The Indian Supreme Court on October 10, 2025, dismissed a Public Interest Litigation (PIL) petition seeking a Central Bureau of Investigation (CBI) probe into the deaths of more than 20 children in Madhya Pradesh and Rajasthan after consuming toxic cough syrup. The court’s rejection came despite widespread public concern over the deaths linked to the contaminated medication, highlighting the ongoing challenges in drug safety regulation in India and the limits of judicial intervention in public health crises.
Key Developments and Findings
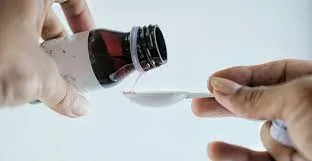
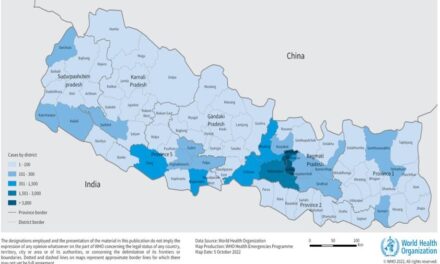
The deaths, primarily in Madhya Pradesh’s Chhindwara district and parts of Rajasthan, have been associated with the use of a cough syrup called Coldrif, manufactured by Sresan Pharmaceuticals in Tamil Nadu. Investigations revealed the syrup was contaminated with dangerously high levels of diethylene glycol (DEG), a toxic industrial chemical used in antifreeze and brake fluid but which is deadly if ingested. Tests found levels of DEG in the syrup at 48.6%, far exceeding the 0.1% permissible limit defined by Indian and World Health Organization (WHO) standards.
Since the crisis emerged in late September and early October 2025, Sresan Pharma’s owner, 73-year-old G. Ranganathan, was arrested by police in Chennai. The Tamil Nadu government revoked the manufacturing license of Sresan Pharma and sealed the factory. Several states have banned Coldrif and two other cough syrups—Respresh and ReLife—after they also tested positive for diethylene glycol contamination. Authorities have ordered recalls and removal of these products from markets.
Despite strong public interest petitions, the Supreme Court bench headed by Chief Justice B. R. Gavai refused to entertain the PIL filed by advocate Vishal Tiwari, citing ongoing investigations by state governments. Solicitor General Tushar Mehta emphasized that states like Madhya Pradesh and Tamil Nadu are capable of managing inquiries and taking effective steps. The bench expressed concern about the frequency of PILs filed by the petitioner based on media reports.
Expert Perspectives and Regulatory Context
The deaths have reignited calls from medical and regulatory experts for stringent enforcement of pharmaceutical safety standards in India’s vast drug manufacturing sector. The presence of diethylene glycol in medicines, a recurring problem historically in India and some other countries, reflects inadequate quality control, weak regulatory oversight, and failures in testing raw materials and final products before market release.
Dr. Praveen Soni, a pediatrician initially involved in the case, was charged with negligence due to prescribing the syrup; however, many medical associations and experts underscore that the primary responsibility lies with regulatory agencies for lapses in ensuring drug safety. An inspection by the Tamil Nadu Drug Control Department found Sresan Pharmaceuticals violated 364 manufacturing norms, including critical deficiencies in personnel qualification, quality assurance, water quality, and sanitary conditions at production facilities.
The World Health Organization has flagged serious concerns about India’s pharmaceutical regulatory gaps, especially with the risk of such toxic medicines possibly entering international markets via unregulated distribution. WHO and Indian regulators have urged more vigilance, especially concerning pediatric formulations, with some states banning all cough and cold syrups for children under two years.
Implications for Public Health and Recommendations
This tragedy highlights urgent needs for systemic reforms in India’s drug safety protocols, such as mandating independent testing of pharmaceuticals by accredited labs and establishing national expert committees to oversee quality control in medicines, with special attention to pediatric drugs. Consumers and healthcare providers must be educated about potential risks in unregulated medicines and encouraged to verify drug sources.
For parents and caregivers, the incident underscores caution in administering over-the-counter cough syrups, especially to young children, who are more vulnerable to toxic exposures. Consulting qualified healthcare professionals before using medicines and sourcing drugs only from trusted suppliers is crucial.
Potential Limitations and Balanced View
While the PIL sought a centralized probe by the CBI to ensure impartiality, the Supreme Court deferred to states’ authority, reflecting the complexity of jurisdiction in India’s federal system. The court did not find sufficient grounds to intervene in ongoing investigations. However, critics argue that state-level inquiries risk fragmented accountability in such public health disasters.
Moreover, the recall and ban actions are reactive measures; preventive regulatory reforms require political will and investment in monitoring capacities. Some experts worry that without systemic changes, similar incidents may recur.
Conclusion
The recent cough syrup deaths reveal deep vulnerabilities in India’s pharmaceutical safety mechanisms, with tangible consequences for child health and public trust. While legal avenues for intervention face hurdles, the case underscores an urgent call for comprehensive reform, diligent enforcement, and greater transparency to safeguard consumers—especially children—from toxic medicines.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References