Flu cases are surging across the United States as holiday travel and gatherings accelerate the spread, according to the latest data from the Centers for Disease Control and Prevention (CDC). Most states now report high or very high flu activity, with infections climbing faster than in recent seasons. Health officials urge vaccination and precautions amid estimates of millions already affected this 2025-2026 season.
Current Surge in Flu Activity
The CDC reports sharp increases in flu indicators nationwide, with clinical labs showing a 5% positivity rate for influenza, up from 2.9% the prior week. Outpatient visits for respiratory illnesses rose to 2.5% from 2.2%, exceeding baseline levels in many areas. Over 19,000 influenza-related hospitalizations occurred in the week ending December 20, a jump of about 10,000 from the previous week.
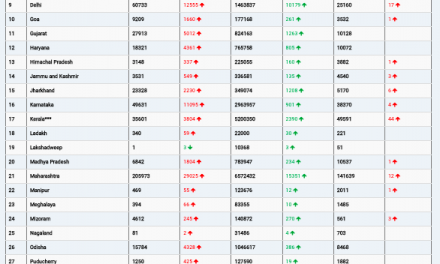
New York State recorded 71,123 flu cases that same week, the highest single-week total since mandatory reporting began in 2004—a 38% increase over the prior week. States like Louisiana, Colorado, and others face intense activity, driven by holiday mobility. CDC estimates place season totals at least at 7.5 million illnesses, 81,000 hospitalizations, and 3,100 deaths as of late December, with numbers expected to climb.
Dominant Strain and Viral Evolution
Influenza A(H3N2), particularly a variant called subclade K, dominates this season, accounting for roughly 92% of the 1,600 CDC-tested samples. This strain, circulating globally since summer, features mutations that may partially evade population immunity built from prior exposures or vaccines. Earlier Southern Hemisphere seasons hinted at its potential severity, though US vaccine matching remains reasonable despite some mismatch concerns.
Five additional pediatric deaths reported last week bring the season total to eight, highlighting risks for children. Older adults comprise over half of hospitalizations in preliminary data from prior patterns. Low severity indicators persist for now, but experts predict weeks of elevated activity ahead.
Expert Insights on Drivers and Outlook
“Holiday interactions are certain to facilitate transmission, and we have yet to observe any signs of a decrease in the acceleration of cases,” stated Cameron Wolfe, MD, professor at Duke University. Public health specialists link the uptick to holiday travel, suboptimal vaccination rates, and viral adaptations. Dr. Wolfe noted genetic sequencing shows mutations aiding immune escape, compounding factors like indoor gatherings.
“Flu is surging across the United States amid a busy holiday travel time,” aligns with CDC’s FluView, signaling the 2025-2026 season’s start. Vaccination distribution reached 130 million doses, yet uptake lags, per CDC. Experts like those at CIDRAP emphasize early antiviral treatment for high-risk groups to curb complications.
Public Health Context and Historical Comparison
This season follows the severe 2024-2025 flu period, with 43-73 million illnesses, 560,000-1,100,000 hospitalizations, and 38,000-99,000 deaths nationwide. Peak positivity hit 31.6% that year, the highest in nine seasons. Current hospitalization rates rank third-highest in 15 years at 6.9 per 100,000 early on.
Factors like waning immunity post-COVID and co-circulating viruses amplify risks. About 90% of pediatric deaths in recent seasons involved unvaccinated children, often with comorbidities. CDC recommends annual shots for all over 6 months, as they reduce severe outcomes even amid drift.
Practical Steps and Prevention Strategies
Vaccination remains the cornerstone, effective against hospitalization despite dominant H3N2. High-risk individuals—pregnant people, young children, elderly, and those with chronic conditions—should seek antivirals like oseltamivir within 48 hours of symptoms. Everyday actions include handwashing, masking in crowds, staying home when ill, and improving ventilation at gatherings.
For travelers, CDC advises checking local activity maps and delaying trips if symptomatic. Pharmacies offer rapid tests and vaccines; over 130 million doses ensure availability. These steps mirror successful containment in milder regions, potentially averting overload on hospitals.
Limitations and Balanced Perspectives
Data relies on voluntary reporting, potentially undercounting cases, as CDC models extrapolate from samples. Vaccine effectiveness varies yearly; subclade K may reduce protection slightly, though benefits persist. No evidence supports herd immunity thresholds met, and misinformation hampers uptake.
Conflicting regional patterns exist—some areas like Louisiana peaked early—urging localized vigilance. Experts caution against panic, noting severity remains low overall, but sustained rises could strain systems. Ongoing surveillance will refine predictions.
Implications for Healthcare and Daily Life
This surge burdens emergency departments, with hospitalizations doubling recent baselines in spots. Healthcare workers face burnout risks amid overlapping respiratory illnesses. For consumers, it means prioritizing flu shots now—clinics report ample supply—and monitoring symptoms like fever, cough, and fatigue.
Families should stock antivirals prescriptions preemptively if high-risk, and schools prepare for absenteeism spikes. Policymakers eye expanded access, as seen in prior seasons’ pediatric protections. Proactive measures could cap this at moderate severity.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Reuters. “Flu cases rise across US as holiday travel fuels spread.” December 31, 2025. https://www.reuters.com/business/healthcare-pharmaceuticals/flu-cases-rise-across-us-holiday-travel-fuels-spread-2025-12-31/reuters