NEW DELHI — In a move that could redefine the landscape of hematological care in India, a coalition of leading medical experts, legal authorities, and patient advocates has issued an urgent call for systemic reforms to the nation’s blood transfusion infrastructure. The group is demanding the enactment of a national “Blood Safety Act” and the universal implementation of advanced screening technologies to protect thousands of patients who rely on regular transfusions for survival.
The initiative was spearheaded by the Thalassemia Patients Advocacy Group (TPAG), which released a comprehensive position paper on Wednesday. The document outlines a roadmap for eliminating preventable risks—specifically Transfusion-Transmitted Infections (TTIs) like HIV, Hepatitis B, and Hepatitis C—that continue to haunt the most vulnerable segments of the patient population.
The Invisible Threat: The “Window Period” Risk
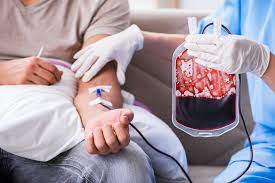
For patients with thalassemia—a genetic blood disorder where the body doesn’t make enough hemoglobin—life is measured in units of blood. Most require transfusions every two to four weeks. However, the very treatment that sustains them often carries a hidden peril.
Currently, many blood banks in India rely on ELISA (Enzyme-Linked Immunosorbent Assay) testing. While effective, ELISA has a significant “window period”—the time between when a donor is infected and when the test can actually detect antibodies or antigens.
“For individuals who require lifelong transfusions, gaps in screening protocols are not just a medical oversight; they are a fundamental threat to survival and dignity,” the expert panel stated in the paper.
To bridge this gap, the experts are calling for the universal adoption of Nucleic Acid Testing (NAT). Unlike traditional methods, NAT detects the genetic material (DNA or RNA) of a virus, significantly shortening the window period. For example, NAT can detect HIV as early as 5–10 days after infection, compared to the 20-plus days often required by older screening methods.
A Call for Uniformity: The Proposed Blood Safety Act
One of the most significant hurdles in India’s current system is its fragmented nature. Blood safety regulations often vary by state, and the lack of a centralized, enforceable law leads to uneven quality of care.
P.C. Sen, a Senior Advocate at the Supreme Court of India and a contributor to the paper, emphasized that blood safety is a constitutional responsibility. The group is lobbying for a National Blood Safety Act that would:
-
Codify Patient Rights: Explicitly state the right of every patient to receive screened, safe blood.
-
Standardize Screening: Mandate NAT testing across all blood banks, whether private or public.
-
Ensure Accountability: Create a legal framework to hold institutions responsible for preventable infections.
“We need to move blood safety from the margins to the mainstream of healthcare governance,” said Deepak Chopra, Mentor of the TPAG. “Our position paper is a call to place patient lives at the center of policy.”
Bridging the Rural-Urban Divide
The experts highlighted a stark disparity in blood safety between urban centers and rural regions. While premier hospitals in metropolitan areas often utilize NAT, rural blood banks—where a significant portion of the thalassemia population resides—frequently lack the infrastructure or funding to implement advanced diagnostic technologies.
Prof. N.K. Ganguly, former Director-General of the Indian Council of Medical Research (ICMR), noted that the lack of a dedicated National Thalassemia Control Programme contributes to this inequity. Such a program would integrate prevention, screening, and long-term care into a single, federally funded initiative, ensuring that a child in a remote village receives the same quality of blood as one in a capital city.
Expert Perspectives: A Preventative Approach
Independent medical professionals echo the urgency of the TPAG’s findings. Hematologists note that treating a patient who has contracted Hepatitis C through a transfusion is far more expensive and taxing on the healthcare system than the cost of a NAT-screened blood bag.
“The cost of NAT is often cited as a barrier, but we must look at the ‘cost of inaction,'” says Dr. Aruna Singh, a hematology consultant (not involved in the paper). “Treating chronic viral infections and the subsequent liver or immune complications involves lifelong costs. Screening is a one-time preventative investment that saves lives and money.”
Challenges and Counterarguments
While the call for NAT is scientifically sound, some public health analysts point to the logistical challenges of universal implementation.
-
Infrastructure: NAT requires sophisticated laboratory equipment and stable power supplies, which can be challenging in underdeveloped regions.
-
Cost: The cost per unit of blood increases with NAT. Critics argue that without heavy government subsidies, this cost might be passed down to patients who are already financially burdened.
-
Donor Base: There are also concerns that stricter screening could initially lead to a higher rate of “false positives” or discarded units, temporarily straining an already thin blood supply.
The TPAG paper addresses these concerns by arguing for a phased implementation and government-backed “hubs” where smaller blood banks can send samples for centralized NAT testing, thereby reducing the need for every facility to own expensive machinery.
What This Means for Patients and Families
For families living with thalassemia, these reforms represent more than just policy changes—they represent peace of mind. Currently, many parents live in fear that the next transfusion could trade their child’s anemia for a chronic viral infection.
“Safe, timely, and equitable access to blood is not a luxury,” the paper concludes. “It is a foundational pillar of India’s healthcare infrastructure.”
Key Recommendations from the Position Paper:
-
Mandatory NAT Testing: To minimize window-period infections nationwide.
-
National Thalassemia Control Programme: To standardize care from birth through adulthood.
-
Transparency: A digital tracking system for blood units to ensure accountability from donor to recipient.
References and Sources
- https://www.newkerala.com/news/a/health-experts-advocates-call-systemic-reforms-protect-transfusion-dependent-176.htm
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.