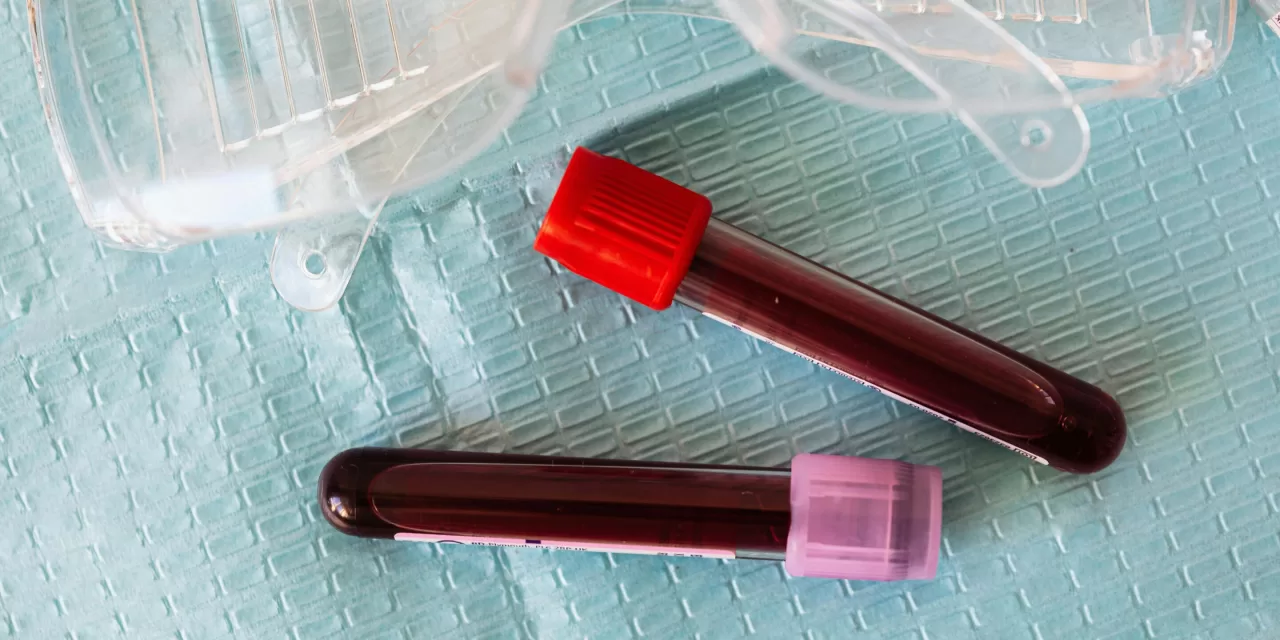
In a landmark development dated May 16, 2025, the U.S. Food and Drug Administration (FDA) approved the first blood test to aid in the diagnosis of Alzheimer’s disease. This innovation, known as the Lumipulse G pTau217/ß-Amyloid 1-42 Plasma Ratio test, offers a minimally invasive, accessible, and cost-effective alternative to traditional diagnostic tools such as positron emission tomography (PET) scans and lumbar punctures. The test is specifically authorized for adults aged 50 and older who display symptoms suggestive of Alzheimer’s disease, aiming to detect hallmark amyloid plaques and tau protein tangles associated with the condition earlier and more efficiently.
Key Findings and How the Test Works
Alzheimer’s disease diagnosis has historically depended on invasive or expensive methods. PET scans visualize amyloid plaques in the brain, while cerebrospinal fluid (CSF) analysis through lumbar puncture detects biomarkers. The Lumipulse blood test measures the plasma ratio of two proteins—phosphorylated tau (pTau217) and beta-amyloid 1-42—that correlate strongly with Alzheimer’s pathology. Analyzing these proteins in the blood allows clinicians to infer the presence of pathology within the brain with over 90% accuracy, on par with established methods.
Phosphorylated tau emerges as neurons begin to malfunction, leading to the characteristic tau tangles inside brain cells, while beta-amyloid forms toxic plaques outside neurons. These markers can develop years before cognitive symptoms appear. The blood test delivers results within approximately 2 to 5 days after a routine blood draw, potentially allowing earlier detection and intervention.
Expert Perspectives and Research Background
Jeff Dage, PhD, senior research professor of neurology at Indiana University School of Medicine and one of the key contributors in identifying phosphorylated tau as a biomarker, emphasized the test’s ability to expand diagnostic accessibility: “This offers a less invasive, more accessible method to identify Alzheimer’s pathology early in the disease process. It opens the door to earlier interventions and broader participation in clinical trials, crucial for advancing treatment”.
Maria C. Carrillo, chief science officer of the Alzheimer’s Association, highlighted the public health promise: “For too long, Americans have struggled to get a simple and accurate diagnosis; with today’s FDA action, it will be easier for individuals to receive an accurate diagnosis earlier”.
Neurology experts not involved in the development echoed this optimism. Dr. Howard Fillit, chief science officer at the Alzheimer’s Drug Discovery Foundation, stated the test “should be a game-changer” for timely, accurate diagnosis and improved patient care. Furthermore, Dr. Bernick from the Cleveland Clinic pointed out the test’s clinical utility in distinguishing Alzheimer’s from other causes of cognitive decline, such as strokes or Parkinson’s disease, and in speeding the recruitment process for clinical trials.
Context and Public Health Implications
Alzheimer’s disease afflicts about 11% of Americans aged 65 and older, numbering over 7 million cases, with projections doubling by 2050. Early and accurate diagnosis is pivotal to managing symptoms, care planning, and applying FDA-approved therapies that may slow disease progression.
Traditional diagnostic methods are limited by cost, invasiveness, and accessibility, especially in rural or underserved areas. The blood test’s simpler procedure—a routine blood draw—could enable broader screening in primary care settings, facilitating earlier detection when treatments might be most beneficial to slow decline. It may also help reduce misdiagnosis rates; currently, primary care physicians correctly diagnose Alzheimer’s approximately 60% of the time, whereas the blood test could raise accuracy above 90%.
Limitations and Balanced Perspectives
While groundbreaking, the Lumipulse blood test is not a standalone diagnostic tool; it is intended to be part of a comprehensive evaluation, including medical history, neurological exams, and cognitive testing. False positives and negatives remain potential challenges, and the test is currently limited to symptomatic adults aged 50 and above. Its utility in asymptomatic individuals or younger populations requires further research.
Experts caution that more longitudinal data is needed to understand fully how the test integrates with other biomarkers and clinical assessments in diverse populations. Insurance coverage is expected but not yet universal, possibly affecting equitable access initially.
What This Means for Readers and Patients
For individuals experiencing memory loss or cognitive symptoms, this blood test offers hope for earlier, easier diagnosis without undergoing costly or invasive procedures. Earlier detection may provide a critical window when existing treatments and lifestyle interventions have greater impact. It also means that patients can more confidently plan for their care and participate in clinical trials advancing future therapies.
Primary care providers, with access to this test, can improve diagnostic confidence and reduce delays traditionally experienced in Alzheimer’s diagnosis pathways. However, people should consult healthcare professionals for comprehensive evaluation, as no single test currently confirms Alzheimer’s disease conclusively.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.