Delhi, Aug. 28, 2025 – A new international study has uncovered compelling evidence that dormant bacteria hiding inside arterial plaques may significantly contribute to the onset of heart attacks. The discovery, led by researchers from Tampere University in Finland in collaboration with UK colleagues, challenges the long-standing belief that heart attacks are solely the result of cholesterol build-up and arterial blockages.
Findings published this month in the Journal of the American Heart Association point to bacterial biofilms—dense, sticky colonies of microbes—as hidden culprits that may lie dormant in atherosclerotic plaques for years before suddenly contributing to plaque rupture and myocardial infarction (heart attack).
“These biofilms are gelatinous, long-lasting colonies of bacteria that are invisible to the immune system and resistant to antibiotics,” explained lead author Professor Pekka Karhunen, a pathologist at Tampere University. “Once reactivated, they can create bursts of inflammation that destabilize plaque walls.”
What the Study Found
The study examined arterial tissues collected from individuals who had died of sudden cardiac events. Using specialized antibodies, researchers detected bacterial DNA and evidence of biofilm structures within atherosclerotic plaques. Many of these bacteria were traced back to the human mouth, particularly species associated with periodontal (gum) disease.
The proposed mechanism is striking:
-
Atherosclerotic plaque formation: Traditionally thought to arise mainly from oxidized LDL cholesterol deposits, these plaques also harbor bacterial colonies.
-
Dormancy within biofilms: The bacteria remain protected inside a biofilm “gel,” shielded from immune surveillance and antibiotics.
-
Reactivation trigger: When a person faces another infection—such as influenza or pneumonia—or experiences systemic inflammation, the dormant biofilm can “switch on.”
-
Plaque instability: The resulting inflammation weakens the fibrous cap surrounding the plaque.
-
Heart attack onset: If the cap ruptures, it can trigger a blood clot, blocking blood flow to the heart muscle and causing a myocardial infarction.
This new line of evidence suggests that bacterial infections—especially oral bacterial infections—could act as silent accomplices in heart disease.
Why This Matters
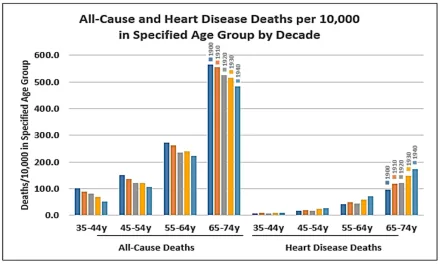
Heart disease, including heart attacks, remains the leading cause of death worldwide, claiming an estimated 17.9 million lives annually, according to the World Health Organization (WHO). For decades, prevention strategies have primarily focused on lowering cholesterol, controlling blood pressure, and promoting lifestyle changes.
If confirmed by further studies, this bacterial connection could broaden prevention and treatment strategies.
Karhunen and his team envision possible interventions in the future, including:
-
Diagnostic tools to detect bacterial activity in arterial plaques before symptoms appear.
-
Targeted therapies aimed at dismantling biofilms or modulating the immune response.
-
Even vaccines designed to prevent bacterial colonization of arterial walls.
Expert Perspectives
Dr. Anjali Menon, a cardiologist at All India Institute of Medical Sciences (AIIMS), New Delhi, who was not involved in the study, sees this as an important new piece in the puzzle:
“We have long observed links between poor oral health and cardiovascular risk. This study strengthens that association with biological evidence. While cholesterol and lifestyle remain crucial factors, infections may be playing a larger role than previously recognized.”
However, she cautions against premature conclusions:
“We’re not at a stage where we can say treating gum disease will automatically prevent heart attacks. More longitudinal studies are needed to establish cause and effect.”
The Oral Health Connection
The study also underscores the importance of oral hygiene. Oral bacteria such as Porphyromonas gingivalis—a key player in periodontal disease—can enter the bloodstream during bleeding gums and dental infections.
The American Heart Association (AHA) has previously acknowledged associations between gum disease and heart disease but emphasized the need for more definitive data. This new study provides a possible biological mechanism connecting the two conditions.
Dr. Rajiv Gupta, professor of microbiology at PGIMER Chandigarh, notes:
“Bacteria do not simply invade the heart. They find niches, create protective layers, and then strike when systemic defenses are low. If confirmed, these findings may shift oral care from being viewed as just a dental matter to one of public cardiovascular importance.”
Implications for Public Health
If bacterial biofilms truly contribute to the risk of sudden plaque rupture:
-
Preventive strategies might expand to include infection control—such as maintaining oral health, timely treatment of bacterial infections, and even developing anti-biofilm therapies.
-
Risk assessment tools could someday incorporate biomarkers for bacterial activity in plaque, alongside cholesterol and inflammatory markers.
-
Treatment guidelines may eventually need to integrate antimicrobial or vaccine-based strategies, though this remains speculative.
A Word of Caution
While the research is compelling, it comes with caveats:
-
The study primarily examined arterial samples from deceased patients rather than following living populations over time.
-
Causality has not been proven—bacteria might accelerate plaque rupture, but they may not be the primary driver in all cases.
-
Standard cardiovascular risk factors such as smoking, obesity, hypertension, and high cholesterol remain strongly established and should not be overlooked.
“This is exciting science, but the road from discovery to clinical application is long,” cautioned Dr. Menon. “People should not neglect lifestyle modifications in the hope of a future vaccine. That future may take a decade or more to arrive.”
Key Takeaways for Readers
-
Oral health matters for the heart: Brushing, flossing, and regular dental visits may reduce systemic bacterial load.
-
Stay vigilant about infections: Promptly treating bacterial infections could potentially reduce systemic inflammation.
-
Core prevention remains unchanged: A healthy diet, regular exercise, not smoking, and managing cholesterol and blood pressure are still the most reliable ways to lower heart attack risk today.
References
- https://www.daijiworld.com/news/newsDisplay?newsID=1290593
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.