiple episodes are being actively investigated, with mosquito vector control measures underway in affected communities.
The virus is transmitted primarily by the Aedes albopictus mosquito, also known as the tiger mosquito, which has increasingly established itself in southern Europe. The surveillance data indicates that the outbreak’s timeline is also notable for an earlier start in the season than past years, with locally acquired cases appearing as early as June 2025.
Expert Commentary and Context
Dr. Caterina Rizzo, professor of hygiene and preventive medicine at the University of Pisa, comments, “The scale and early timing of the chikungunya outbreaks in France underline the shifting epidemiology of mosquito-borne diseases in Europe. Vector expansion driven by warmer climates and human mobility makes timely surveillance and public education vital.” She also notes that while chikungunya vaccines are approved and available in some countries, their current use in Europe is limited and focused mainly on travelers.
Jan C. Semenza, PhD, an epidemiologist at Umeå University, Sweden, highlights the role of climate change, stating, “Our research shows every 1°C rise in summer temperature increases outbreak risks by approximately 55%. We are likely to see increasing chikungunya outbreaks in southern Europe unless robust vector control and vaccination strategies are widely adopted.” He warns that countries like France and Italy are at heightened risk, reflecting the ongoing expansion of invasive mosquito species.
Disease Overview and Symptoms
Chikungunya is caused by a virus transmitted to humans through bites from infected Aedes mosquitoes. Symptoms usually appear 4 to 8 days after infection and include sudden fever, severe joint pain (often debilitating), rash, headaches, and muscle pain. While rarely fatal, the joint pain can persist for months, impacting quality of life. There is no specific antiviral treatment; management focuses on relieving symptoms through rest, hydration, and pain relief.
Public Health Implications
The outbreak underscores several public health concerns. First, the presence of sustained mosquito populations capable of virus transmission confirms that chikungunya is no longer confined to tropical climates but can establish itself in temperate zones under favorable conditions. This challenges traditional assumptions about vector-borne disease geography.
Second, public health authorities emphasize the need for community cooperation in eliminating mosquito breeding sites, such as standing water around homes, combined with municipal vector control programs. Surveillance includes screening suspected cases, reporting clusters, and educating the public on protective measures like using insect repellents and window screens.
Third, the outbreak highlights the importance of travel vaccination advice. The U.S. CDC and European health bodies recommend immunization for travelers visiting regions with active chikungunya transmission, although wider vaccine use for residents in outbreak zones remains limited.
Limitations and Counterarguments
While the outbreak is significant, some experts caution that chikungunya’s expansion may remain geographically restricted due to climatic and ecological limits on mosquito survival and virus replication. Additionally, available data may underreport mild or unconfirmed cases, complicating precise risk assessments.
Vaccination remains a complex issue; although vaccines exist, there are logistical and economic challenges in deploying mass vaccination campaigns, especially in non-endemic countries. Prevention efforts still primarily rely on vector control and public awareness.
What This Means for Readers
For residents and travelers in France and similar regions, heightened awareness and active prevention are critical. Using mosquito repellents, wearing protective clothing, and removing stagnant water are practical daily steps to reduce risk. Healthcare providers should consider chikungunya in patients presenting with compatible symptoms during mosquito season, including those without recent travel history.
Furthermore, the outbreak serves as a reminder of evolving infectious disease landscapes influenced by environmental change, urging continued investment in vector monitoring, vaccine research, and public health readiness.
Medical Disclaimer:
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: