A groundbreaking study published in October 2025 reveals that even individuals who appear healthy and have a normal body weight can harbor hidden fat deposits that damage arteries, significantly increasing their risk of cardiovascular disease. This research, led by scientists at McMaster University in Canada, challenges the conventional reliance on body-mass index (BMI) as the main indicator of cardiovascular risk and underscores the dangers of “hidden” visceral and liver fat in artery health.
Key Findings and Study Overview
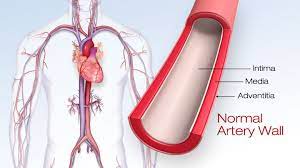
The study analyzed advanced MRI imaging data from more than 33,000 adults across Canada and the United Kingdom. Researchers specifically measured visceral fat, which accumulates deep inside the abdomen around organs, and hepatic fat deposited in the liver. They found a strong association between these fat types and the thickening and clogging of the carotid arteries in the neck, crucial blood vessels supplying the brain. Narrowing of these arteries is a known precursor to stroke and heart attack.
Importantly, the study demonstrated that even after adjusting for traditional cardiovascular risk factors such as high cholesterol and high blood pressure, visceral and liver fat independently contributed to arterial damage. Visceral fat was persistently linked to carotid artery plaque buildup and wall thickening, with liver fat showing a weaker but still significant effect.
“This study provides a wake-up call for both clinicians and the public,” said Russell de Souza, co-lead author of the study and associate professor at McMaster’s Department of Health Research Methods, Evidence, and Impact. “The presence of artery-damaging fat in people considered healthy by standard measures demands a shift in how we assess cardiovascular risk,” he emphasized.
Expert Perspectives
Dr. Marie Pigeyre, co-author and associate professor in the Department of Medicine at McMaster University, noted, “This research reveals that relying solely on BMI or outward appearance can miss a significant part of cardiovascular risk related to hidden fat deposits. Clinicians need to incorporate imaging and metabolic assessments when evaluating patients, even those without obvious obesity.”
Dr. Anita Kapoor, a cardiologist unaffiliated with the study, explained the significance: “Visceral and hepatic fat are metabolically active and contribute to inflammation, insulin resistance, and arterial plaque formation. This study highlights the silent danger these fats pose, especially to individuals who might be labeled ‘skinny fat’—normal weight but unhealthy fat distribution.”
Context and Background
Visceral fat is known to surround vital organs, promoting inflammation and metabolic disturbances. Similarly, fatty liver (hepatic steatosis) is increasingly recognized as a contributor to metabolic syndrome and cardiovascular disease. Previous research linked these fat deposits to Type 2 diabetes, hypertension, and heart disease, but their direct impact on artery health was less clear until now.
This study’s comprehensive approach leveraging MRI technology and a large participant base clarifies the pathways by which hidden fat damages arteries. It also sheds light on limitations of BMI, which cannot differentiate between lean mass, subcutaneous fat, and dangerous visceral fat layers.
Statistical Context
-
The study included data from about 33,000 adults—6,760 from Canada and 26,547 from the U.K.
-
Visceral fat showed a consistent positive correlation with carotid artery wall thickening and plaque presence.
-
Liver fat also had a statistically significant link, although less robust than visceral fat.
-
These findings persisted after controlling for cholesterol levels, blood pressure, age, sex, and other risk parameters.
Public Health Implications
This research underscores the need for greater awareness that normal-weight individuals can still be at high cardiovascular risk due to hidden fat accumulation. It suggests a need to revise standard screening protocols by integrating imaging methods to assess fat distribution, particularly in people with metabolic risk factors but normal BMI.
Practically, these findings support lifestyle interventions focusing on reducing visceral and liver fat through diet, exercise, and weight management, even for those who may appear slim. Monitoring metabolic health beyond simple weight metrics is crucial for early prevention of stroke and heart disease.
Limitations and Counterarguments
While the study is robust, some limitations include the observational design which cannot prove causation definitively. MRI imaging, though precise, is less accessible widely and costly. Future research might explore interventions specifically targeting visceral and hepatic fat reduction and their effects on arterial health.
Some experts caution that more randomized controlled trials are needed to confirm these findings and to refine screening guidelines. However, the accumulating evidence firmly establishes the role of hidden fat in cardiovascular risk.
Practical Advice for Readers
-
Maintain a balanced diet low in saturated fats and refined sugars to minimize visceral fat accumulation.
-
Regular physical activity helps reduce abdominal fat independent of changes in body weight.
-
Consult healthcare professionals for metabolic screening, especially if you have risk factors or a family history of heart disease.
-
Avoid relying solely on weight or BMI as a measure of cardiovascular health.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: