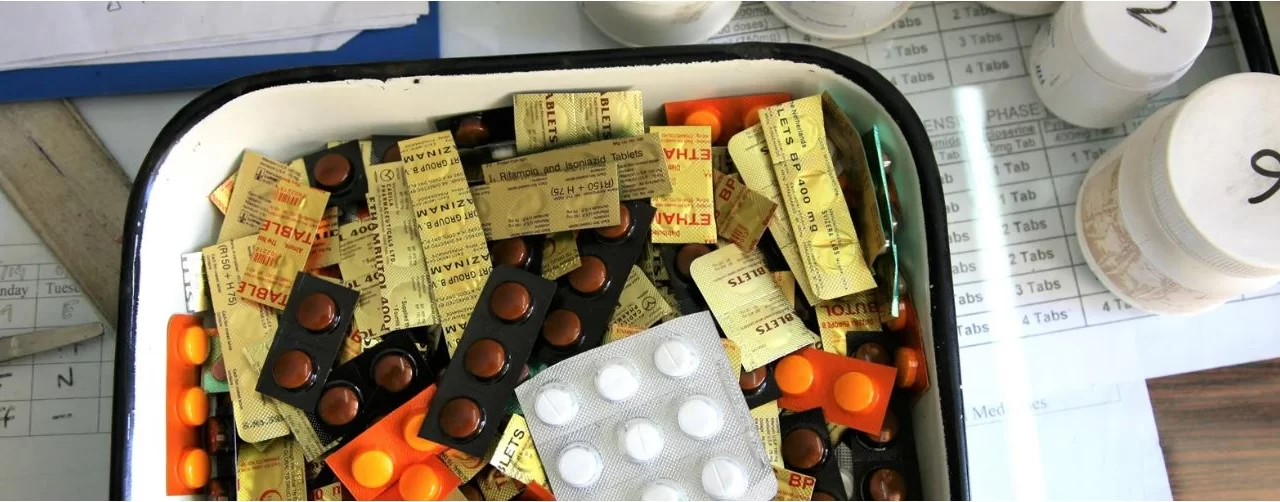
Early action against antimicrobial resistance (AMR) is critical to ensuring that infections remain treatable and that surgical procedures stay safe, according to the World Health Organization (WHO). AMR, the resistance of microbes to antimicrobial drugs, is currently causing over a million deaths annually worldwide and threatens the core foundations of modern medicine by making common infections harder to treat. The burden of AMR is particularly severe in low- and middle-income countries and regions such as South-East Asia and the Eastern Mediterranean.
The WHO highlights that rising AMR jeopardizes decades of medical progress, impacts essential treatments, and puts enormous strain on healthcare systems globally. Surgical site infections (SSIs), which can complicate surgeries ranging from cesarean sections to gastrointestinal procedures, are increasingly caused by resistant bacteria, raising the risk of postoperative complications and antibiotic treatment failures. For example, antibiotic-resistant Escherichia coli and Staphylococcus aureus—the leading pathogens causing postoperative infections—have challenged the effectiveness of surgical antibiotic prophylaxis, a key measure to prevent infections during surgery.
To address this, the WHO has emphasized the need for immediate and coordinated action that includes strengthening surveillance systems, promoting responsible use of antimicrobials, improving infection prevention and control (IPC) practices, and fostering innovation in diagnostics, treatments, and vaccines. The new Regional Roadmap on AMR for South-East Asia (2025–2030) endorsed by member states underscores the importance of national leadership, sustainable financing, multisectoral partnerships, and a One Health approach—including human, animal, and environmental health—to effectively combat AMR.
Experts stress the practical implications of these findings for public health and daily health decisions: preventing infections through hygiene and safe surgical practices limits the need for antibiotics, which helps slow resistance development. Careful antibiotic prescribing guided by local data and rapid diagnostics reduces unnecessary exposure. In addition, investment in laboratory capacity and community initiatives are vital, especially in regions facing unique healthcare challenges.
However, there are limitations and challenges. Vaccine development against key surgical pathogens like Staphylococcus aureus has proven difficult, and the landscape of pathogen resistance is continuously evolving. The capacity to implement evidence-based guidelines varies widely between countries, and suboptimal compliance contributes to resistance. Surveillance data gaps, especially in underserved areas, hinder timely responses.
In conclusion, combating AMR requires urgent, coordinated, and sustained global action with a focus on prevention, surveillance, stewardship, and innovation. Without this, the effectiveness of antibiotics and safe surgery practices will continue to decline, risking public health worldwide.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: