A groundbreaking study from Stanford Medicine has illuminated the role of “creeping fat”—an abnormal expansion of mesenteric fat surrounding the intestines—as a direct driver of intestinal scarring in Crohn’s disease (CD). Published in September 2025, this research reveals that creeping fat is not merely a bystander but actively contributes to the debilitating fibrotic strictures that complicate Crohn’s disease, underscoring new possibilities for targeted treatments to prevent intestinal scarring and improve patient outcomes.
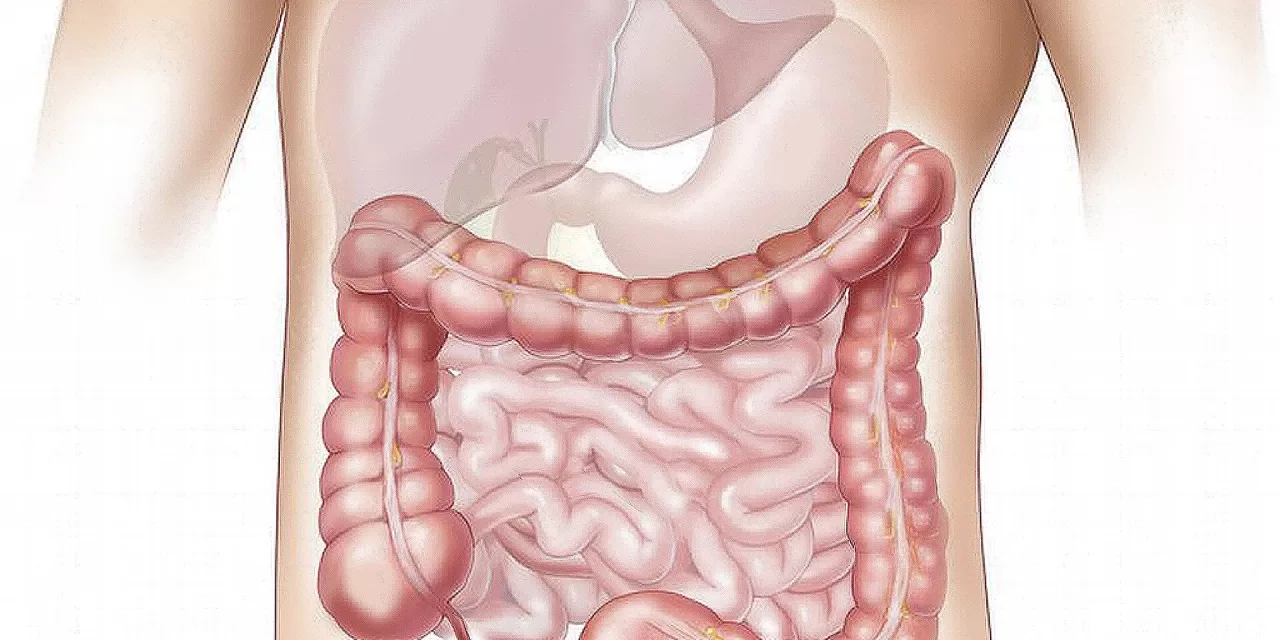
Crohn’s disease is a chronic inflammatory condition of the gastrointestinal tract that often leads to complications like strictures—narrowings in the intestine caused by fibrotic scar tissue. These strictures frequently require surgical intervention, as no effective therapies currently exist to halt or reverse scar formation. Creeping fat, characterized by finger-like deposits of thickened mesenteric adipose tissue encasing diseased bowel, has long been associated clinically with strictures, but its precise role had remained unclear until now.
The Stanford team analyzed tissue samples from more than 400 Crohn’s patients, using advanced spatial transcriptomics and ultrastructural methods to create detailed maps of fibroblast activity at the interface between the creeping fat and intestinal wall. They discovered that fibroblasts within creeping fat express a protein called collagen triple helix repeat containing 1 (CTHRC1), which plays a key role in tissue remodeling. These cells migrate into border regions between the fat and bowel where they produce large quantities of collagen, promoting fibrotic scar formation through the activation of the YAP/TAZ signaling pathway.
To validate these findings, researchers developed a novel mouse model replicating the creeping fat and intestinal fibrosis seen in human Crohn’s disease. By genetically disabling the YAP/TAZ pathway in creeping fat fibroblasts, they significantly reduced scar tissue formation and fat wrapping around the intestines in mice, demonstrating a causal relationship between creeping fat activity and fibrosis.
Dr. Jeong Hyun, assistant professor of pediatric surgery at Stanford and co-senior author, emphasized the clinical significance: “My patients suffer not only physically but emotionally from unpredictable flare-ups and the need for repeated surgeries. Identifying molecular targets in creeping fat offers hope for treatments that could prevent strictures, potentially transforming Crohn’s disease management.”
Crohn’s disease fibroblasts in creeping fat respond sensitively to mechanical strain from intestinal inflammation and stretching, ramping up extracellular matrix (ECM) production that builds fibrotic scar tissue. This mechanosensitive behavior mirrors scar formation processes in other tissues like skin, reinforcing the concept that creeping fat fibroblasts actively drive fibrosis rather than being passive participants.
Implications for public health are considerable. Strictures affect 70% to 90% of Crohn’s patients and frequently require surgical removal of affected intestine segments. Repeated surgeries diminish intestinal length, increasing risks such as malabsorption and requiring lifelong management. Developing drugs targeting creeping fat fibroblast pathways could reduce reliance on surgery, improve quality of life, and limit healthcare costs related to chronic Crohn’s complications.
However, experts caution that translating these findings into human therapies will require further research. Dr. Michael Longaker, the other senior author and a surgeon at Stanford, highlighted current limitations: “While this model is promising, human Crohn’s disease is complex, involving immune dysregulation, microbiome factors, and genetics alongside fibrosis. Therapies will need to be tested rigorously for safety and efficacy.”
In addition, creeping fat exhibits immunological activity contributing to intestinal inflammation through cytokine secretion and interactions with the mucosal immune system, complicating the picture. These multifaceted roles require integrative approaches in future treatments.
For individuals living with Crohn’s disease, these findings underscore the importance of ongoing research and the potential for advances in personalized medicine targeting fibrotic mechanisms. Maintaining regular follow-ups with healthcare providers and adherence to prescribed therapies remain critical for managing symptoms and monitoring complications.
This study enriches scientific understanding of Crohn’s disease pathology and offers an optimistic outlook toward novel therapeutic strategies that interrupt scar formation and improve patient care.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: