The World Health Organization (WHO) announced on January 26, 2026, that six countries in its European Region— the United Kingdom, Spain, Austria, Armenia, Azerbaijan, and Uzbekistan—have lost their measles elimination status due to ongoing outbreaks in 2024. This reversal, verified by the European Regional Verification Commission for Measles and Rubella Elimination (RVC) in September 2024 based on that year’s data, highlights a troubling resurgence of the highly contagious virus across the continent. With Europe reporting over 127,000 measles cases in 2024 alone—double the previous year’s total—the WHO is calling for urgent vaccination drives to protect vulnerable children.
Key Developments and Countries Affected
The RVC, an independent body assessing measles interruption for at least 36 months, revoked elimination status after confirming endemic transmission in these nations. In the UK, 2,911 confirmed cases were recorded in England in 2024, the highest since 2012, with around 3,600 suspected cases across England and Wales. Spain, Austria, and others followed suit, while 13 additional countries like France, Germany, Italy, Poland, and Romania now face endemic measles.
Europe’s 2024 outbreak marked the highest case count in over 25 years, surpassing 127,320 confirmed infections, with children under 5 comprising over 40% and more than half requiring hospitalization. Romania reported 30,000 cases and Kazakhstan 28,000, driving the regional surge. Only 32 of 53 WHO European member states (60%) maintain measles elimination, down from prior highs.
Causes: Declining Vaccination Rates
Measles elimination demands at least 95% coverage with two doses of measles-containing vaccines (like MMR) at national and subnational levels. Yet, the UK achieved just 84.4% for two doses in children by 2024, with regional lows like London exacerbating risks. Broader European data shows an average first-dose coverage of 90% in 2024, but many nations fall short, including the UK at 89%.
Pandemic disruptions, vaccine hesitancy, and misinformation fueled this backslide, with 500,000 children missing their first dose in 2023 alone. In unvaccinated cases (87% of 2024 EU/EEA reports), outbreaks spread rapidly in under-immunized communities. Experts link post-COVID skepticism to rebounds in vaccine-preventable diseases.
Expert Commentary
“This change reflects a broader challenge we’re facing across the WHO European Region,” a WHO spokesperson stated, noting immunity gaps alongside antimicrobial resistance as key threats. Dr. Helena Kasstan-Dabush, an anthropologist at the University of Durham not involved in the verification, commented: “Sustained measles transmission reflects a decade-long decline in routine vaccination coverage… Profoundly low coverage in areas such as Hackney underscores the unequal distribution of risk and harm to children.”
The UK Health Security Agency (UKHSA) emphasized: “Elimination can only be achieved… by improving coverage of the MMRV vaccine in children to meet the WHO 95% target and by using all opportunities to catch up older children and adults.” Dr. Simon Williams, a public health expert from Swansea University, added via Science Media Centre: “It is unsurprising the UK has lost its WHO measles elimination status, following nationwide outbreaks since 2024.”
Background on Measles and Elimination Efforts
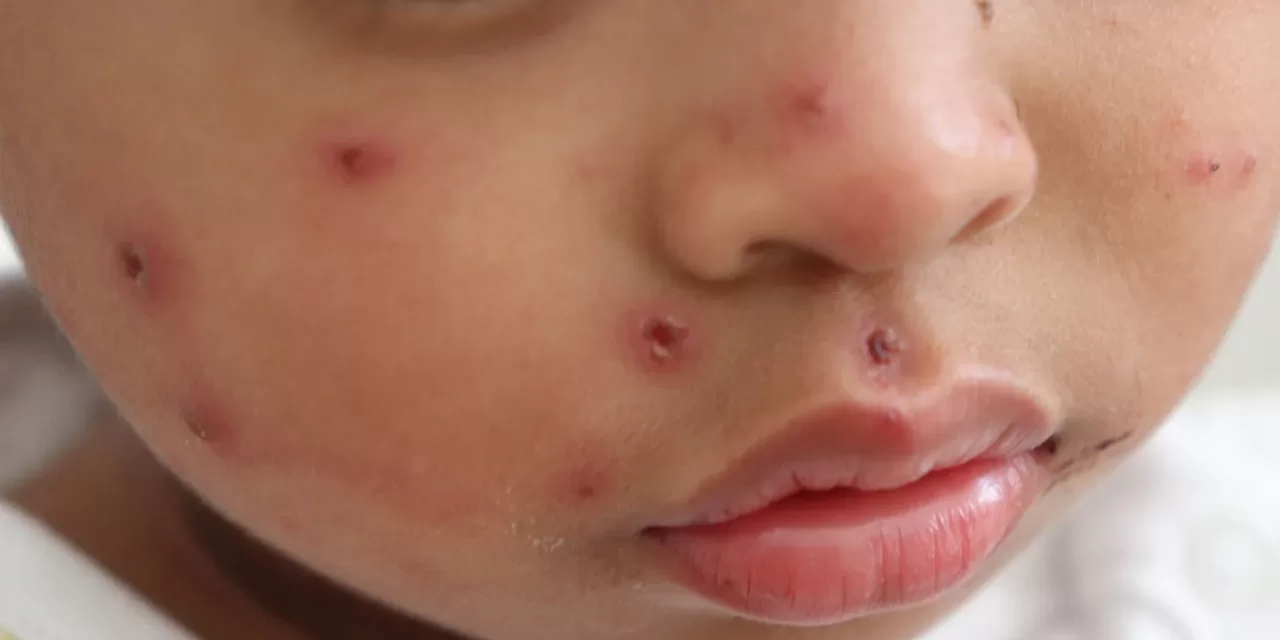
Measles, a paramyxovirus spread via respiratory droplets, causes fever, cough, rash, and potentially severe complications like pneumonia, encephalitis, or death—especially in young children. One infected person can transmit to 12-18 others in susceptible groups, making herd immunity critical. The WHO European Region targeted elimination via the European Immunization Agenda 2030, building on progress where cases fell to 4,440 in 2016.
Gains reversed post-2018-2019 outbreaks (89,000 and 106,000 cases) and COVID-19 setbacks, with 38 deaths reported in 2024 preliminary data. Globally, Europe accounted for a third of cases last year, mirroring losses like Canada’s in 2025.
Public Health Implications
This setback endangers children, with over 40% of cases in under-5s and hospitalization rates exceeding 50%. Unvaccinated individuals face highest risks, but outbreaks strain healthcare, diverting resources from other needs. For the public, it signals urgency: parents should verify two-dose MMR status (typically at 12-15 months and 3-5 years), and adults born post-1970 may need boosters.
Governments must launch catch-up campaigns, targeting low-uptake areas like London’s Hackney. Success stories, like Hungary and Portugal sustaining 95%+ coverage, show it’s achievable with sustained efforts.
Limitations and Counterarguments
While data is robust, verification relies on self-reported surveillance, potentially undercounting cases in low-testing areas. Some argue regional disparities (e.g., urban vs. rural) complicate national metrics, and migration adds imported cases. Critics of mandates highlight access barriers over hesitancy, though evidence points to both.
No evidence suggests vaccine safety issues; side effects are rare and mild compared to measles risks. The RVC notes 92% rubella elimination success, proving strategies work when applied.
This development underscores that elimination is fragile without vigilance. Boosting uptake to 95% could restore status within 36 months, protecting future generations.
References
-
Reuters. “European countries including UK lose measles elimination status.” January 26, 2026. https://www.reuters.com/business/healthcare-pharmaceuticals/european-countries-including-uk-lose-measles-elimination-status-2026-01-26/[reuters]
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.